Acute Vaginitis: A Rare Cause of Labial Adhesions
Ankita Mann1, Sumita Mehta2, Anshul Grover3
1 Senior Resident, Department of Obstetrics and Gynaecology, Babu Jagjivan Ram Memorial Hospital, Delhi, India.
2 Specialist and Head, Department of Obstetrics and Gynaecology, Babu Jagjivan Ram Memorial Hospital, Delhi, India.
3 Specialist, Department of Obstetrics and Gynaecology, Babu Jagjivan Ram Memorial Hospital, Delhi, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Ankita Mann, F-49, Prashant Vihar, New Delhi, India.
E-mail: ankitamann1988@gmail.com
Labial adhesions occur most often in infants and young girls and are associated with low oestrogen levels. Herein, we report a case of labial adhesion in a 24-year-old young girl, who presented with acute retention of urine. Clinical examination revealed normally developed external genitalia and a thin membrane occluding the introital opening. Her secondary sexual characters were normal; the most probable cause being acute vaginitis, her hormonal profile was not done. Patient was managed with sharp excision of membrane followed by local application of antibiotics. Patient was asymptomatic at three months follow-up with completely healed labia.
Hence, all women including unmarried ones who present with urinary complaint need to have a complete gynaecological examination as the two can be related.
Labial fusion, Recurrent urinary tract infections, Vulval dystrophy
Case Report
A 24-year-old unmarried girl attended gynae OPD of the hospital, with complaints of acute retention of urine and lower abdominal pain for past 8 hours. She had a history of voiding difficulty with recurrent urinary tract infection for past 6 months, for which she had taken medication from a local practitioner and got symptomatically relieved. She had a course of Norfloxacin for 7 days followed by another course of Nitrofurantoin for one week in the past. No examination or any investigation was done in the past. She had no history of surgical intervention and her medical history was insignificant. There was no history of trauma or sexual assault. She attained menarche at 13 years and her menstrual cycles were regular.
On examination, she had normal secondary sexual characters. Examination of genital area showed introital opening occluded with a thin membrane which had a small pinhole opening about 2 cm below the clitoris [Table/Fig-1]. This was the common opening for both urine and menstrual blood. Pelvic ultrasound and laboratory work-up were normal. Dermatological examination was unremarkable. Micturating Cystourethrography (MCU) affirmed normal urinary system.
Occluded vaginal introitus.
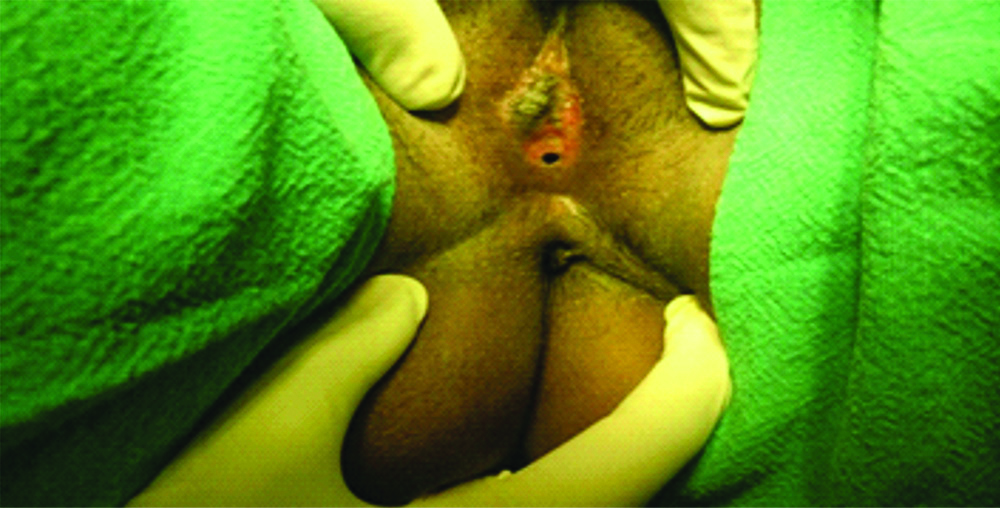
She was examined under general anaesthesia and inspection of external genitalia revealed no urethral or vaginal opening but a thin membrane occluding the introitus with a small pin-hole opening presents about 2 cm below the clitoris.
