Successful outcome of dental restorative procedures depends on a number of factors. A few factors are structural whereas others are implemented during the treatment procedure. The factors include adequate tooth preparation, geometry of framed tooth, surface roughness of the tooth, as well as intaglio surface of restoration and cementing agents [1]. To enhance bond strength between adhesive cement and casting, a rough and a contamination-free surface is essential [1]. Due to lack of ideal tooth preparation form, surface treatment of intaglio surface may have clinically relevant correlations with the retentive strength of castings thus eliminating the need for extensive procedures [2]. Improvement of bond strength in intaglio surface of restoration can be accomplished by various surface modalities such as airborne-particle abrasion with alumina, glass beads, metal primers, lasers, and a combination of these [3]. Among these, airborne-particle abrasion is a sensitive and inexpensive technique in fabricating a roughened alloy surface [4]. Intaglio surface refers to internal surface of casting which has main role in retention. It should clearly duplicate external surface of prepared tooth. Sandblasted, etched, surface treated intaglio surface provide micro-mechanical retention. Metal primer treated intaglio surface provides chemical retention [2].
Adhesion of resins to the substrate depends upon both physico-chemical bonding and micro-mechanical interlocking [5]. Innovation of metal primers has improved bond strength of resin cements to dental alloys, which provides micro-mechanical retention as well as chemical bonding [4]. Metal primers and some resin cements have active monomers that create a strong chemical bond between resin-based materials and oxides present on the metal surface. Metal primers have shown to be effective on noble alloys [6]. There is a lack of evidence about their effect on base metal alloys. Hence, studies investigating the effect of metal primers on retention of base metal alloys are required [4]. Glass Ionomer Cement (GIC) is the most commonly used conventional luting agent for cementation of fixed dental prosthesis. Chemical adhesion to tooth structure, good translucent properties, and ideal cariostatic potential has made GIC an extremely definitive luting agent [7]. To overcome the drawbacks of conventional luting cements, Resin-Modified Glass Ionomer (RMGI) and resin-based luting agents were introduced which revolutionised the restorative techniques. A dual-cure hybrid, higher flexural strengths, fluoride release from the cement, and ease of handling are the advantages of RMGI compared to conventional GICs [7]. Good strength, multiple substrate adhesion, insolubility in oral conditions and esthetic potential have made resin based luting agents as an appropriate choice for fixed dental prosthesis. Resin cements are preferred mostly when the preparation lacks optimal retention and resistance forms [8].
Null hypothesis states that surface treatment of intaglio surface does not have any effect on retention of complete cast crowns. In the current in-vitro study, an attempt was made to compare and evaluate the effect of surface treatment of intaglio surface with sandblasting and metal primer on retention of complete cast crowns cemented with different luting cements. The effect of metal primers on noble alloys has been studied several times and proved to be efficacious but there is insubstantial information about their effect on base metal alloys hence, this study was conducted to study effect of metal primer on base metal alloys.
Materials and Methods
The current in-vitro experimental study was conducted at three centers: Department of Prosthodontics, KLES VK Institute of Dental Sciences; SDM Dental College, Dharwad; Belgaum Material Testing Centre, Belagavi, Karnataka. The study was conducted in September 2015 over duration of 3 months.
