Incidentally Detected Intranasal Supernumerary Tooth: A Case Report
S Aparna1, Rishikant Sinha2, Upasna Sinha3, Prem Kumar4
1 Academic Junior Resident, Department of Radiodiagnosis, AIIMS, Patna, Bihar, India.
2 Senior Resident, Department of Radiodiagnosis, AIIMS, Patna, Bihar, India.
3 Assistant Professor, Department of Radiodiagnosis, AIIMS, Patna, Bihar, India.
4 Professor and Head, Department of Radiodiagnosis, AIIMS, Patna, Bihar, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. S Aparna, Hostel 5, AIIMS, Patna, Phulwari Sharif, Patna-801507, Bihar, India.
E-mail: aparnas659@gmail.com
Intranasal tooth is a rare type of supernumerary teeth. Its aetiopathogenesis is uncertain but genetic predisposition, trauma and infection are described in previous literatures. It can be either symptomatic or asymptomatic. In our case report, it was asymptomatic which was diagnosed mainly by CT scan as a radiopaque lesion with morphology and attenuation same as that of intraoral tooth. We report a case of an incidental intranasal supernumerary tooth in a 45-year-old male who presented with history of road traffic accident and parasymphyseal fracture of left mandible. This case highlights the rarity of this entity.
Ectopic tooth, Mesiodens, Nasal tooth
Case Report
A 45-year-old male presented to the emergency department with history of road traffic accident and chief complaint of pain in jaw and difficulty in opening mouth. His systemic examination and blood investigations were within normal limits. The Non-Contrast Computerized Tomography (NCCT) head and face showed normal brain parenchyma with no evidence of intra axial or extra axial bleed. No fractures of calvarial bones were seen. A linear non-displaced fracture was seen involving the left parasymphyseal region extending upto alveolar cortex. Incidentally, a hyperdense area with attenuation and morphology similar to that of tooth was noted in left nasal cavity below the inferior turbinate [Table/Fig-1,2]. The radiological differentials were rhinolith and calcified fungal mass. These were excluded on the basis of characteristic features. The patient was given conservative management with antibiotic prophylaxis and referred to dental department where conservative management and treatment for fracture was continued. The patient was counselled for follow-up owing to higher chances for complications such as sinusitis.
CT scan Axial View shows a hyperdense area of tooth attenuation and morphology with central radiolucency in left nasal cavity below left inferior turbinate, oriented obliquely. (yellow arrow)

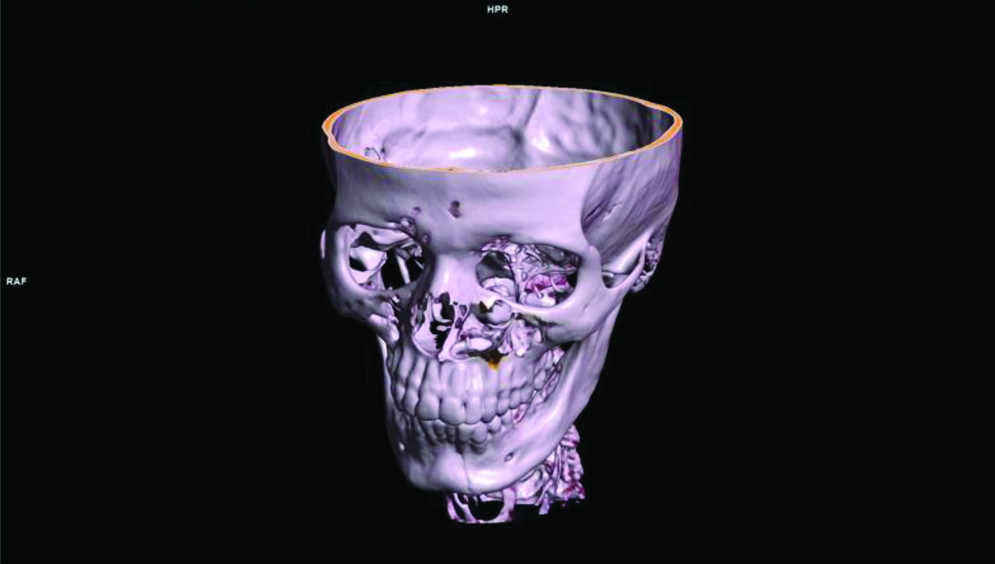
Volume rendered image shows an obliquely oriented tooth in left nasal cavity. Left parasymphyseal fracture also seen.
Discussion
Supernumerary teeth are those that are additional to the normal dentition (with an incidence of 0.1-1% of general population) with uncertain aetiopathogenesis, and are most commonly located in the anterior region of the maxilla where they are known as Mesiodens, [1] growing either palatally or rarely as ectopic tooth at sites of mandibular condyle, coronoid process, orbit, nasal cavity including the nasal septum [2] with intra nasal teeth rarest among these [3] often considered as an inverted mesiodens. Several associations such as Gardner’s Syndrome, Cleidocranial Dysostosis, Cleft Palate have been described with it [4].
