Imaging of the eye has grown significantly over the last 20 years. Among various ophthalmic imaging techniques such as scanning laser polarimetry and confocal scanning laser ophthalmoscopy, OCT has emerged to the forefront of ocular imaging. It is a method of using low-coherence interferometry to determine the echo time delay and magnitude of backscattered light reflected-off an object of interest. In 1993 Fercher AF et al., [1] presented the first in vivo OCT images and in 1995, Schuman JS et al., [2] and Puliafito CA et al., [3] produced the first images of retinal disease. The archetype instrument for OCT is grounded on slit lamp biomicroscope that was revised to offer a view of the fundus for image orientation and also capable of simultaneous OCT imaging. Developments in OCT technology have been attained by examining ultra-high-resolution OCT, adaptive optics OCT, eye-tracking OCT, and changes in signal detection technique from Time-Domain (TD) to Spectral-Domain (SD) detection.
The Spectral-Domain OCT (SD-OCT) offers greatly improved image acquisition speed and image resolution up to 5 μM.
Triamcinolone acetonide is an effective and safe agent for intravitreal injection in conditions requiring long-term administration of ocular steroids. It decreases inflammation and scarring and is routinely used to treat eye inflammation. IVTA injection has been shown to be effective in refractory cystoid macular oedema with birdshot retinochoroidopathy [5], refractory diabetic macular oedema [6], macular oedema secondary to retinal vascular diseases [7], central retinal vein occlusion [8], branch retinal vein occlusion [9], proliferative diabetic retinopathy and proliferative vitreoretinopathy [10], and idiopathic retinal periphlebitis [11-12].
Glucocorticoids are known to decrease mediators of inflammation including Interleukin-5, Interleukin-8, prostaglandins, interferon gamma and tumour necrosis factor [13-15]. Triamcinolone Acetonide (TA) is a highly selective glucocorticoid without significant mineralocorticoid action. It is a more potent synthetic derivative of triamcinolone having low water solubility which contributes to its prolonged duration of action. The half life of 4 mg IVTA injection in non vitrectomized human eyes is 18.7±5.7 days and 3.2 days in vitrectomized eyes. The complete elimination of TA in non vitrectomized eye is not achieved until 93±28 days [16].
Triamcinolone has the capacity to modulate epithelial cell resistance, reduces permeability of the outer blood-retinal barrier, resorption of exudation and down-regulates inflammatory stimuli [17]. Corticosteroids have been shown to abolish the production of Vascular Endothelial Growth Factor (VEGF) by pro-inflammatory mediators like Platelet Derived Growth Factor (PDGF) and platelet activating factor [18]. They also inhibit expression of VEGF gene [19], reverses capillary permeability and stabilises blood vessels and the blood-retinal barrier [20-21], and also have an effect on cellular calcium levels [22-23], which may aid in the active diffusion of the fluid resulting in a decrease in the macular oedema.
In patients with uveitis, macular oedema and its sequelae are among the leading causes of decreased vision. Corticosteroids have been used in the treatment of macular oedema because of their ability to inhibit the arachidonic acid pathway, downregulate the production of vascular endothelial growth factor (VEGF), modulate the expression of Intercellular Adhesion Molecule-I (ICAM-1) and to reduce breakdown of the blood-retinal barrier (BRB).
Eales’ disease is an idiopathic retinal periphlebitis characterised by capillary non-perfusion, neovascularisation and recurrent vitreous haemorrhages, mainly involving the peripheral fundus. In Eales’ disease clinical manifestations are due to inflammation (peripheral retinal perivasculitis), ischemic changes (peripheral retinal capillary nonperfusion) and neovascularization of the disc and retina which frequently leads to vitreous haemorrhage.
Retinal vein occlusion is the second most common retinal vascular disease after diabetic retinopathy. Macular oedema is the commonest cause of visual impairment among those patients and developed due to vascular leakage and/or cytotoxic events. Corticosteroids, both intra- and extraocular, have long been used to treat oedema with Retinal Vein Occlusion (RVO), and the SCORE study results validated this therapy for oedema in CRVO.
Pseudophakic cystoid macular oedema is a common cause of decreased vision following complicated or uncomplicated cataract surgery. Vitreous loss preoperatively, placement of anterior chamber intraocular lens and prolonged postoperative inflammation are some of the risk factors associated with development of cystoid macular oedema following cataract surgery. It usually resolves spontaneously in majority of eyes and only a small subset of patients suffer permanent visual morbidity.
A number of studies have documented OCT changes after IVTA in posterior uveitis [24-25], retinal venous occlusive diseases [26-28], pseudophakic cystoid macular oedema [29-30] and idiopathic cystoid macular oedema [31].
