Adult intussusception is a rare condition and can be secondary to an intestinal lipoma. In this case report, a 41-year-old woman presented with an acute abdominal pain and a tender central abdominal mass. Abdominal computed tomography scan showed an ileo-ileal intussusception with a fat-density mass at the leading point. Laparotomy with reduction of the intussusception, bowel resection and anastomosis was performed. Histological examination revealed a benign submucosal lipoma.
Early laparotomy with resection and without deintussusception is usually recommended. In this case, a careful reduction allowed to preserve the non necrotic intestinal segment involved in the intussusception.
Abdominal pain, Intestinal resection, Surgery
Case Report
A 41-year-old woman presented with an acute central abdominal pain associated with vomiting, 24 hours prior to admission. She had no fever, no blood in stools nor changes in bowel habits. No previous similar episode was reported.
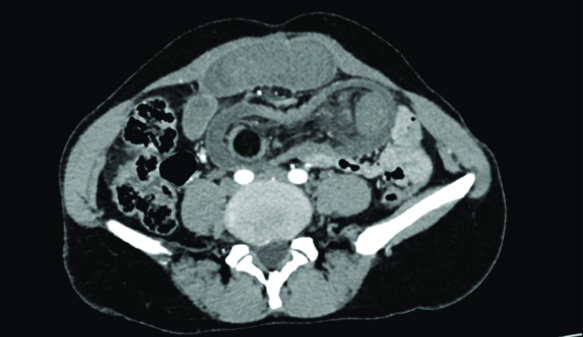
Abdominal examination revealed a central tender sausage-shaped mass with no other significant physical findings. Blood tests were normal, except white blood cell count of 13500/mL. Abdominal CT scan showed a segment of ileo-ileal intussusception. Moreover, a rounded well-limited low-density lesion was identified as the lead point causing the intussusception [Table/Fig-1,2]. There were no signs of obstruction and no other lesions were found.
Abdominal computed tomography scan showing a rounded fatty mass in the small intestine.
Abdominal computed tomography scan. Coronal view showing the “sausage” shape of the intussusception.
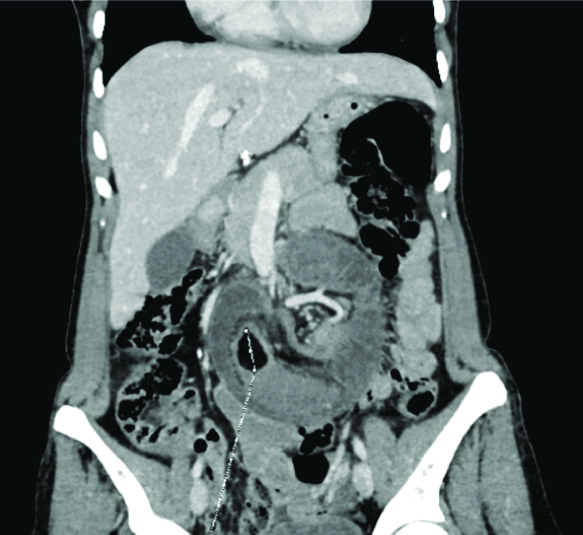
The patient was diagnosed preoperatively as having an ileo-ileal intussusception caused by a lipoma in the small intestine, relying on the CT scan findings that showed the low density lesion with lipid attenuation. Laparotomy confirmed the presence of enteroenteric intussusception involving the proximal Ileum [Table/Fig-3]. A manual reduction was gently performed. The length of the intussuscepted ileal segment was 120 cm in which 50 cm were necrotic [Table/Fig-4]. The leading point was a palpable endoluminal rounded mass which was resected with the necrotic bowel, 70 cm in total. Primary anastomosis was performed. The tumour appeared macroscopically as fatty tissue [Table/Fig-5]. Pathological examination revealed a benign submucosal lipoma. Postoperative course was uneventful and the patient was discharged on the 6th postoperative day.
Discussion
Adult intestinal intussusception is a rare clinical entity. Usually the underlying cause is a malignant or a benign tumour [1,2]. Intestinal lipoma has been reported among the benign causes. It accounts for 2% of all gastro-intestinal tumours. It can act as the leading point of the intussusception due to its intraluminal location [3]. Intestinal lipomas were found in the ileum in 22 cases among the 51 cases as reported by Mouaqit O et al., [3]. About 23 more cases of intestinal intussusceptions caused by lipomas, in the English literature was compiled since August 2012. Lipomas were located in the ileum in nine cases [Table/Fig-6] [3-25]. The clinical presentation is non-specific and the typical clinical triad of abdominal pain, a sausage-shaped mass and red jelly stools, usually lacks in adults making this condition difficult to diagnose [26].
