Letter to the Editor on ‘PCR as a Diagnostic Tool for Extra-Pulmonary Tuberculosis’
Takahiko Nagamine1
1 Department of Emergency Medicine, Sunlight Brain Research Center, Hofu, Yamaguchi, Japan.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Takahiko Nagamine, 4-13-18 Jiyugaoka, Hofu, Yamaguchi, Japan.
E-mail: tnagamine@outlook.com
Dear Editor,
Extra-Pulmonary Tuberculosis (EPTB) is a significant cause of morbidity. Diagnosis of this condition requires high clinical suspicion. Accurate diagnosis of EPTB depends on the detection of mycobacteria, but these methods have low sensitivity. I read with great interest the article entitled “PCR as a Diagnostic Tool for Extra-Pulmonary Tuberculosis” by Ajantha GS et al., [1]. They indicated that Polymerase Chain Reaction for TB (PCR-TB) is certainly a very useful tool in the diagnosis of EPTB. I agree with the proper utilisation of PCR-TB. It may give vital evidence compared to the established conventional methods. Recently, I experienced a patient who was diagnosed as having miliary TB and spinal caries, by performing repeated PCR-TB for the lung specimen.
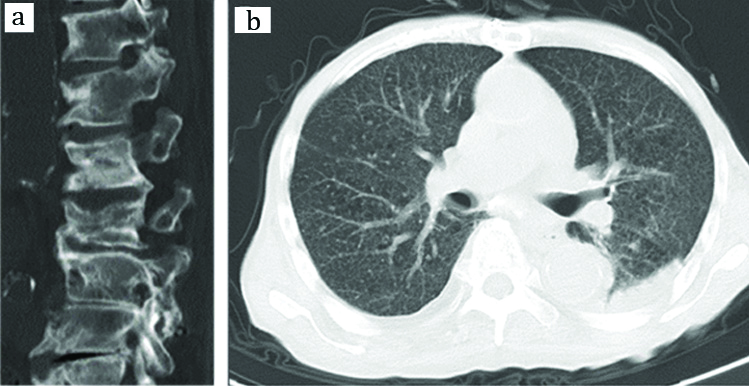
An 89-year-old man was transferred to the emergency department because of fever and low back pain. He was not immuno-compromised, and never had immuno-suppressive agents. Although several antibiotics such as cefmetazole, sulbactam/ampicillin, and meropenem had been prescribed, periodic high fever continued. He did not show any respiratory symptoms such as cough and dyspnea. Lumbar Computed Tomography (CT) revealed the distraction of vertebras and chest CT showed miliary nodules that were generally uniform in size and widespread in distribution, indicative of EPTB such as spinal caries and miliary TB [Table/Fig-1]. We immediately performed PCR-TB for his lung specimen several times. A positive result was finally obtained after performing it five times, while acid fast bacteria stain was all negative. Then, he was diagnosed as having EPTB, and successfully treated with antitubercular agents.
Spinal CT: a) Indicating the distraction of vertebra and chest CT; b) Showing miliary pattern.
Miliary TB is the result of diffuse dissemination of M. tuberculosis bacilli via blood stream, causing numerous foci in multiple organs [2]. Non-specific clinical features and late appearance of chest radiographic changes make the diagnosis difficult. Moreover, accurate diagnosis of spinal TB is difficult because of the necessity of invasive procedures. Spinal TB accounts for around 2% of all cases of TB and around 15% of EPTB [3]. Rapid diagnostic tests reduce diagnostic delays and should be performed on patients with radiological features of TB. EPTB patients may show negative smear results for acid-fast bacilli, no granulomas on histopathology and even negative culture for M. tuberculosis. The interferon-γ- release assays are also useful to detect TB, but they cannot discriminate between latent infection and active disease [4].
Nucleic acid amplification may help in diagnosis of EPTB. PCR techniques can be based on conventional DNA amplification. It is a suitable method for fast detection of M. tuberculosis complex DNA. However, PCR-TB has several limitations. First, the effectiveness of PCR in diagnosing TB is related to demanding factors including DNA concentration in the clinical sample. Second, PCR has often been criticised for amplifying dead bacilli. Third, as for the most important thing, the sensitivity of PCR is not so high that repeated measurement was warranted to increase diagnostic sensitivity. Developing a new technology to diagnose EPTB is needed because diagnosis of this condition still remains high clinical suspicion.
Sincerely.
Author Declaration:
Financial or Other Competing Interests: No
Was informed consent obtained from the subjects involved in the study? NA
For any images presented appropriate consent has been obtained from the subjects. Yes
PLAGIARISM CHECKING METHODS: [Jain H et al.]
Plagiarism X-checker: Sep 03, 2019
Manual Googling: Sep 24, 2019
iThenticate Software: Sep 27, 2019 (9%)
[1]. Ajantha GS, Shetty PC, Kulkarni RD, Biradar U, PCR as a diagnostic tool for extra-pulmonary tuberculosisJ Clin Diagn Res 2013 7(6):1012-15.10.7860/JCDR/2013/5425.307523905092 [Google Scholar] [CrossRef] [PubMed]
[2]. Sharma SK, Mohan A, Miliary tuberculosisMicrobiol Spectr 2017 5(2)10.1128/microbiolspec [Google Scholar] [CrossRef]
[3]. Chen CH, Chen YM, Lee CW, Chang YJ, Cheng CY, Hung JK, Early diagnosis of spinal tuberculosisJ Formos Med Assoc 2016 115(10):825-36.10.1016/j.jfma.2016.07.00127522334 [Google Scholar] [CrossRef] [PubMed]
[4]. Purohit M, Mustafa T, Laboratory diagnosis of Extra-pulmonary Tuberculosis (EPTB) in resource-constrained setting: State of the art, challenges and the needJ Clin Diagn Res 2015 9(4):EE01-EE06.10.7860/JCDR/2015/12422.579226023563 [Google Scholar] [CrossRef] [PubMed]