There is a dearth of studies on OCT changes after IVTA in cases of choroiditis and Eales’ disease. Therefore this prospective interventional study was undertaken to study changes in posterior segment OCT and the impact of changes in posterior OCT on visual acuity after IVTA injection.
Materials and Methods
The present study was a hospital-based prospective interventional study conducted at the tertiary care centre in north India from April 2014 to December 2015. Institutional Ethical Clearance was obtained from institutional ethical committee and Tenets of the declaration of Helsinki were followed. A well informed written consent for repeated ocular examination, Fundus Fluorescein Angiography (FFA), OCT and IVTA injection was taken from all patients recruited in the study.
Inclusion criteria: Study group comprised of 30 patients (30 eyes) having inflammatory, proliferative or oedematous diseases of posterior segment who have not received any treatment for their condition in past and requiring IVTA injection.
Control group consisted of 30 patients (30 untreated healthy other eye of the patients enrolled in the study).
Exclusion criteria: Patients who have had previous ocular trauma, glaucoma, infective ocular disease, received laser photocoagulation, received systemic or local corticosteroids within past four weeks, eyes with significant corneal opacities, dense cataract, and significant vitreous haze or haemorrhage were excluded.
Even though IVTA injection can be safely given in well controlled diabetic patients but in present study none of the patient was diabetic.
A thorough ophthalmic examination (including LogMAR visual acuity, applanation tonometry, slit lamp biomicroscopy and fundus examination) was done at baseline and two weekly follow-up after IVTA injection upto 12-weeks follow-up.
Posterior segment OCT (Cirrus HD-OCT Model 5000, Carl Zeiss Meditec) and Fundus Fluorescein Angiography (FFA) was done at baseline, 6 weeks and 12 weeks follow-up. Macular thickness was documented in a modified Early Treatment of Diabetic Retinopathy Study (ETDRS) macular map. ETDRS macular map has central subfield of 1 mm diametre surrounded by parafoveal and perifoveal subfield having diameters of 3 mm and 6 mm respectively. These parafoveal and perifoveal subfields are divided into 4 quadrants (superior, inferior, nasal and temporal) by 4 radial lines. The retinal thickness in each of quadrants (of parafoveal and perifoveal subfields) and CFT were measured at baseline and at 6 and 12 weeks follow-up.
An unopened fresh 1 mL (40 mg) vial of preservative free TA (injection Aurocort 40 mg/mL by Aurolab pharmaceuticals) in suspension form was mixed by shaking and 4 mg in 0.1 mL was injected transconjunctivally through inferior pars plana with a 27G needle attached to a tuberculin syringe, 3.5 mm (pseudophakic eye) to 4 mm (phakic eye) posterior to the limbus. Indirect ophthalmoscopy was done after IVTA injection to confirm proper intravitreal localisation of the drug suspension and perfusion of the optic nerve head and presence of central retinal artery pulsations. The Intraocular Pressure (IOP) was measured using hand held tonometer and anterior chamber paracentesis was performed if IOP was greater than 25 mmHg. Immediately following IVTA injection patients were asked to sit up or allowed to lie in propped-up position so that the drug settles down inferiorly and not collect over macula.
Posterior segment OCT (Cirrus HD-OCT Model 5000, Carl Zeiss Meditec) was done at 6 and 12 weeks during follow up. FFA was done at baseline before IVTA injection and in the follow-up whenever possible during follow up.
Statistical Analysis
Statistical analysis was done using SPSS software version. Continuous variables were expressed as mean, standard deviation (SD) and range. Paired t-test was used to assess the statistical significance of differences in various variables at baseline and in the follow-up within the group. To study correlation between CFT and LogMAR viasual acuity, Pearson’s correlation test was applied and “r value” (correlation coefficient) was calculated. The difference was considered as statistically significant with p-value ≤0.05.
Results
The age of the patients ranged from 15 to 75 years with the mean age of 36.36±16.93 years. Out of 30 patients enrolled in the study (17 were males and 13 were females) 12 had posterior uveitis, 10 had retinal vascular occlusive diseases, 6 had Eales’ disease, whereas, pseudophakic cystoid macular oedema and idiopathic cystoid macular oedema was seen in one eye each.
The mean LogMAR visual acuity in the study group was 0.67±0.55 at baseline. After IVTA injection mean LogMAR visual acuity improved to 0.37±0.33 at 6 weeks (p<0.001) and 0.30±0.29 at 12 weeks (p<0.001) compared with the baseline [Table/Fig-1].