A total of 50 extracted sound human maxillary first premolar teeth with healthy and intact surfaces were chosen for the study (extracted for orthodontic treatment). Sample size calculation was done by formula, where δ is standard deviation, E is error rate, 1.96 is 95% confidence
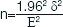
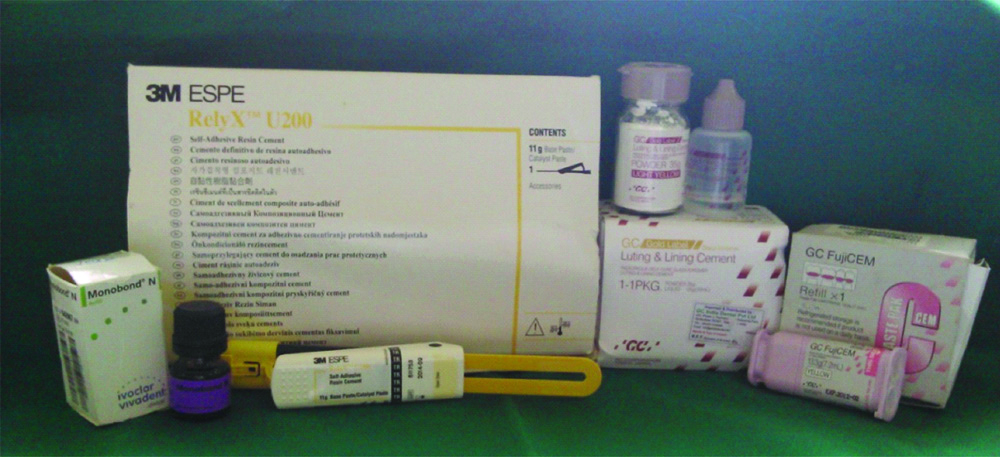
Extracted teeth were collected from Department of Oral Surgery over period of one week. Once collected; the adhering soft tissue and the blood were cleaned under running water and stored in a closed container containing artificial saliva until use [9-11]. Selected teeth were divided randomly into three groups. Each group was luted with three luting cements-GIC (10) (GC Gold Label, GC corp, Tokyo Japan), RMGI (20) (GC FugiCEM, GC Corp, Tokyo Japan), and resin cement (20) (RelyxTM U200, 3M ESPE, Germany). Ethical clearance was not obtained as study (in-vitro) conducted did not involve any living subjects [Table/Fig-1].
Materials used in the present study.
Horizontal notches were positioned on roots of every tooth for retention and centered in index using an autopolymerising acrylic resin [12]. (DPIRR, Cold CureBatch no: 4156) specimen preparations were done by a single operator. A jig was held firmly on surveyor base and crown preparations were made with a high-speed hand piece and stabilised by using a k-9 crown installation machine at the desired taper [13,14]. To frame axial surfaces and establish a finish line, parallel-sided course diamond points with rounded tip were used [12]. With the hand piece held at intended taper, tooth preparation was done by moving base of the surveyor against the diamond bur. Occlusal surface of the teeth was made flat [4,15], parallel to the floor, and occlusocervical dimension of the teeth was standardised at 4 mm for all the samples [1,16]. A new bur was used for every test group [Table/Fig-2,3] [17].
Specimen held on the surveyor base and placed over K-9 crown installation device for tooth preparation.


Crown preparation with taper of 6° was achieved for all the specimens by tilting the hand piece to their respective degree. A small indexing groove was made using carbide bur to establish path of insertion for seating [16]. Tooth preparations were done by single operator and blinding was considered to overcome experimental bias. The surface area of each specimen was calculated using AutoCAD software [18]. After measuring the surface area, die preparation [4,19] die spacer application (Han Dae Chemical, Korea), Die spacer was applied in 2 layers to obtain approximately 25 μ thickness with 0.5 mm short of the margin. Wax patterns were fabricated using inlay casting wax by dipping the die twice in molten blue inlay wax in a prewarmed wax-pot, to achieve a standardised thickness of 1 mm. Wax patterns were immediately invested after remargination to minimise distortion [19]. Conventional lost wax technique was carried out to completely eliminate wax from the moulds, casting procedures using cobalt chromium alloys were carried out in an induction casting machine to fabricate metal copings. A total of 50 castings of same dimensions were recovered from the investment and finished and polished to standardised thickness of 1 mm [19]. Surface treatment and cementations were performed as follows [4]:
Group A (Control group): Sandblasted for 15s at 0.3 Mpa pressure with 50 μm particles of aluminum oxide + cemented with GIC (control group-10). Several studies have proved GIC to be gold standard and in clinical use since many years. It’s widely used in clinical practice and proved to provide good retention for long time hence it is used as control [15,17,18].
