A Novel Laboratory Technique of Fabricating a Definitive Hollow Obturator using Brown Sugar
Sivaranjani Gali1, Aiswarya Premanand2, Hima Bindu Lanka3
1 Associate Professor, Department of Prosthodontics, Faculty of Dental Sciences, Ramaiah University of Applied Sciences, Bangalore, Karnataka, India.
2 Undergraduate Student, Department of Prosthodontics, Faculty of Dental Sciences, Ramaiah University of Applied Sciences, Bangalore, Karnataka, India.
3 Postgraduate Student, Department of Prosthodontics, Faculty of Dental Sciences, Ramaiah University of Applied Sciences, Bangalore, Karnataka, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Sivaranjani Gali, M S Ramaiah University of Applied Sciences, New BEl Road, Bangalore-560054, Karnataka, India.
E-mail: nature79gali@gmail.com
Obturators are prostheses that help to seal congenital or acquired tissue openings of hard, soft palate and adjacent structures and restore patient’s lost function, comfort and aesthetics. In the process of its fabrication, the extension of the obturator often depends on the patient’s presentation of the tissue defect. In large maxillofacial defects, the retention of the obturator is often compromised due to increased inter-ridge distance and the weight of the prosthesis. In such cases, light weight hollow obturators can enhance the retention, stability of the prosthesis and further improve patient comfort. Brown sugar is soluble in water and can be shaped with ease and removed from the prosthesis, without leaving any residue. We propose an investment technique using brown sugar as a three dimensional spacer for fabricating hollow obturator. Solubility of brown sugar over the commonly used hollow spacer materials such as salt and granulated sugar was compared and further verified for any residues in the hollow obturator. Uniform thickness of the obturator wall has been accomplished through use of heat polymerized pellets on the tissue surface of the obturator mould.
Definitive obturators, Hollow obturators, Maxillofacial prosthesis
Introduction
Prosthetic rehabilitation for patients with congenital or acquired defects of palatal tissues is provided in the form of obturators. Definitive obturators must fulfil basic requirements of being light weight, stable and restore the patient’s lost function and aesthetics. In large maxillofacial defects, the retention of the obturator is often compromised due to increased inter-ridge distance and the weight of the prosthesis [1]. Techniques using various materials and techniques of fabricating light weight hollow obturators have been proposed to improve obturator retention, stability and patient comfort. A hollow space can be created in the denture in order to decrease its overall weight and has been experimentally found that the weight of the denture could be significantly reduced by creating a hollow space [2-7]. In the proposed technique, brown sugar is used as the three dimensional spacer to create a hollow space. The prime advantage of brown sugar is that it is highly soluble, has the ease of removal from the hollow bulb, while providing a uniform thickness of the obturator. Solubility of brown sugar over the commonly used hollow spacer materials such as salt and granulated sugar was calculated from the percentage ratio of the mass of solute to the mass of the solvent [8]. The weighed amount of the above mentioned spacer materials such as salt and granulated sugar, as solutes were gradually added to 100 mL of the distilled water as the solvent till the saturation point and their respective solubilities were measured as an average of three readings by the authors. Uniform thickness of the tissue bearing surface of the obturator is essential to achieve the objective of reduced weight of the prosthesis. This has been accomplished in the proposed technique through use of heat polymerized pellets on the tissue surface of the obturator mould.
Procedure
Dewax the waxed up obturator following conventional procedures [Table/Fig-1].
Conventional procedure of dewaxing the obturator.