In consultation with general surgeon, the pin hole opening in the membrane was used as a guide to sharply dissect the membrane under guidance, in both upward and downward direction. Both the urethral orifice and the vaginal introitus were seen in normal anatomical positions behind the excised membrane. The released edges were sutured. Vaginal mucosa was congested and inflamed and a vaginal swab was taken for culture. Intra-operative visualisation confirmed that cervix and vagina were also anatomically normal as shown in [Table/Fig-2].
Normal vagina and urethral opening.
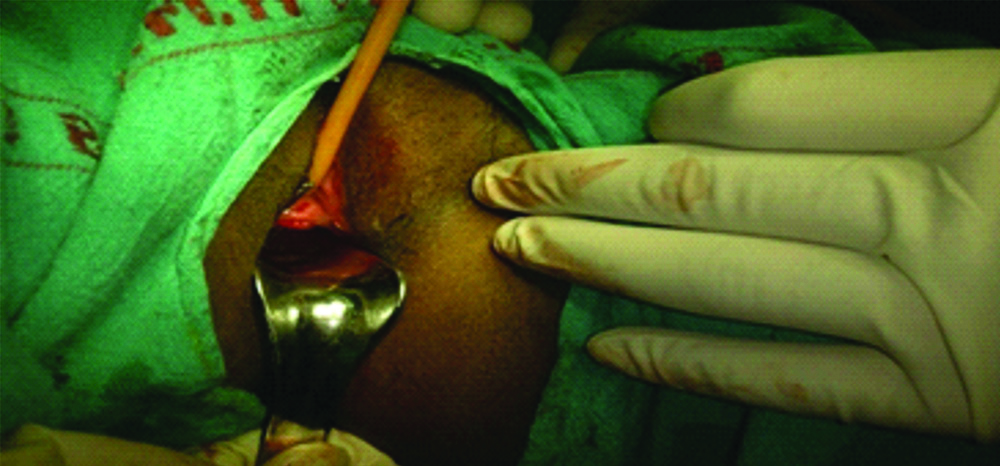
Patient was discharged in satisfactory condition with advice for daily local application of antibiotic (Mupirocin) ointment. On follow-up at the end of 2 weeks, labial tissue was found completely healed and her voiding problems had resolved.
Discussion
Labial Fusion (LF) is defined as partial or complete adhesion of labia majora or minora and is estimated to occur in 0.6-5% of pre-pubertal girls [1]. It may also be known as synechia vulvae or labial agglutination. The exact cause for labial adhesions remains uncertain. However, it is believed that hypo-estrogenism may be a contributing cause. In post-menopausal women, due to low oestrogen, genital area is more suspectible to irritation and inflammation, which may lead to adhesion.
On reviewing the literature, numerous case reports [2,3] in young girls with hypoestrogenic state leading to labial adhesions were found, but no case report discussing labial adhesions following vaginal infection was found.
Labial fusion is extremely rare in reproductive age group like the index patient, due to sufficient levels of oestrogen found in this population. It is usually associated with local inflammatory and irritative conditions and vulval dystrophies. These processes cause denudation of labial epithelium and the contra-lateral labial edges then heal together by fibrosis. The condition has varied symptomatically; although majority of reported cases are asymptomatic, rarely they may present with post-void dribbling (urinary incontinence), urinary tract infections, vaginitis, haematuria and urinary frequency [4]. Labial fusion can be present secondary to vaginal laceration after child birth, female circumcision, herpes simplex or dermatological conditions. In chronic or untreated cases, chronic inflammation leads to fibrosis and scarring despite of normal oestrogen levels [5].
In the present case, inflammation and irritation secondary to vaginitis may have caused superficial epithelium of labia to heal with fibrous adhesions thereby occluding the introitus. Recurrent urinary tract infection may have been the result of her passing urine and menstruating through the same opening. Vaginal swab was sterile due to multiple courses of antibiotics she had taken in the past.