Group B1: Cemented with RMGI, without surface treatment (sample-10)
Group B2: Intaglio surface of casting was sandblasted for 15 seconds at 0.3 Mpa pressure with 50 μm particles of aluminum oxide (Renfert, Germay), cleaned in an ultrasonic unit for a minute, rinsed with water spray and dried with oil free air, and then a single layer of metal primer (Monobond N, Ivoclair Vivadent Lot no: R71491) was coated with micro brush. Allowed material to react for 60 seconds and excess dispersed with stream of air+cemented with resin modified GIC. (Sample-10)
Group C1: Cemented with resin cement, without surface treatment. (Sample-10)
Group C2: Intaglio surface of casting was surface treated as in group B2 + cemented with resin cement. (Sample -10) [Table/Fig-4].
Experimental groups prepared for each cement type and surface treatment.

After surface treatment, Cements were mixed according to manufacturer instructions and cemented onto teeth by single trained operator. GIC powder liquid was mixed in ratio of 3:1 by weight. Resin modified GIC and resin cements were supplied as two paste systems with auto dispensing device. With this device equal quantity of each paste by volume were dispensed and mixed. Thin film of luting cement was applied to intaglio surface of crown with a plastic instrument. The crowns were seated on corresponding tooth under constant load of 5 kg for 10 minutes along the long axis of the tooth with help of customised device to maintain weight of 5 kg for each specimen [4]. Excess cement was removed from all the samples and stored in 100% humidity at 37°C for 3 months in a storage media to simulate oral conditions and accomplish artificial ageing [12].
Method of Testing
A special holding device was fabricated for the purpose of holding the specimen in INSTRON universal testing machine [4,18]. The machine was switched on and tensile load of 500 kN at cross-speed of 0.5 mm/min was applied [18]. The breaking load was noted when the casting got separated from the tooth. The force at failure was noted in newton (N). The tensile force required to break the specimen was calculated in Megapascals (Mpa) according to the following equation [12].
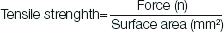
Each separated crown was subjected to stereomicroscopic analysis (LEICA stereomicroscope, LEICA Microsystems, Germany) to perceive the nature of bond failure. All the recordings were made by one observer. Three modes of failure were instituted, cohesive failure that is within cement, adhesive failure between metal and cement, and mixed failure combination of both. Metal cement interface fracture (adhesive failure, when more than 75% of cement remained attached on the axial wall of the tooth) was considered in the study. Specimens after debonding were observed under stereomicroscope for 3D view and evaluate type of failure [Table/Fig-5] [4].
INSTRON universal testing machine.

Statistical Analysis
SPSS 17.0 statistical software was used to analyse the data. The data obtained were subjected to statistical analysis using ANOVA test followed by Tukey’s Honest Significant Difference (HSD) post-hoc test. The mean average values were calculated for each group and the standard deviations were calculated. p<0.05 was considered significant for all the tests.
Results
The mean tensile bond strength of all the groups is shown in the [Table/Fig-6]. Among these, group C2 (resin cement with surface treatment) showed highest tensile bond strength (7.61±0.78 N/mm2), whereas group A (GIC control group) showed least tensile bond strength (3.78±0.65 N/mm2). The mean tensile bond strength between different groups of luting cements showed statistically significant difference (F=60.061, p<0.001)
The distribution of mean tensile bond strength of all five groups.