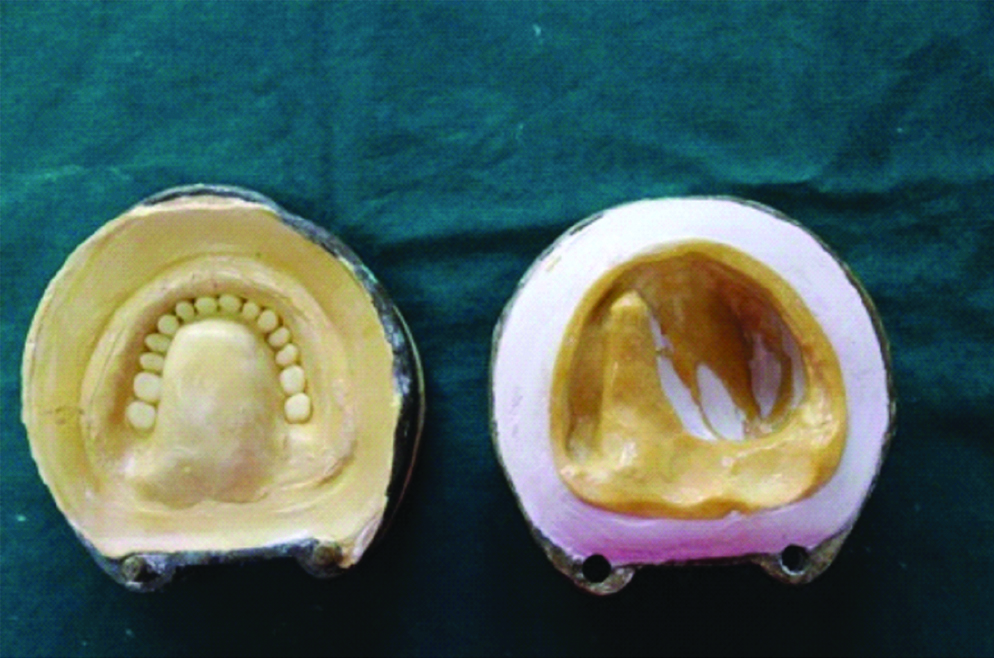
Use heat polymerised acrylic resin (Acralyn H, DPI) to fabricate 2×2×1 mm pellets, and secure the pellets to the hard tissue bearing areas of the master cast with cyanoacrylate to ensure uniform thickness of the obturator [Table/Fig-2].
Heat polymerized pellets placed over the mould.
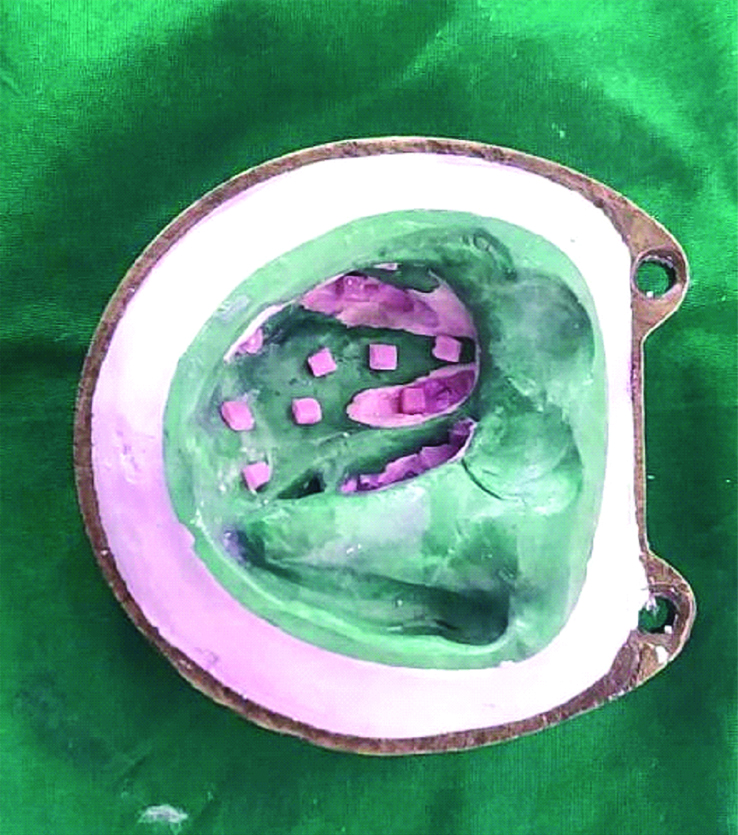
Shape the brown sugar to the defect area of the obturator by mildly warming with Bunsen Burner and then subsequently cooling it [Table/Fig-3].