Mean LogMAR visual acuity on follow-ups after intravitreal triamcinolone acetonide injection.
| Time of examination | LogMAR visual acuity |
|---|
| Study group | Control group |
|---|
| (mean±SD) | p-value | (mean±SD) | p-value |
|---|
| Baseline | 0.67±0.55 | | 0.35±0.49 | |
| 6 weeks | 0.37±0.33 | <0.001* | 0.33±0.49 | 0.375 |
| 12 weeks | 0.30±0.29 | <0.001* | 0.30±0.49 | 0.233 |
The LogMAR visual acuity in posterior uveitis, retinal venous occlusive diseases, Eale’s diseases, pseudophakic CME and idiopathic CME during follow-up are depicted in [Table/Fig-2].
Mean LogMAR visual acuity on follow-up.
| Study group | Mean LogMAR visual acuity mean±SD |
|---|
| Baseline | 6 weeks | p-value | 12 weeks | p-value |
|---|
| Posterior uveitis | 0.52±0.56 | 0.29±0.33 | 0.036* | 0.22±0.20 | 0.072 |
| Retinal venous occlusive diseases | 0.86±0.60 | 0.37±0.25 | 0.007* | 0.35±0.30 | 0.007* |
| Eales’ disease | 0.61±0.45 | 0.36±0.38 | 0.040* | 0.38±0.42 | 0.179 |
| Pseudophakic cystoid macular oedema | 1.3 | 0.78 | | 0.60 | |
| Idiopathic cystoid macular oedema | 0.18 | 0.18 | | 0.00 | |
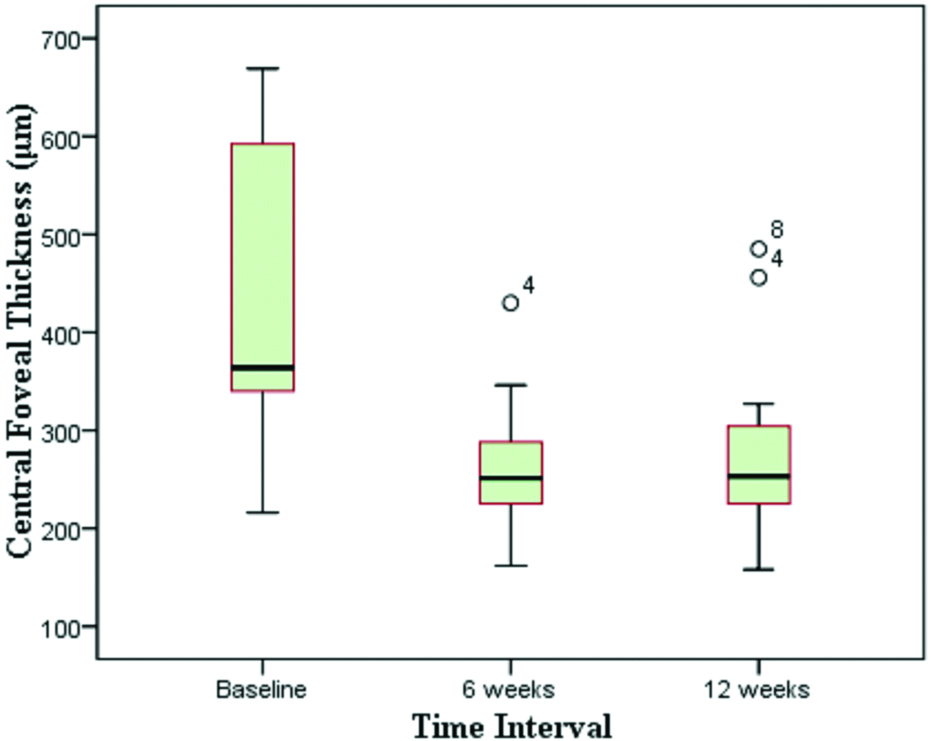
The mean baseline CFT in study group was 350.73±149.14 μM. After IVTA it decreased to 228.47±67.85 μM (p<0.001) and 250.27±82.09 μM (p<0.001) at 6 weeks and 12 weeks follow-up respectively [Table/Fig-3,4].
Effect of IVTA on central foveal thickness in study group.