Intraoperative findings: Ileoileal intussusception with signs of ischemia.
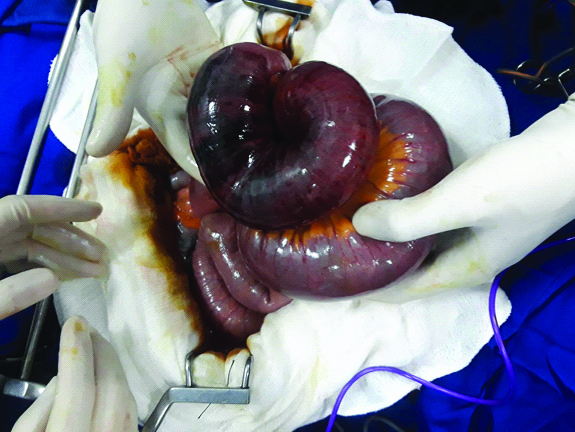
Intraoperative findings: After partial reduction. Intussuscepted segment with both necrotic and viable bowel.
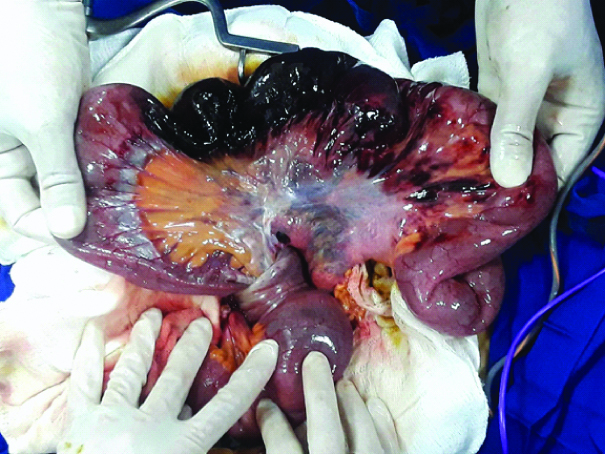
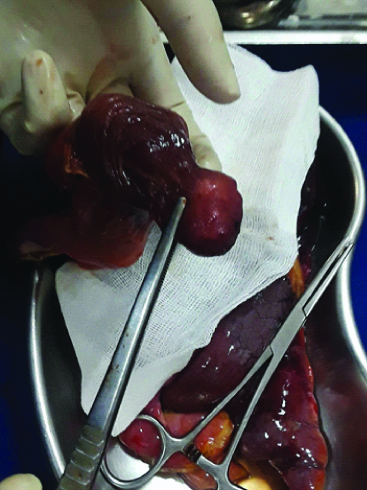
Intraoperative findings: Submucosal rounded fatty mass.
Case reports of intestinal intussusceptions caused by lipomas reported in the English literature since August 2012 [3-25].
| Gender | Age | DG | Location | Size (cm) | Treatment | Author | Year |
|---|
| Male | 55 | CT | Colon | 3 | Right hemicolectomy | Mouaqit O et al., [3] | 2013 |
| Female | 52 | CT* | Ileum | 6 | Ileal resection | Uyulmaz S et al., [4] | 2018 |
| Male | 22 | CT | Ileum | - | Ileal resection | Vagholkar K et al., [5] | 2015 |
| Male | 50 | CT | Ileum | 4 | Ileal resection | Jiang RD et al., [6] | 2015 |
| Female | 45 | CT | Ileum | - | Ileal resection | Fazeli MS et al., [7] | 2014 |
| Female | 52 | CT, Colonoscopy | Ileum | 0,3-5 | Ileal resection | Gao PJ et al., [8] | 2014 |
| Female | 30 | US | Ileum | 3 | Ileocaecal resection | Bosman WM et al., [9] | 2014 |
| Female | 30 | CT | Ileum | - | Right hemicolectomy | Molnar C et al., [10] | 2013 |
| Female | 73 | CT, Colonoscopy | Ileum | 3 | Endoscopic | Lee ES et al., [11] | 2013 |
| Male | 55 | Laparotomy | Ileum | 4 | Ileal resection | Singhal S et al., [12] | 2012 |
| Male | 40 | CT, Colonoscopy | Colon | 6 | Segmental colectomy | M’rabet S et al., [13] | 2018 |
| Female | 65 | Laparotomy | Colon | 9 | Left hemicolectomy | Ongom PA et al., [14] | 2012 |
| Female | 44 | CT | Jejunum | 3 | Jejunal resection | Seow-En I et al., [15] | 2014 |
| Male | 47 | CT | Ileocaecal valve | 3 | Ileo-caecal resection | Kumar K et al., [16] | 2017 |
| Female | 47 | CT | Colon | 9 | Right hemicolectomy | Casiraghi T et al., [17] | 2016 |
| Male | 50 | CT, Sigmoidoscopy | Colon | 6 | Left hemicolectomy | Low HM et al., [18] | 2016 |
| Male | 57 | CT, Colonoscopy | Colon | 6 | Segmental colectomy | De Figueiredo LO et al., [19] | 2016 |
| Female | 52 | US*, CT | Ileocaecal valve | 5 | Right hemicolectomy | Stancu B et al., [20] | 2016 |
| Male | 44 | CT | Colon | 6 | Right hemicolectomy | Arslan E et al., [21] | 2017 |
| Female | 73 | US, CT | Ileocaecal valve | 6 | Right hemicolectomy | Gys B et al., [22] | 2015 |
| Female | 65 | CT, Colonoscopy | Ileocaecal valve | 7 | | Kang B et al., [23] | 2014 |
| Male | 56 | CT | Colon | - | Right hemicolectomy | Eyselbergs M et al., [24] | 2014 |