| Group | N | Mean±SD, N/mm2 | 95% confidence interval for mean | Range (Mpa) |
|---|
| Lower bound | Upper bound |
|---|
| A | 10 | 3.78±0.65 | 3.31 | 4.25 | 2.82-4.95 |
| B1 | 10 | 5.14±0.50 | 4.78 | 5.50 | 4.34-6.21 |
| B2 | 10 | 6.09±0.61 | 5.64 | 6.53 | 5.49-6.98 |
| C1 | 10 | 6.83±0.39 | 6.54 | 7.12 | 6.21-7.34 |
| C2 | 10 | 7.61±0.78 | 7.05 | 8.18 | 6.16-8.59 |
| Total | 50 | 5.68±1.49 | 5.25 | 6.10 | 2.82-8.59 |
Comparison of mean difference of tensile bond strength within different luting cements by applying Tukey’s HSD post-hoc test showed statistically significant results. Firstly, the mean difference of GIC (group A) was compared with the mean difference other test groups. Similarly, the mean tensile bond strength of RMGI (group B1) compared with group C1 and C2 showed highly significant (p<0.001*) whereas with B2, the difference was statistically significant (0.010*). Comparison between group B2 and C2 showed statistically significant (p<0.001*) result whereas with group C1, the difference was not statistically significant (p=0.064). In addition, comparison between group C1 and C2 showed statistically significant difference (p<0.047*); [Table/Fig-7].
Comparison of mean tensile bond strength within different groups of luting cements Tukey’s HSD post-hoc test (p<0.001).
| (I) Groups | (J) Groups | Mean difference (I-J) | p-value |
|---|
| A | B1 | −1.36400* | <0.001* |
| B2 | −2.30500* | <0.001* |
| C1 | −3.05000* | <0.001* |
| C2 | −3.83100* | <0.001* |
| B1 | B2 | −0.94100* | 0.010* |
| C1 | −1.68600* | <0.001* |
| C2 | −2.46700* | <0.001* |
| B2 | C1 | −0.74500 | 0.064 |
| C2 | −1.52600* | <0.001* |
| C1 | C2 | −0.78100* | 0.047* |
*Significant; SD: Standard deviation
Two subsets of groups with statistically similar means were created by Tukey’s test. The first and second subsets contained means of group A and group B1 (indicated no other groups have similar means), whereas the third subset contained group B2 and group C1 had one mean per group (indicated that these groups have similar means). The fourth subset contained means of group C2 (indicated no other groups have similar means). Only two groups group B2 and group C1 had similar means and was found to be statistically insignificant.
Mean tensile bond strength of Glass ionomer cement control group (3.78±0.65) was significantly lower than mean tensile bond strength of other test groups. Resin cement with surface treatment showed highest retentive strength among all tested groups while glass ionomer cement showed lowest tensile bond strength.
Null hypothesis that Surface treatment of intaglio surface does not have any effect on retention of complete cast crowns was rejected as the surface treatment significantly improved bond strength improving retention [Table/Fig-6,7].
Discussion
The purpose of the study was to assess and evaluate the retention of complete cast crowns, which were subjected to surface treatments involving sandblasting with alumina particles and metal primer and these restorations were cemented with GIC, RMGI, and resin cement. Objectives of this study were to comparatively evaluate surface treatments and cements and their effect on retention of complete cast crowns.
This study showed that the mean retentive strength of resin cement and RMGI increased after surface treatment with sandblasting and metal primer. With significant statistical difference, the resin cement indicated greater tensile strength values, followed by RMGI and GICs. Similarly, a study conducted by Consani S et al., also showed that the resin cement was superior when compared with glass ionomer and RMGI [20].
Metal primers contain active monomers that promote chemical bonding between the cement and the oxides present on the metal surface. Metal primers provide chemical as well as mechanical retention. Mechanical retention achieved by etching of metal surface by acids in metal primer. Metal primers having a phosphoric acid monomer (MDP, 10-methacryloyloxydecyl dihydrogen phosphate) react with readily formed oxides of base metal and improve the bonding of resin to the metal. Use of these metal primers require adequate isolation, avoid contact with skin and mucus membrane [4].