Mean macular thickness on follow-up after IVTA injection.
| Macular thickness | Study group | Control group |
|---|
| Baseline (μM)±SD | 6 weeks (μM)±SD (p-value) | 12 weeks (μM)±SD (p-value) | Baseline (μM)±SD | 6 weeks (μM)±SD (p-value) | 12 weeks (μM)±SD (p-value) |
|---|
| Central foveal thickness |
| CFT | 350.733±149.14 | 228.47±67.85 (<0.001)* | 250.27±82.09 (<0.001)* | 256.75±55.96 | 255.00±50.44 (0.36) | 245.24±58.08 (0.13) |
| Inner macular thickness (parafoveal=3 mm) |
| Temporal | 367.83±117.48 | 287.43±67.12 (<0.001)* | 294.63±96.64 (0.01)* | 309.44±42.67 | 307.56±44.33 (0.32) | 300.64±57.51 (0.91) |
| Superior | 362.73±111.89 | 300.87±68.66 (0.002)* | 304.97±99.10 (0.01)* | 322.38±79.62 | 323.88±25.38 (0.93) | 312.40±44.71 (0.94) |
| Nasal | 369.87±97.47 | 288.30±60.36 (<0.001)* | 308.77±102.06 (<0.001)* | 327.75±25.88 | 325.19±25.35 (0.10) | 315.12±40.44 (0.13) |
| Inferior | 360.67±126.72 | 277.10±70.29 (<0.001)* | 297.57±102.35 (<0.001)* | 335.06±62.58 | 322.25±26.38 (0.23) | 310.12±47.30 (0.15) |
| Outer macular thickness (perifoveal=6 mm) |
| Temporal | 299.03±77.32 | 253.93±48.01 (<0.001)* | 257.60±63.61 (<0.001)* | 272.63±62.29 | 266.19±53.59 (0.17) | 261.71±34.61 (0.64) |
| Superior | 301.50±74.42 | 271.17±50.59 (0.023)* | 272.80±60.17 0.039)* | 273.94±49.82 | 279.38±25.15 (0.70) | 270.76±27.69 (0.54) |
| Nasal | 328.17±67.31 | 291.72±66.94 (<0.001)* | 286.62±75.97 (<0.001)* | 302.06±21.66 | 300.25±20.74 (0,32) | 295.29±20.60 (0.10) |
| Inferior | 302.53±62.87 | 267.97±38.13 (<0.001)* | 276.53±72.15 (0.034)* | 267.75±25.28 | 266.50±25.57 (0.34) | 258.80±25.86 (0.13) |
The mean CFT in study group during follow-up is depicted in [Table/Fig-5].
Mean central foveal thickness on follow-up after IVTA injection.
| Study group | Central foveal thickness |
|---|
| Baseline (μm)±SD (μm) | 6 weeks | 12 weeks |
|---|
| (μm)±SD (μm) | p-value | (μm)±SD (μm) | p-value |
|---|
| Posterior uveitis | 330.58±117.04 | 240.08±49.90 | 0.012* | 228.42±41.73 | 0.006* |
| Retinal venous occlusive diseases | 413.13±170.79 | 242.50±81.81 | 0.001* | 297.90±109.08 | 0.014* |
| Eales’ disease | 252.67±94.96 | 197.33±79.18 | 0.006* | 217.33±81.50 | 0.034* |
| Pseudophakic cystoid macular oedema | 632.00 | 162.00 | | 221.00 | |
| Idiopathic cystoid macular oedema | 274.00 | 202.00 | | 263.00 | |
There was a positive but statistically insignificant correlation between baseline CFT and baseline LogMAR visual acuity in study group at 6 weeks (r=0.157, p=0.407) and 12 weeks (r=0.116, p=0.540) follow-up i.e increased CFT was associated with increased in value of LogMAR visual acuity (decline in logMAR visual acuity) [Table/Fig-6].
Relationship between CFT and LogMAR visual acuity on follow-up after IVTA in study group.
| Time of examination | Correlation coefficient (r) | p-value |
|---|
| Baseline-6 weeks | 0.157 | 0.407 |
| Baseline-12 weeks | 0.116 | 0.540 |
There was a positive but statistically insignificant correlation between change in CFT and change in LogMAR visual acuity from baseline to 6 weeks (r=0.351, p=0.058) and 12 weeks (r=0.257, p=0.170) follow-up after IVTA injection in study group [Table/Fig-7].
Relationship between change in CFT and change in LogMAR visual acuity on follow-up after IVTA in study group.
| Time of examination | Correlation coefficient (r) | p-value |
|---|
| Baseline-6 weeks | 0.351 | 0.058 |
| Baseline-12 weeks | 0.257 | 0.170 |
Mean intraocular pressure on follow-up after IVTA: The mean IOP at baseline before IVTA injection in study group was 14.27±3.53 mmHg [Table/Fig-8]. After IVTA statistically significant (p<0.05) elevation in mean IOP from baseline IOP was seen, as depicted in [Table/Fig-8].