| Female | 54 | CT | Colon | 6 | Left hemicolectomy | Grasso E et al., [25] | 2012 |
*CT: Computed tomography, *US: Ultrasonography
The best diagnostic modality is abdominal CT scan [27]. The finding of lipid attenuation (-100 to -50 HU) is mandatory to the diagnosis of a lipoma [28,29]. To avoid mistaking the lipoma for intraluminal gas or invaginated mesenteric fat, the observation of the images reformatted in multiple dimensions, with the optimal window and oral contrast filling of the bowel can be needed [30]. Possible vascular compromise is difficult to assess on axial images with conventional CT scan. A much better assessment of the vascular supply to the affected bowel loop and of the intussusception length can be made using multidetector CT [31]. In our patient preoperative diagnosis was made successfully supported by CT scan findings. Other modalities include colonoscopy which allows a direct visualisation of the lipoma and it is more appropriate to assess colonic localisation [13]. Nevertheless, colonoscopy was useful for the diagnosis for ileal lipoma with ileo-colic intussusception in two case [8,31]. The other diagnostic tools reported are ultra-sonography, barium studies and video capsule endoscopy [3]. Intraoperative diagnosis during exploratory laparotomy were reported in two cases [12,14].
Laparotomy with bowel resection and primary anastomosis is the treatment of choice. In colonic intussusceptions, it is recommended to perform resection in block without reduction. For entero-enteric cases, a selective approach can be applied. Reduction is not recommended when signs of bowel ischemia or inflammation are present or malignancy is suspected [15,28]. Intraoperative reduction of the instussusception prior to resection may preserve a considerable length of bowel [4,5]. In this case, the preoperative diagnosis of ileal lipoma being made, the involved bowel segment was long and even though the bowel showed signs of ischemia, we attempted reduction successfully, which allowed us to spare 50 cm of bowel length. This method could have caused inadvertent bowel injury that is why it should be performed gently. Reduction should be abandoned and followed by resection anastomosis if the attempt is not harmless and successful [32].
Conclusion
Submucosal intestinal lipoma can cause intussusception presenting as an acute tender abdominal mass. The preoperative diagnosis is possible with CT scan; showing a target sign or a pseudo kidney sign with a fat-density lead point. Early surgery allows definitive diagnosis and treatment which is resection with primary anastomosis.