GIC is considered as control as most of the studies have proved it to be gold standard and is in clinical use since many years. It’s widely used in clinical practice and proved to provide good retention for long time. Surface treatment with metal primer considered only for test groups i.e., resin modified GIC and resin cement. Metal primer does not react with GIC, hence only surface treatment with alumina particles was done for control group.
With regard to bond performance, resin cement showed higher bond strength than RMGI. Capa N et al., also studied the bonding performance of RMGI cement and self-adhesive resin cement to various fixed prosthodontic core materials and found the highest bond strength for RelyXUnicem (resin cement) and the lowest for FujiCem (GIC) which is in agreement with current study [21].
Matsumura H et al., evaluated that bonding of a cobalt-chromium alloy with acidic primers and found that all acidic primers used in the study elevated bond strength of resin to cobalt chromium alloys, which is in agreement with the present study, where surface treatment with metal primer increased bond strength of resin-based cements [22]. A study conducted by Di Francescantonio M et al., also studied the effectiveness of application of adhesive primers to cobalt-chromium and nickel-chromium metal alloys on the bond strength of resin cements to alloys [6]. They concluded that the application of metal primer led to a higher bond strength for LinkMax resin cement when used in both the metal alloys, which was in agreement with the current study. However, similar results were not found with other cementing systems used in their study. Also, a study conducted by Yoshida K et al., evaluated the bond strengths of four resin cements to cobalt-chromium alloy using two adhesive primers [23]. They also evaluated the effect of four adhesive primers on bond strength of a self-curing resin to cobalt-chromium alloy [24]. All the primed specimens showed improved shear bond strength between resin cement and cobalt-chromium alloy when compared to nonprimed specimens. The results obtained were concurrent to current study that metal primers improved retentive strength of cobalt chromium crowns.
All the intaglio of castings were subjected to airborne abrasion from alumina to seize over the superficial oxide layer before application of metal primer. This also helped in mechanically cleaning the surface of investment, and increase the surface bonding area. This procedure had been used in study conducted by Di Francescantonio M et al., and Kunt GE et al., to prepare the surface for bonding [25,26]. Similarly, a study conducted by Freitas APd and Francisconi PAS, assessed the effect on shear bond strength and their mode of fracture after different intaglio surface treatments between a metallic alloy and resin cement [27]. They observed an improved retention with the alloy primer; however, there was less bond strength when compared to sandblasting. In the current study, metal primer enhanced bonding with sandblasted alloy surface. Fairly alike, two studies conducted by Yoshida K et al., also assessed the effect of adhesive primers for noble metals and found results similar to current study [Table/Fig-8] [28,29]. Hence, metal primers can be regarded as an efficient method of improving retention for base and noble metal alloys and for cementation of fixed dental prosthesis. Sarafianou A et al., studied the effect on the bond strength between base metal alloy and indirect composite resin by using adhesive primers. they concluded that the airborne particle abrading nickel chromium castings with 50-μm alumina particles and proper adhesive primer can achieve a clinically satisfactory metal-resin bond strength [30]. thus, metal primer is useful in improving resin metal bonding.
Tabulation and comparison of other studies with the current study [6,20-23,25,27,29].