Brown sugar (without the cellophane sheet) over the wax up of the defect area.
Pack the heat polymerized acrylic resin into the mould of the counter flask and place the shaped brown sugar.
Process the conventional heat polymerizing acrylic resin (Acralyn H, DPI) definitive obturator [Table/Fig-4].
Heat polymerized obturator with heat polymerized pellets.
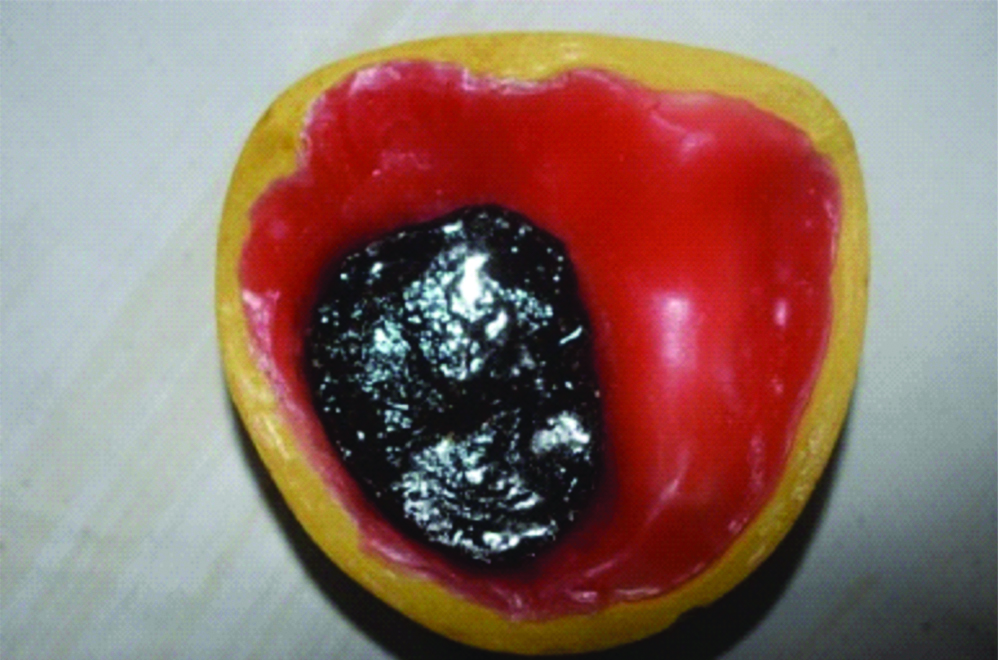
After deflasking, drill two holes (2 mm, diameter) on the palatal aspect of the obturator and inject hot water into the holes with a syringe to flush out the brown sugar [Table/Fig-5].
Holes drilled to remove the brown sugar.