*CT: Computed tomography, *US: Ultrasonography
[1]. Bilgin M, Toprak H, Cheikh Ahmad I, Yardimci E, Kocakoc E, Ileocecal Intussusception due to a Lipoma in an AdultCase Rep Surg 2012 2012:68429810.1155/2012/68429822991683 [Google Scholar] [CrossRef] [PubMed]
[2]. Aminian A, Noaparast M, Mirsharifi R, Bodaghabadi M, Mardany O, Ali FA, Ileal intussusceptions secondary to both lipoma and angiolipoma: A case reportCases J 2009 2:709910.4076/1757-1626-2-709919829910 [Google Scholar] [CrossRef] [PubMed]
[3]. Mouaqit O, Hasnai H, Chabani L, Benjelloun B, El Bouhaddouti H, Ibn el Majdoub K, Adult intussusceptions caused by a lipoma in the jejunum: report of a case and review of the literatureWorld J Emerg Surg 2012 7:2810.1186/1749-7922-7-2822913731 [Google Scholar] [CrossRef] [PubMed]
[4]. Uyulmaz S, Zünd M, Caspar U, Diebold J, Slankamena K, Ileoileal intussusception in unspecific recurrent abdominal pain in adult: A case reportSAGE Open Med Case Rep 2018 6:2050313X1879281410.1177/2050313X1879281430116530 [Google Scholar] [CrossRef] [PubMed]
[5]. Vagholkar K, Chavan R, Mahadik A, Maurya I, Lipoma of the small intestine: a cause for intussusception in adultsCase Reports in Surgery [online] 2015 2015:856030http://dx.doi.org/10.1155/2015/85603010.1155/2015/85603026295002 [Google Scholar] [CrossRef] [PubMed]
[6]. Jiang RD, Zhi XT, Zhang B, Chen ZQ, Li T, Submucosal lipoma: a rare cause of recurrent intestinal obstruction and intestinal intussusceptionJ Gastrointest Surg 2015 19(9):1733-35.10.1007/s11605-015-2824-125895980 [Google Scholar] [CrossRef] [PubMed]
[7]. Fazeli MS, Kazemeini A, Elyasinia F, Parsaei R, Adult ileo-ileal intussusception caused by intestinal lipomaIran J Med Sci 2014 39(6):589-90. [Google Scholar]
[8]. Gao PJ, Chen L, Wang FS, Zhu JY, Ileo-colonic intussusception secondary to small-bowel lipomatosis: A case reportWorld J Gastroenterol 2014 20(8):2117-19.10.3748/wjg.v20.i8.211724587685 [Google Scholar] [CrossRef] [PubMed]
[9]. Bosman WM, Veger HT, Hedeman Joosten PP, Ritchie ED, Ileocaecal intussusception due to submucosal lipoma in a pregnant womanBMJ Case Rep [online] 2014 2014:20311010.1136/bcr-2013-20311010.1136/bcr-2013-20311024532237 [Google Scholar] [CrossRef] [CrossRef] [PubMed]
[10]. Molnar C, Neagoe V, Nicolescu C, Pantiru A, Tudor A, Roşca C, Ileo-ceco-descendento-colic intussusception in adult-a case reportChirurgia 2013 108(6):892-95. [Google Scholar]
[11]. Lee ES, Lee KN, Choi KS, Lee HK, Jun DW, Lee OY, Endoscopic treatment of a symptomatic ileal lipoma with recurrent ileocolic intussusceptions by using cap-assisted colonoscopyClin Endosc 2013 46(4):414-17.10.5946/ce.2013.46.4.41423964343 [Google Scholar] [CrossRef] [PubMed]
[12]. Singhal S, Singhal A, Arora PK, Tugnait R, Tiwari B, Malik P, Adult Ileo-Ileo-Caecal Intussusception: Case Report and Literature ReviewCase Rep Surg 2012 2012:78937810.1155/2012/78937823346450 [Google Scholar] [CrossRef] [PubMed]
[13]. M’rabet S, Jarrar MS, Akkari I, Ben Abdelkader A, Srihac B, Hamila F, Colonic intussusception caused by a sigmoidal lipoma: A case reportInt J Surg Case Rep 2018 50:1-4.10.1016/j.ijscr.2018.06.00930059860 [Google Scholar] [CrossRef] [PubMed]
[14]. Ongom PA, Wabinga H, Lukande RL, A ‘giant’ intraluminal lipoma presenting with intussusception in an adult: A case reportJ of Med Case Rep 2012 6:37010.1186/1752-1947-6-37023107601 [Google Scholar] [CrossRef] [PubMed]
[15]. Seow-En I, Foo FJ, Tang CL, BMJ Case Rep Published online: 2014 October [08/02/2018]10.1136/bcr-2014-20729725355752 [Google Scholar] [CrossRef] [PubMed]
[16]. Kumar K, Noori MR, Patel KM, Yuen W, Bello C, Rare diagnosis of intestinal lipomatosis complicated by intussusception in an adult: A case reportInt J Surg Case Rep 2017 39:339-42.10.1016/j.ijscr.2017.08.03828898799 [Google Scholar] [CrossRef] [PubMed]