Being a rare form of supernumerary teeth it may be symptomatic or remain asymptomatic as in our case. Symptoms of intranasal tooth may vary from nasal obstruction, epistaxis, foul smelling rhinorrhea, headache, facial pain, sinusitis [5] to external nasal deformity, nasal localised ulceration, rhinitis caseosa with nasal septal perforation and aspergillosis and naso-oral fistula [6].
The diagnosis of nasal teeth is based on clinical and radiographic findings.
Clinical examination and nasal speculum examination followed by radiographic evaluation with waters view, lateral skull or orthopantamogram is sufficient for initial diagnosis in case of symptomatic patients. Incidentally detected cases from CT such as ours have the advantage that since CT confirms diagnosis and will also show the depth of root at the eruption site it assists in surgical planning for removal and it also helps in differentiating it from luxative injury in dental trauma to permanent dentition causing ectopic location of tooth [7]. CT represents certain findings which include lesions that are radiopaque and has same attenuation as of teeth. With the application of Bone window setting and depending on the orientation of the teeth, the central radiolucency is correlated with the pulp cavity having a spot or slit as seen in our patient. There may also be soft tissue surrounding radiopaque lesion consistent with granulation tissue [6]. The nasal supernumerary teeth usually have a specific morphology, in which the most common form is the cone shape [8]. The less frequent are the molar shape and barrel shaped types. In our case cone shaped tooth like hyperdense area within the left nasal cavity below left inferior turbinate, with left parasymphyseal fracture of mandible was seen but there was no injury to any of the maxillary alveolar sockets thus differentiating it from a luxative injury associated with ectopic location.
Radiopaque foreign body; rhinolith; inflammatory lesions in tuberculosis, or calcifications within fungal infection; osteoma, calcified polyps, enchondroma, dermoid are some of the common differentials of nasal tooth [4-6]. The possible differentials in our case were that of ectopic location following dental trauma but absence of any comminuted fracture to any of the alveolar socket ruled out the same and others were fungal mass, bony sequek,strum and exostosis.
The treatment involves removal of nasal teeth endoscopically or otherwise via intra nasal or intra oral approach [9]. Asymptomatic nasal tooth may be followed-up radiographically with orthopantamogram, water’s view or CT scan.
Conclusion
Intranasal supernumerary tooth is a rare form of ectopic tooth which in the present case was asymptomatic and detected incidentally in radiological imaging by its characteristic appearance of attenuation similar to that of intraoral tooth. CT imaging helps in diagnosing and preoperative evaluation by assessing the depth of eruption site and orientation of tooth at the ectopic site as well as in follow-up.
Author Declaration:
Financial or Other Competing Interests: No
Was informed consent obtained from the subjects involved in the study? Yes
For any images presented appropriate consent has been obtained from the subjects. Yes
Plagiarism Checking Methods: [Jain H et al.]
Plagiarism X-checker: Aug 12, 2019
Manual Googling: Nov 05, 2019
iThenticate Software: Nov 23, 2019 (14%)
[1]. Noleto JW, Prado R, Rocha JF, DaCosta MF, Barbosa CG, Toscano MG, Intranasal inverted tooth: A rare cause of a persistent rhinosinusitisIndian J Dent Res 2013 24:762-64.10.4103/0970-9290.12763024552943 [Google Scholar] [CrossRef] [PubMed]
[2]. Mohebbi S, Salehi O, Ebrahimpoor S, Ectopic supernumerary tooth in nasal septum: a case studyIran J Otorhinolaryngol 2013 25(72):183-86. [Google Scholar]
[3]. Choudhury B, Das AK, Supernumerary Tooth in the Nasal CavityMed J Armed Forces India 2008 64(2):173-74.10.1016/S0377-1237(08)80071-8 [Google Scholar] [CrossRef]
[4]. Nazif MM, Ruffalo RC, Zullo T, Impacted supernumerary teeth: A survey of 50 casesJ Am Dent Assoc 1983 106:201410.14219/jada.archive.1983.03906572675 [Google Scholar] [CrossRef] [PubMed]
[5]. Chen A, Huang JK, Cheng SJ, Sheu CY, Nasal teeth: report of three casesAJNR 2002 23(4):671-73. [Google Scholar]
[6]. Smith RA, Gordon NC, De Luchi SF, Intranasal teeth: report of two cases and review of the literatureOral Surg Oral Med Oral Pathol 1979 47:120-22.10.1016/0030-4220(79)90163-4 [Google Scholar] [CrossRef]
[7]. Kumar RA, Kumar PS, Maxillary permanent tooth in the nasal cavity: Report of two cases with different etiopathogenesis, management and review of the literatureThe Internet Journal of Dental Sciences 2009 9(1):01-06.10.5580/104e [Google Scholar] [CrossRef]
[8]. Kim DH, Kim JM, Chae SW, Hwang SJ, Lee SH, Lee HM, Endoscopic removal of an intranasal ectopic toothInt J Pediatr Otorhinolaryngol 2003 67:79-81.10.1016/S0165-5876(02)00290-2 [Google Scholar] [CrossRef]
[9]. Lin IH, Hwang CF, Su CY, Kao YF, Peng JP, Intranasal tooth: report of three casesChang Gung Med J 2004 27(5):385-89. [Google Scholar]