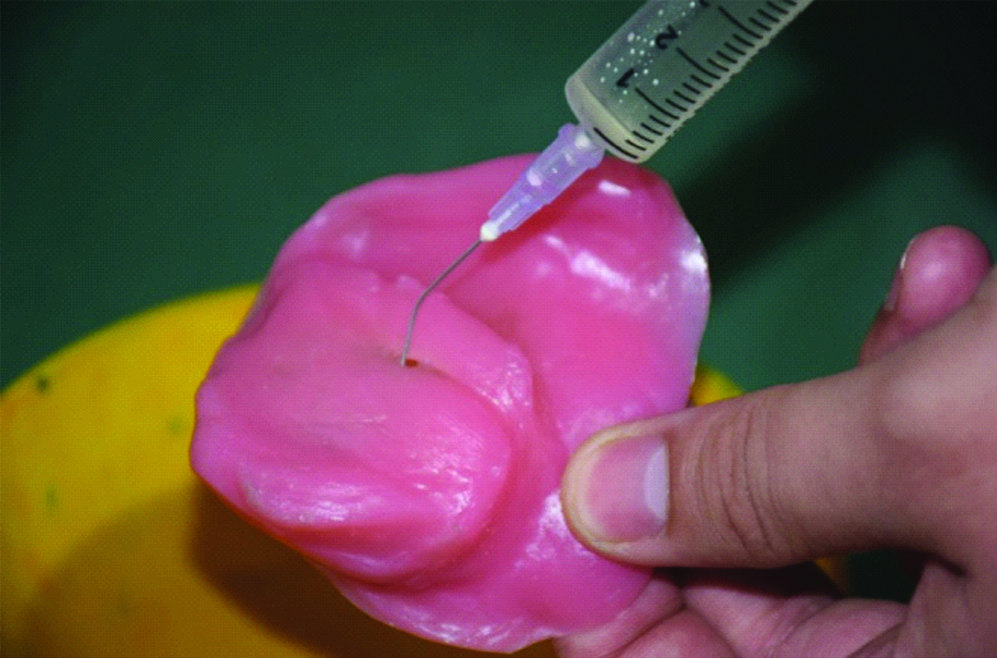
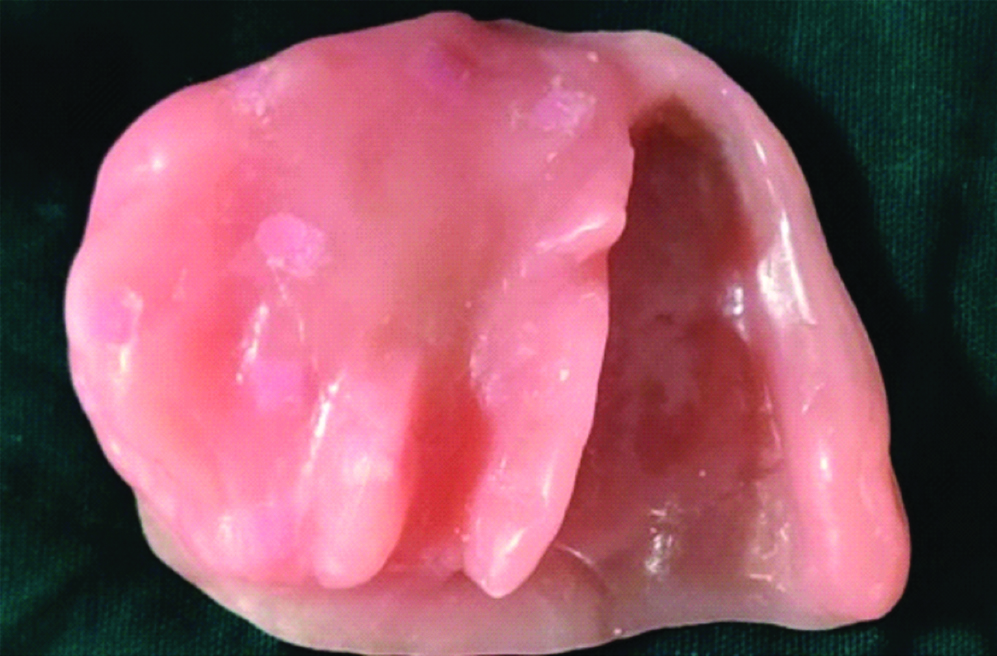
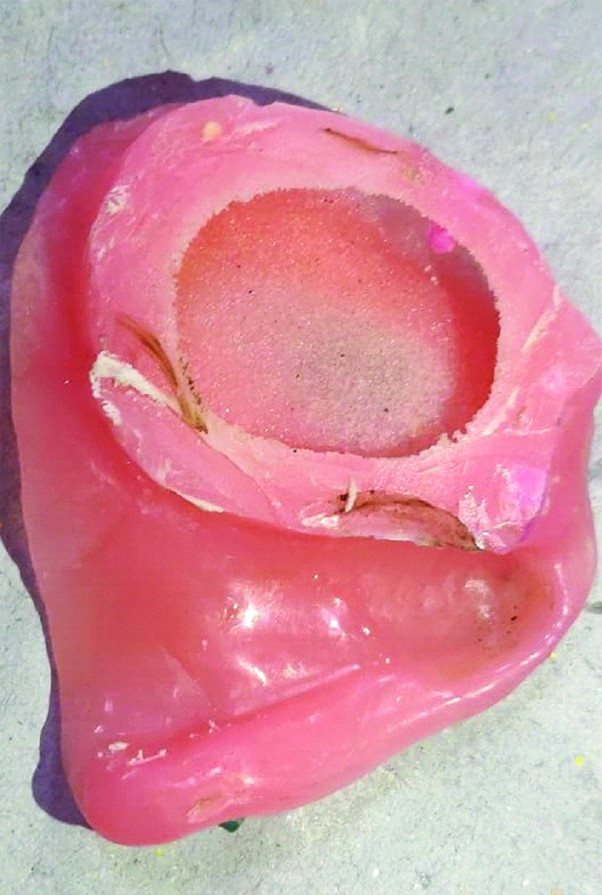
Once the brown sugar dissolves, the holes can be filled with auto-polymerizing resin followed by finishing and polishing [Table/Fig-6].