Labial adhesion is a clinical diagnosis and treatment depends on symptoms. Some studies have reported upto 80% of labial adhesion resolution without any treatment [6-8]. While favourable results are usually obtained with topical oestrogen application and good hygiene practices for labial adhesions in children, oestrogen therapy is not always successful as a first-line treatment in adults [9,10]. Mostly surgery may be necessary in them as was with our patient who was managed with surgical adhesionolysis. Recurrences are common in labial adhesions and can be managed with topical treatment or with surgical lysis of the fusion.
Conclusion
In young women, labial adhesions can occur after untreated severe vaginitis irrespective of normal oestrogen levels. Such women can present with menstrual problems or voiding difficulties. Therefore, gynecological examination is necessary for evaluation of voiding symptoms. The index patient presented with urinary retention and history of recurrent urinary tract infection probably due to labial adhesions. Labial adhesions would have been missed if a complete examination including gynaecological examination had been omitted.
Author Declaration:
Financial or Other Competing Interests: No
Was informed consent obtained from the subjects involved in the study? Yes
For any images presented appropriate consent has been obtained from the subjects. Yes
Plagiarism Checking Methods: [Jain H et al.]
Plagiarism X-checker: Jun 18, 2019
Manual Googling: Aug 08, 2019
iThenticate Software: Oct 09, 2019 (16%)
[1]. Mayaoglu L, Dulabon L, Martin-Alguacil N, Pfaff D, Schober J, Success of treatment modalities for labial fusion: a retrospective evaluation of topical and surgical treatmentsPediatr Adolesc Gynecol 2009 22(4):247253(247-250)10.1016/j.jpag.2008.09.00319646671 [Google Scholar] [CrossRef] [PubMed]
[2]. Vilano SE, Robbins CL, Common prepubertal vulvar conditionsCurr Opin Obstet Gynecol 2016 28(5):359-65.10.1097/GCO.000000000000030927517340 [Google Scholar] [CrossRef] [PubMed]
[3]. Bussen S, Eckert A, Schmidt U, Sutterlin M, Comparison of conservative and surgical therapy concepts for synechia of the labia in pre-pubertal girlsGeburtshilfe Frauenheilkd 2016 76(4):390-95.10.1055/s-0035-155810127134294 [Google Scholar] [CrossRef] [PubMed]
[4]. Ustuner I, Avsar AF, Labial adhesion with acute urinary retention secondary to bartholin’s abscessLUTS: Lower Urinary Tract Symptoms 2012 4(2):106-08.10.1111/j.1757-5672.2012.00142.x26676535 [Google Scholar] [CrossRef] [PubMed]
[5]. Awang NA, Viegas C, Viegas OA, Incomplete bladder emptying due to labial fusion in a pubertal girl: a delayed consequence of female circumcisionAust NZ J Oster Gynecol 2004 44:372-73.10.1111/j.1479-828X.2004.00261.x15282020 [Google Scholar] [CrossRef] [PubMed]
[6]. Norris JE, Elder CV, Dunford AM, Rampal D, Cheung C, Grover SR, Spontaneous resolution of labial adhesions in pre-pubertal girlsJ Paediatr Child Health 2018 54(7):748-53.10.1111/jpc.1384729436045 [Google Scholar] [CrossRef] [PubMed]
[7]. Rubinstein A, Rahman G, Risso P, Ocampo D, Labial adhesions: Experience in a children’s hospitalArch Argent Pediatr 2018 116(1):65-68.10.5546/aap.2018.eng.65 [Google Scholar] [CrossRef]
[8]. Fernandez S, A Pediatrician’s take on a few common infant urologic and gynaecologic issuesPediatr Ann 2017 46(11):e397-99.10.3928/19382359-20171018-0329131917 [Google Scholar] [CrossRef] [PubMed]
[9]. Seehusen DA, Earwood JS, Postpartum labial adhesionsJ Am Board Fam Med 2007 20:408-10.10.3122/jabfm.2007.04.06021417615422 [Google Scholar] [CrossRef] [PubMed]
[10]. Acharya N, Mandal AK, Ranjan P, Kamat R, Kumar S, Singh SK, Labial fusion causing pseudo-incontinence in an elderly womanInt J Gynecol Obstet 2007 99:246-47.10.1016/j.ijgo.2007.05.03217669409 [Google Scholar] [CrossRef] [PubMed]