Mean intraocular pressure on follow-up after intravitreal triamcinolone acetonide injection.
| Time of examination | Intraocular pressure (mmHg) |
|---|
| Study group | Control group |
|---|
| (Mean±SD) | p-value | (Mean±SD) | p-value |
|---|
| Baseline | 14.27±3.53 | | 14.20±3.25 | |
| 2 weeks | 16.54±4.29 | 0.028* | 14.25±3.01 | 0.190 |
| 4 weeks | 18.54±5.50 | <0.001* | 15.58±3.90 | 0.066 |
| 6 weeks | 19.00±5.98 | <0.001* | 14.53±3.69 | 0.705 |
| 8 weeks | 18.82±5.00 | 0.008* | 13.33±3.45 | 0.205 |
| 12 weeks | 22.50±0.71 | 0.001* | 14.74±3.29 | 0.553 |
Out of 30 eyes in the study group IOP elevation of ≥6 mmHg from baseline was seen in 17 (57.67%) eyes. Out of which 11 (64.71%) were males and 6 (35.29%) were females. The majority i.e., 12 (70.59%) eyes developing IOP elevation ≥6 mmHg belonged to younger age groups who were <30 years of age [Table/Fig-9].
Age and gender wise distribution of cases with intraocular pressure elevation of ≥6 mmHg from baseline.
| Age range (Years) | Total No. of patients (%) | No. of cases with IOP elevation of ≥6 mmHg from baseline |
|---|
| Male | Female | Total (%) |
|---|
| 11-20 | 6 | 2 | 2 | 4 (23.53) |
| 21-30 | 9 | 4 | 4 | 8 (47.06) |
| 31-40 | 2 | 0 | 0 | 0 (00.00) |
| 41-50 | 8 | 5 | 0 | 5 (29.41) |
| 51-60 | 1 | 0 | 0 | 0 (00.00) |
| 61-70 | 3 | 0 | 0 | 0 (00.00) |
| 71-80 | 1 | 0 | 0 | 0 (00.00) |
| Total (%) | 30 | 11 (64.71) | 6 (35.29) | 17 (100.00) |
In 15 out of 17 (88.24%) eyes which developed IOP elevation, IOP was controlled with topical anti-glaucoma medications. However in 2 eyes glaucoma filtering surgery was done to control increased IOP.
The mean intraocular pressure (IOP) at baseline in 30 eyes of 30 controls was 14.20±3.25 mmHg. Beside increase in IOP no other local or systemic complication was seen after IVTA injection up to 12 weeks follow-up.
Discussion
Optical Coherence Tomography (OCT) is a non-contact noninvasive technique that permits in vivo imaging of the eye comprising of the anterior structures of the eye, choroid, optic nerve head, and retina. It is the standard diagnostic modality in the detection, monitoring of treatment and determining prognosis in various inflammatory and oedematous pathologies of posterior segment of eye.
The frequency of application of IVTA injection for the treatment of intraocular oedematous and neovascular diseases has increased exponentially over the last few years. Various studies have reported an improvement in visual acuity after IVTA in various inflammatory diseases of eye. There is a dearth of studies on OCT changes after IVTA in cases of choroiditis and Eales’ disease.
After IVTA injection, mean LogMAR visual acuity in study group improved at 6 weeks (p<0.001) and 12 weeks (p<0.001) follow-up.
After IVTA mean baseline CFT in study group decreased at 6 weeks (p<0.001) and 12 weeks (p<0.001) follow-up. After IVTA injection statistically significant reduction in parafoveal and perifoveal macular thickness in all quadrants was seen at 6 weeks and 12 week follow-up in the study group. In the Control group there were no statistically significant changes in CFT, para foveal and perifoveal thickness at 6 weeks and 12 week follow-up.
Ocular inflammatory diseases have greater potential for visual morbidity and visual loss. Macular oedema is the leading cause of decreased vision in uveitic patients.
In the present study, the mean LogMAR visual acuity in 12 eyes with posterior uveitis improved at 6 weeks (p=0.036) and 12 weeks (p=0.072) follow-up after IVTA injection. In 4 out of 12 eyes with posterior uveitis there was no improvement in LogMAR visual acuity from baseline. Out of those 4 eyes, 2 eyes with central choroiditis had macular scar at presentation, one eye with tubercular retino-choroidal granuloma had multiple pigment epithelial detachments over macula and one eye with Serpiginous Like Choroiditis (SLC) had multiple healed patches of choroiditis over macula at the time of diagnosis. Two patients with SLC enrolled in our study showed hyperreflective fuzzy areas on SD-OCT which involved the RPE, photoreceptor, external limiting membrane, and outer nuclear layer. The inner retinal layers were not involved. In one patient with SLC baseline LogMAR visual acuity was 0.30 and baseline CFT was 216 μM. After IVTA injection at 12 weeks follow-up LogMAR visual acuity improved to 0.00 and CFT decreased to 204 μM. The lesions became discrete and irregular elevations of outer retinal layers appeared. In second patient of SLC there was no change in LogMAR visual acuity due to presence of multiple healed patches of choroiditis over macula at the time of diagnosis. CFT decreased from baseline value of 266 μM to 257 μM at 12 weeks follow-up. Similar findings on OCT were observed by Bansal et al, (2011) [32] in their study to describe changes in high resolution SD-OCT scan with simultaneous fundus autofluorescence signals in tubercular Serpiginous Like Choroiditis (SLC).