[17]. Casiraghi T, Masetto A, Beltramo M, Girlando M, Di Bella C, Intestinal obstruction caused by ileocolic and colocolic intussusception in an adult patient with cecal lipomaCase Rep Surg Published online: 2016 october [08/02/2018] 10.1155/2016/351960628044120 [Google Scholar] [CrossRef] [PubMed]
[18]. Low HM, Chinchure D, Clinics in diagnostic imaging (172). Colocolic intussusception with a lipoma as the lead pointSingapore Med J 2016 57(12):664-68.10.11622/smedj.201618127995264 [Google Scholar] [CrossRef] [PubMed]
[19]. De Figueiredo LO, Garcia DPC, Alberti LR, Paiva RA, Petroianu A, Paolucci LB, Colo-colonic intussusception due to large submucous lipoma: A case reportInt J Surg Case Rep 2016 28:107-10.10.1016/j.ijscr.2016.09.00627693869 [Google Scholar] [CrossRef] [PubMed]
[20]. Stancu B, Chira A, Chira RI, Grigorescu I, Gherman CD, Dumitraşcu DL, Ileo-colic intussusception by ileo-cecal valve lipoma-an infrequent ultrasonographic occurrence. A case reportMed Ultrason 2016 18(3):394-96.10.11152/mu.2013.2066.183.ile27622418 [Google Scholar] [CrossRef] [PubMed]
[21]. Arslan E, Çağlayan K, Sipahi M, Banlı O, Gündoğdu F, Şahin S, Intussusception of the bowel in adults: two different casesTurk J Surg 2015 33(3):217-19.10.5152/UCD.2015.300128944338 [Google Scholar] [CrossRef] [PubMed]
[22]. Gys B, Haenen F, Gys T, Ileocolic intussusception caused by a giant ulcerating lipoma of bauhin’s valve: an unusual cause of intestinal obstruction in the adultIndian J Surg 2015 77(Suppl 1):01-02.10.1007/s12262-013-1023-025972625 [Google Scholar] [CrossRef] [PubMed]
[23]. Kang B, Zhang Q, Shang D, Ni Q, Muhammad F, Hou L, Resolution of intussusception after spontaneous expulsion of an ileal lipoma per rectum: a case report and literature reviewWorld J Surg Oncol 2014 12:14310.1186/1477-7819-12-14324884620 [Google Scholar] [CrossRef] [PubMed]
[24]. Eyselbergs M, Ceulemans LJ, De Bontridder S, Vanhoenacker F, Van Overbeke L, Quanten I, Ileocolic intussusception due to lipomatosis of the ileum: a common complication of a rare clinical entityJBR-BTR 2014 97(1):36-38.10.5334/jbr-btr.324765771 [Google Scholar] [CrossRef] [PubMed]
[25]. Grasso E, Guastella T, Giant submucosal lipoma cause colo-colonic intussusception. A case report and review of literatureAnn Ital Chir 2012 83(6):559-62. [Google Scholar]
[26]. Shehzad KN, Monib S, Ahmad OF, Riaz AA, Submucosal lipoma acting as a leading point for colo-colic intussusception in an adultJ Surg Case Rep 2013 2013(10):rjt088Available from: https://doi.org/10.1093/jscr/rjt08810.1093/jscr/rjt08824964327 [Google Scholar] [CrossRef] [PubMed]
[27]. Goh BK, Quah HM, Chow PK, Tan KY, Tay KH, Eu KW, Predictive factors of malignancy in adults with intussusceptionWorld J Surg 2006 30:1300-04.10.1007/s00268-005-0491-116773257 [Google Scholar] [CrossRef] [PubMed]
[28]. Ross GJ, Amilineni V, Case 26: Jejunojejunal intussusceptions secondary to a lipomaRadiology 2000 216:727-30.10.1148/radiology.216.3.r00se3372710966702 [Google Scholar] [CrossRef] [PubMed]
[29]. Drop A, Czekajska-Chehab E, Maciejewski R, Giant retroperitoneal lipomas-radiological case reportAnn Univ Mariae Curie Sklodowska Med 2003 58:142-46. [Google Scholar]
[30]. Fang SH, Dong DJ, Chen FH, Jin M, Zhong BS, Small intestinal lipomas: Diagnostic value of multi-slice CT enterographyWorld J Gastroenterol 2010 16(21):2677-81.10.3748/wjg.v16.i21.267720518091 [Google Scholar] [CrossRef] [PubMed]
[31]. Lin HH, Chan DC, Yu CY, Chao YC, Hsieh TY, Is this a lipoma?The Am J of Med 2008 121(1):21-23.10.1016/j.amjmed.2007.09.00918187069 [Google Scholar] [CrossRef] [PubMed]
[32]. Meshikhes AWN, Al-Momen SAM, Al Talaq FT, Al-Jaroof AH, Adult intussusception caused by a lipoma in the small bowel: Report of a caseSurg Today 2005 35(2):161-63.10.1007/s00595-004-2899-x15674501 [Google Scholar] [CrossRef] [PubMed]