Hollow obturator (with the brown sugar dissolved).
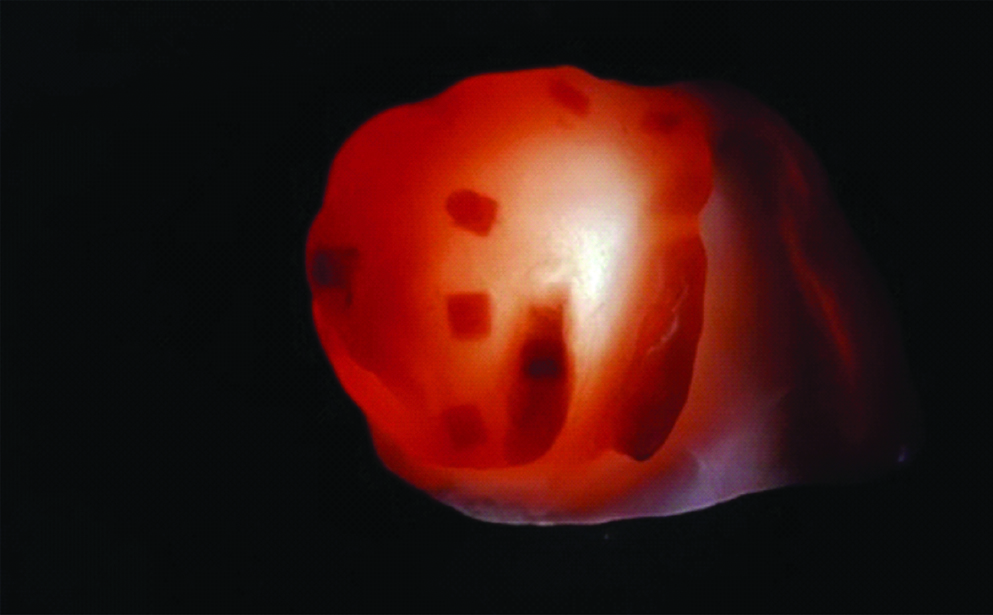
Discussion
The technique can be used for patients requiring light weight interim or definitive obturators. Brown sugar was used as a three dimensional spacer to create a hollow space for the obturator due to its high solubility and the ease of removing it from the hollow bulb. The graphic representation of the solubility of brown sugar, salt and granulated sugar is presented in [Table/Fig-7] [8]. The high solubility of brown sugar can be attributed to the molasses present in brown sugar with its hygroscopic property [9]. The apparent reduction in the weights of the solid and hollow obturator using the brown sugar can be deciphered in [Table/Fig-8] [10]. We further sectioned the obturator prosthesis to verify residues of brown sugar. As shown in [Table/Fig-9], with no residues of brown sugar, the solubility of brown sugar can be vindicated. However, roughness can be observed on the hollow surface of the obturator, indicating that the surface details of the obturator in terms of strength and porosity can be affected by the spacer material. Brown sugar available as granulated powder, was dry flamed for few minutes and as it softens, can take shape of the defect and was later cooled to a firm solid spacer. It has advantage of mouldability, to be able to adapt to the obturator defect, unlike the other spacers such as salt or sugar can also be viewed as a limitation of additional procedure. Brown sugar has the advantage of ease of customising to the defect without a cellophane sheet, unlike Dipal PM et al., alum technique, which has the limitation of leaving cellophane in the prosthesis and the difficulty in shaping the alum crystals to the defect [11]. Achieving a uniform thickness of the obturator has been attempted by various authors through lost wax technique, asbestos sheet and auto-polymerized acrylic resin which are time consuming and complicated [5,12]. Heat polymerised pellets were used for creating uniform thickness of the obturator to ease the multi-seam appearance with auto-polymerized resin as shown in [Table/Fig-6] [11].