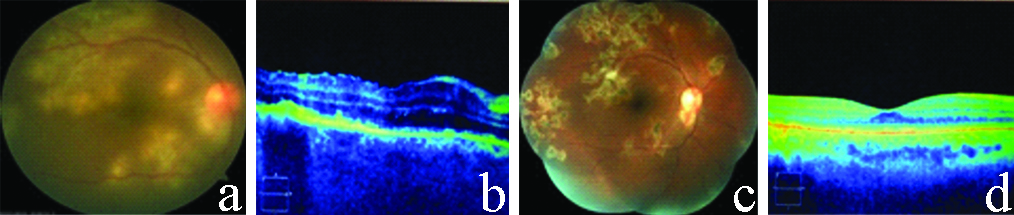
In the present study, one patient of Tubercular multifocal choroiditis had baseline logMAR visual acuity of 0.78 with CFT of 386 μm and severe vitritis, macular oedema, choroidal hyperreflectivity below the RPE and drusen-like material between the RPE and the Bruch membrane on OCT. At 12 weeks follow-up after IVTA injection logMAR visual acuity improved to 0.18 and CFT was decreased to 243 μM. On OCT vitritis subsided and the choroidal hyperreflectivity below the RPE was reduced [Table/Fig-10].
a) Fundus photograph at baseline: showing vitreous haze due to severe vitritis with multiple acute lesions of choroiditis; b) OCT at baseline showing outer retinal and choroidal hyper reflectivity with macular oedema with loss of normal foveal contour, Central foveal thickness: 386 μM. Poor quality of OCT scan due to intense vitreous haze; c) Fundus photograph at 12 weeks after IVTA showing clear media with healed lesions of choroiditis; d) OCT at 12 weeks after IVTA showing decreased choroidal hyper reflectivity and complete resolution of macular oedema with return of normal foveal contour. Central foveal thickness: 243 μM.
In the present study, epiretinal membrane was found in one patient of Tubercular Central choroiditis which was demonstrated by presence of a highly reflective line just above the internal limiting membrane on OCT. We also observed diffuse uveitic macular oedema, CME and serous retinal detachment (SRD) in patients of posterior uveitis enrolled in study group. Iannetti et al, (2008) [33] had also reported the presence of ERM as an important features in patients with uveitis.
Vance et al, (2011) [34] compared the SD OCT findings of multifocal choroiditis and new-onset myopic choroidal neovascularization and reported vitritis, localised choroidal hyperreflectivity below RPE and drusen-like material between RPE and Bruch membrane in acute lesions of multifocal choroiditis while in myopic choroidal neovascularisation, subretinal neovascular pattern, a very thin choroid and posterior staphyloma was found on SD OCT.
Macular oedema is the leading cause of decreased vision in uveitic patients and can lead to permanent visual impairment in 8.5% of cases [35]. In present study the mean CFT in 12 eyes with posterior uveitis was decreased at 6 weeks (p=0.012) and 12 weeks (p=0.006) follow-up after IVTA injection. Similar results were found by Sivaprasad et al., (2007) [24]. They conducted a study to evaluate the therapeutic effect on different morphological patterns of uveitic macular oedema and central macular thickness using OCT.
Retinal vein occlusion (RVO) is the second most common retinal vascular disease after diabetic retinopathy. Macular oedema is the commonest cause of visual impairment in these conditions. It is present in majority of patients with central retinal vein occlusion (CRVO) and 5-15% of patients with branch retinal vein occlusion (BRVO) [36]. In the present study the mean LogMAR visual acuity in 10 eyes with RVO was improved at 6 weeks (p=0.007) and 12 weeks (p=0.007) follow-up.
In present study a statistically significant reduction in mean CFT was found in all eyes with RVO at 6 weeks follow-up but in 2 out of 10 eyes (both were pseudophakic and had CRVO) there was recurrence of macular oedema at 12 weeks follow-up which might be due to rapid clearance of TA from vitreous in pseudophakic compared to phakic eyes [37-38].