| Reference | Aim of study | Material type | Cements used | Surface treatment | Results |
|---|
| Consani S et al., [20] | Effect of different cements on tensile strength of metallic crowns subjected to thermocycling | Nickel chromium | SS White zinc phosphate, Vitremer RMGIC, Rely X resin cement | - | Resin cement >zinc phosphate and resin modified GIC which is in agreement with current study where resin cement showed higher bond strength than RMGIC |
| Capa N et al., [21] | Comparison of Shear bond strength of luting cements to different restorative core materials | Au-Pd-Ag, Co-Cr,Ni-Cr-Mo, Ni-Cr-Fe Titanium, Zirconia and Empress | RelyX Unicem and FujiCem. | - | Resin cement was found to have higher Bond strength with different metal alloys and Zirconia than that of RMGIC. This is in agreement with current study |
| Matsumura H et al., [22] | Effect of acidic primers on the bonding of luting agents to cobalt chromium alloy. | Co-Cr alloy | Super-Bond Opaque | Acryl Bond,Cesead opaque primer,Metal primer,MR bondSuper Bond liquid | All five primers enhanced bonding of resin to co-cr alloy which is similar to results of current study |
| DI Francescantonio M et al., [6] | Effect of adhesive primers on the bond strength of resin cements to alloys. | Cobalt-Chromium and Nickel-Chromium | Bistite II DC, LinkMax, Panavia F 2.0, RelyX Unicem | Metaltite, Metal Primer II, Alloy Primer, Ceramic Primer | The study concluded that adhesive primers did not increase the bond strength between alloy surfaces and resin cements. |
| Yoshida K et al., [23] | Effect of adhesive primers on Shear bond strengths of resin cements to alloys. | Cobalt-Chromium (Co-Cr) alloy | Imperva Dual, Panavia 21, Super-Bond C&B and Bistite Resin Cement | Metal Primer and Cesead Opaque Primer | The Cesead Opaque Primer has resulted to enhance the shear bond strengths of resin cements to alloy as compared with non-primed and Metal Primer. Results of this study are similar to the current study |
| Di Francescantonio M et al., [25] | Studied the effect of adhesive primer on the bond strength of resin cements to cast titanium. | Titanium | Bistite II DC, Link Max, Panavia F 2.0, RelyX Unicem and RelyX ARC | Metaltite, Metal Primer II, Alloy Primer and Ceramic Primer | Adhesive primers were proofed to enhance bond strength of cast titanium to resin cement. These findings are similar to the findings of current study |
| Freitas APd and Francisconi PAS, [27] | Metal Primer Effect on the Bond Strength of Metal and Resin Interface | Co-Cr-Mo - Remanium CD | Rely X TM | Sandblasting andAlloy Primer (Kuraray); | Alloy Primer increased the retention between the cement and the polished surface of alloy. |
| Yoshida K et al., [29] | Effect of adhesive primers on bond strengths of resin cement to noble metal | Silver-Palladium-Copper-Gold | BistiteII (BRII), Panavia Fluoro Cement (PFC) and Super-Bond C&B (SB) | Alloy Primer (AP), Metal PrimerII (MPII) and Metaltite (MT | Bond strength seemed to improve in primed specimens in comparison to nonprimed specimens |
| Current study | Effect of surface treatment on retention of cast crowns luted with different cements | Cobalt Chromium | GIC GC Gold Label, RMGI GC FugiCEM, resin cement RelyxTM U200 | Sandblasting andMetal primer (monobond N) | Combination of sandblasting and metal primer enhanced bond strength of cast crowns to resin based cements |
Limitation(s)
Although the test methods used in current study attempted to simulate the clinical conditions there were some limitations. In the current in-vitro study fixed taper and height for crown preparations were used, however this is not the case in clinical situations, this may show a different clinical outcome. The bonding of the cement to the extracted teeth may not be similar to bonding with natural vital tooth which may have affected the result. The unilateral static loading force applied to specimen cannot replicate the complex dynamic forces present in the oral cavity during mastication and parafunctional habits.
Conclusion(s)
Within the limitations of the current study, sandblasting plus metal primer application can be an effective method of increasing bond strength of crowns to resin-based cements. Since, application of metal primer is simple and effective method of increasing retentive strength, this could be an alternative to various other complicated surface treatments. Further investigation are needed to assess factors like, taper of preparation, different metal alloys being cemented, effect of the auxiliary retentive features, effect of various other surface treatments, different luting agents, and their film thickness. To authenticate the findings of the study, the surface treatment of intaglio of crown may be applied clinically. Such study would validate clinical outcome of surface treatment for resin-based cements on retention.
*Significant; SD: Standard deviation