Solubility of brown sugar compared to salt and granulated sugar.
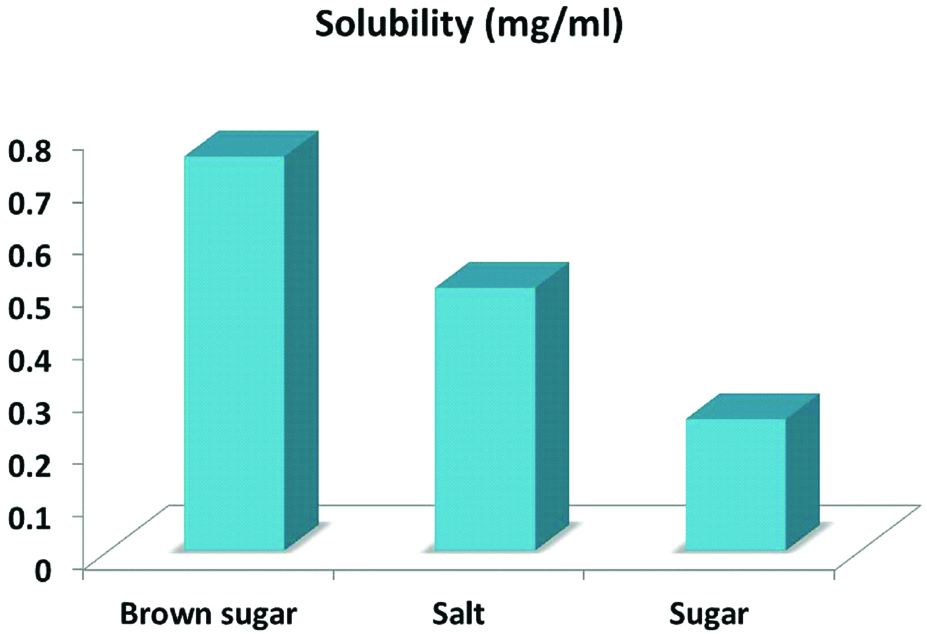
Comparison of the weights of solid and hollow obturator.
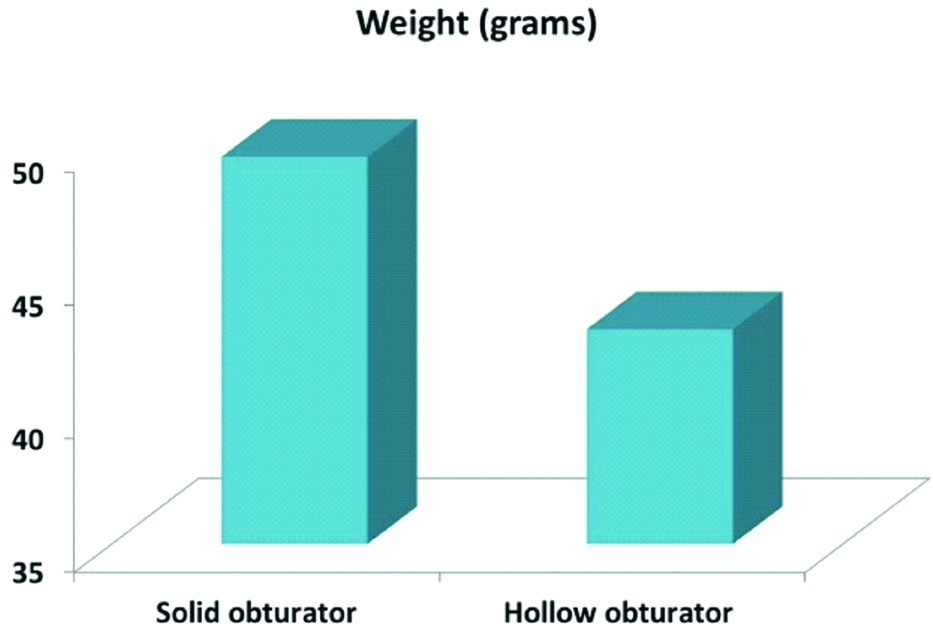
Sectioned obturator with no residues of brown sugar.