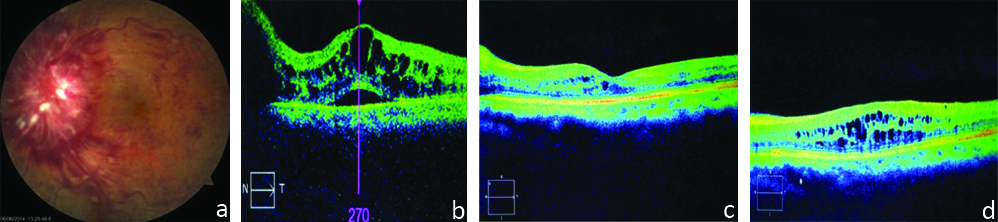
In one out of these 2 eyes baseline LogMAR visual acuity was 1.78 and baseline CFT was 669 μM with multiple cysts in retinal layers on OCT. After IVTA LogMAR visual acuity improved to 0.48 and CFT was decreased to 251 μM at 6 weeks follow-up. But recurrence was seen at 12 week follow-up with decline in LogMAR visual acuity to 0.30 and increased in CFT to 485 μM [Table/Fig-11].
a) Fundus photograph at baseline showing dilated and tortuous vessels with superficial retinal haemorrhages in a all four quadrants of fundus with obscured disc margins; b) OCT at baseline showing multiple cystoid spaces in retinal layers with serous detachment of retina and CFT of 669 μM; c) OCT at 6 weeks after IVTA showing marked decrease in cystoid spaces with resolution of serous detachement and CFT of 251 μM; d) OCT at 12 week after IVTA showing recurrence of multiple cystoid spaces at macula and CFT of 485 μM.
In the other case of RVO the baseline LogMAR visual acuity was 1.78 and baseline CFT was 433 μM with multiple cysts in retinal layers on OCT. After IVTA LogMAR visual acuity improved to 0.48 and CFT decreased to 220 μM at 6 weeks follow-up. At 12 week follow-up recurrence of macular oedema was seen and CFT increased to 321 μM but there was no change in LogMAR visual acuity.
After IVTA injection mean CFT in 10 eyes with RVO was decreased at 6 weeks (p=0.001) follow-up and at 12 weeks it again increased but still when compared with baseline it was found to be statistically significant.
Various studies have reported the role of IVTA in treatment of Eales’ disease [39-40], but there is a dearth of studies on OCT changes after IVTA in cases of Eales’ disease.
The mean CFT in 6 patients with Eales’ disease enrolled in present study was decreased at 6 weeks (p=0.006) and at 12 weeks it again increased but still when compared with baseline it was found to be statistically significant (p=0.034). The mean LogMAR visual acuity in 6 eyes with Eales’ disease was improved at 6 weeks (p=0.040) and 12 weeks (p=0.179) follow-up, after IVTA injection.
Cystoid macular oedema (CME) is a common cause of decreased vision following complicated or uncomplicated cataract surgery. Characteristics of pseudophakic CME on OCT include macular thickening and cystic spaces in the outer plexiform layer, occasionally with subfoveal fluid [41]. In 90% of patients it usually resolves spontaneously and only few patients suffer permanent visual morbidity [42].
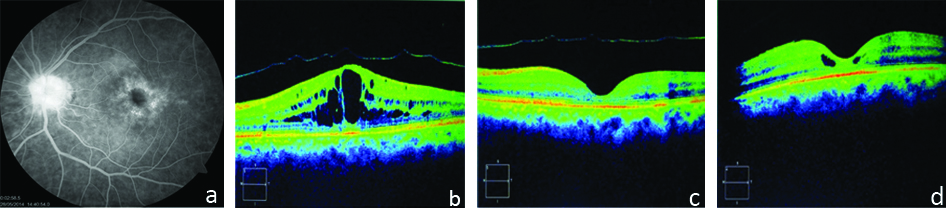
One patient of chronic pseudophakic CME included in our study had multiple large cystic spaces in outer retinal layers with loss of foveal contour on OCT. Baseline LogMAR visual acuity was 1.3 and CFT was 632 μM. After IVTA injection, LogMAR visual acuity improved to 0.78 at 6 weeks and CFT was decreased to 162 μM with disappearance of cystic spaces from retinal layers and returned of normal foveal contour. At 12 weeks follow-up there was recurrence of CME and CFT became 221 μM but still there was further improvement in LogMAR visual acuity to 0.60. The recurrence of macular oedema might be due to rapid clearance of TA from vitreous cavity in pseudophakic eyes compared to phakic eyes [Table/Fig-12].
a) Fundus fluorescein angiography showing characteristic flower petal appearance; b) OCT at baseline showing multiple cystoid spaces in retinal layers with loss of normal foveal contour with posterior vitreous detachment and Central foveal thickness of 632 μM; c) OCT at 6 weeks after IVTA showing complete resolution of CME with return of normal foveal contour with posterior vitreous detachment and CFT of 162 μM; d) OCT at 12 weeks after IVTA showing recurrence of cystoid spaces in retinal layers and CFT of 221 μM.