Conclusion
The solubility of brown sugar and its ease of removal from the mould, make brown sugar suitable as a three dimensional spacer for fabricating hollow definitive obturators.
[1]. Karen SM, Sandra R, Glenn EM, An innovative investment method for the fabrication of a closed hollow obturator prosthesisJ Prosthet Dent 1998 80:129-32.10.1016/S0022-3913(98)70098-8 [Google Scholar] [CrossRef]
[2]. Glenn EM, Donald N, Sandra LR, An alternative method for fabrication of a closed hollow obturatorJ Prosthet Dent 1986 55:48510.1016/0022-3913(86)90183-6 [Google Scholar] [CrossRef]
[3]. Bhushan P, Aras MA, Chitre V, Mysore AR, Mascarenhas K, Kumar S, The hollow maxillary complete denture: A simple, precise, single-flask technique using a caramel spacerJ Prosthodont 2019 28:e13e1710.1111/jopr.1261628383131 [Google Scholar] [CrossRef] [PubMed]
[4]. Brown KE, Fabrication of a hollow bulb obturatorJ Prosthet Dent 1969 21:97-103.10.1016/0022-3913(69)90035-3 [Google Scholar] [CrossRef]
[5]. Worley JL, Kneijski ME, A method for controlling the thickness of the hollow obturator prosthesisJ Prosthet Dent 1983 50:227-29.0.1016/0022-3913(83)90022-7 [Google Scholar] [CrossRef]
[6]. Holt RA, Jr, A hollow complete lower dentureJ Prosthet Dent 1981 45:45210.1016/0022-3913(81)90112-8 [Google Scholar] [CrossRef]
[7]. DaBreo EL, A light cured interim obturator prosthesis: A clinical reportJ Prosthet Dent 1990 63:371-73.10.1016/0022-3913(90)90222-X [Google Scholar] [CrossRef]
[8]. https://sciencing.com/calculate-solubilities-5179123.html [Google Scholar]
[9]. Schneider A, Method of fabricating a hollow obturatorJ Prosthet Dent 1978 40:351https://en.wikipedia.org/wiki/Brown_sugar10.1016/0022-3913(78)90046-X [Google Scholar] [CrossRef]
[10]. Yn-low W, Norman GS, Comparison of weight reduction in different designs of solid and hollow obturator prosthesesJ Prosth Dent 1989 62(2):214-17.10.1016/0022-3913(89)90317-X [Google Scholar] [CrossRef]
[11]. Dipal PM, Muddugangadhar BC, Arindham D, Vishal K, Flasking technique with alum crystals for fabricating definitive hollow bulb obturatorsJ Prosthet Dent 2017 120:144-46.10.1016/j.prosdent.2017.09.01229258691 [Google Scholar] [CrossRef] [PubMed]
[12]. Pravinkumar GP, Smita PP, A hollow definitive obturator fabrication technique for management of partial maxillectomyJ Adv Prosthodont 2012 4:248-53.10.4047/jap.2012.4.4.24823236579 [Google Scholar] [CrossRef] [PubMed]