One patient of idiopathic CME enrolled in our study had LogMAR visual acuity of 0.18 and CFT of 274.00 μM at presentation. At 6 weeks follow-up after IVTA, no improvement was seen in LogMAR visual acuity but CFT was decreased to 202.00 μM. At 12 weeks follow-up CFT increased to 263.00 μM which may be due to rapid clearance of TA from vitreous in pseudophakic eyes. Scott et al, (2003) [31] has also reported the transient change in macular thickness and improvement in VA after IVTA in patients with idiopathic CME.
Various authors have reported decreased CFT to be associated with improvement in LogMAR visual acuity in patients with posterior uveitis [24] retinal venous occlusive diseases following IVTA [27,43], pseudophakic CME [27,30] and idiopathic CME [31].
In present study a positive but statistically insignificant correlation was seen between baseline CFT and baseline LogMAR visual acuity in study group at baseline (r=0.157, p=0.407) and 12 weeks follow-up (r=0.116, p=0.540) i.e increased CFT was associated with increased in value of LogMAR visual acuity (decline in logMAR visual acuity) after IVTA.
In the present study, positive but statistically insignificant correlation was seen between change in CFT and change in LogMAR visual acuity from baseline at 6 weeks follow-up (r=0.351, p=0.058) and at 12 weeks follow-up (r=0.257, p=0.170) after IVTA injection in study group.
The most commonly reported side effect of IVTA is a transient rise in intraocular pressure (IOP) [44-45] leading to a secondary chronic open angle glaucoma [46]. After IVTA injection it increased at 2 weeks, 4 weeks, 6 weeks, 8 weeks and 12 weeks follow-up respectively which was found to be statistically significant (p<0.05) at each follow-up. Out of 30 eyes in the study group IOP elevation of ≥6 mmHg from baseline was seen in 17 (57.67%) eyes. In 15 out of 17 (88.24%) patients who developed IOP elevation, IOP was controlled with topical anti-glaucoma medications. However, two patients underwent filtering glaucoma surgery for controlling raised IOP.
Bakri and Beer (2003) [13] reported more than 5-mmHg elevation in IOP in 48.8% and more than 10 mmHg in 27.9% of patients after IVTA.
A number of other complications associated with IVTA have been reported by various authors like cataract [47], pseudoendophthalmitis [48], infectious endophthalmitis [49], pseudohypopyon [50], ptosis [51] entrapment of triamcinolone behind the lens [52] and conjunctival necrosis [53]. Beside IOP elevation no other local or systemic complication was seen after IVTA injection up to 12 weeks follow-up in our study.
Limitation
Number of cases of each type of disease was quite less. Long term follow-up should have been done to find out recurrence of diseases and long term side effects of IVTA injection eg. Steroid induced cataract.
Conclusion
IVTA injection is a useful method of treatment for oedematous and inflammatory diseases of posterior segment of the eye. Significant improvement of VA was seen after IVTA injection in posterior uveitis, Eales’ disease, RVO, pseudophakic CME and idiopathic cystoid macular oedema. There was significant decrease in macular thickness after IVTA injection in all those cases and there was no recurrence of macular oedema upto 12 weeks of follow-up. After IVTA injection the macular thickness was significantly decreased in eyes with RVO, pseudophakic CME and idiopathic CME at 6 and 12 weeks follow-up but a recurrence in macular oedema was seen in pseudophakic eyes at 12 weeks follow-up most likely due to increased clearance of the drug from vitreous cavity in pseudophakic eyes, thereby decreasing the duration of effect of the drug. Increased macular thickness was associated with decrease in visual acuity in oedematous and inflammatory diseases of posterior segment of the eye. Change in macular thickness after IVTA injection was associated with change in visual acuity in all cases.
After IVTA injection there was significant rise in IOP especially in young males. This increase in IOP was mainly observed within 6 weeks of IVTA injection but in few eyes it developed 12 weeks after injection. Hence all cases should be closely monitored after IVTA injection for an early diagnosis and timely treatment of various complications especially, late rise of intra ocular pressure.