Novel Treatment for Hard-to-Heal Chronic Plantar Ulcers in Hansen’s Disease
Gatha M Upadya1, Srinidhi Govindarajan2
1 Professor and Head, Department of Dermatology, Kasturba Medical College, Manipal Academy of Higher Education, Mangalore, Karnataka, India.
2 Undergraduate Medical Student, Department of Dermatology, Kasturba Medical College, Manipal Academy of Higher Education, Mangalore, Karnataka, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Gatha M Upadya, Professor and Head, Department of Dermatology, Kasturba Medical College, Manipal Academy of Higher Education, Mangalore-575001, Karnataka, India.
E-mail: gathaupadya@hotmail.com
Hansen’s disease is an important public health problem and it is one of the important cause of disability in patients with non-healing trophic ulcer in Hansen’s disease, and also the long-term management of these trophic ulcers works out to be very costly. Reduction in the healing time would be a major step in the rehabilitation of these patients.
Authors hereby present one such case of chronic plantar ulcer in Hansen’s patient which was refractory to standard treatment like oral and topical antibiotics and daily dressings for more than six years. Hence, Platelet Rich Fibrin Matrix (PRFM) was applied along with adequate rest using Plaster of Paris (POP) cast. The wound was opened and the dried PRFM was cleared from the bed of the wound after 10 days. Procedure was repeated every third week. This led to dramatic healing of the ulcer with a reduction in wound diameter with no noticeable side-effects.
Leprosy patients, New treatment, Platelet rich fibrin matrix, Resistant plantar ulcers
Case Report
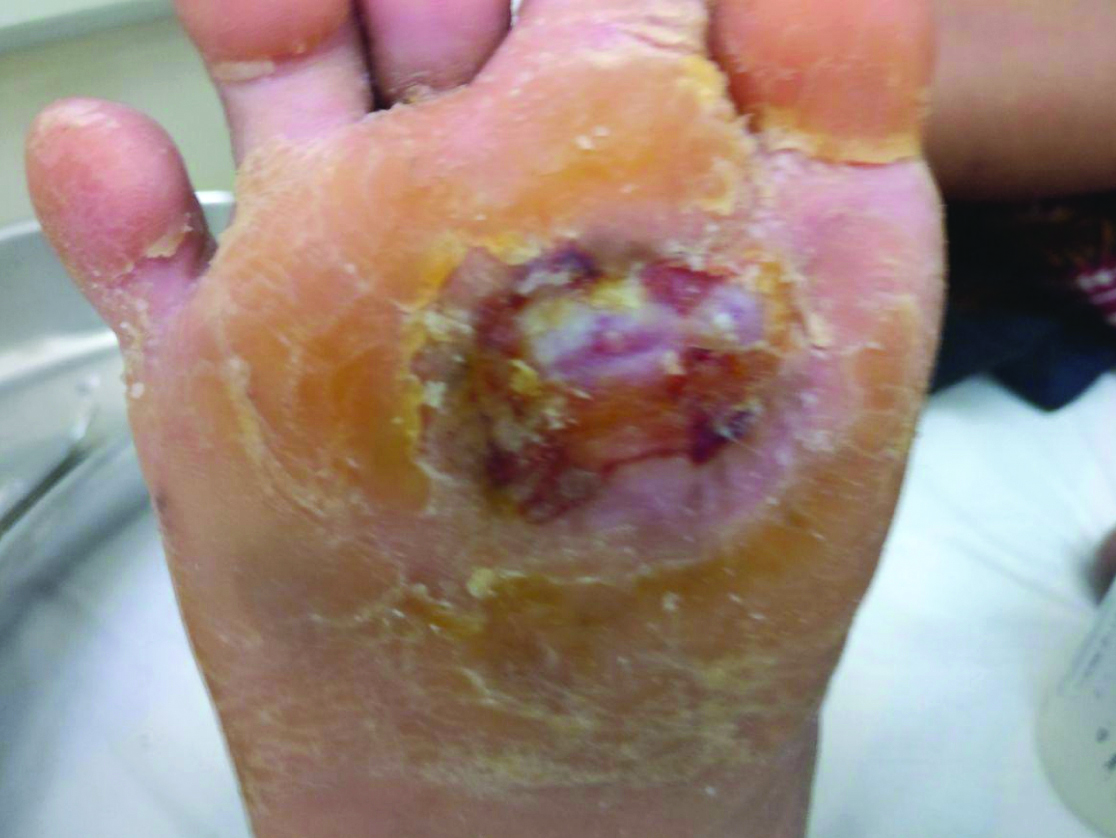
A 60-year-old female patients having a history of Hansen’s disease treated six years back, presented to Department of Dermatology of a tertiary care hospital with a non-healing ulcer of size 4×3 cm over the right sole since three years. Six years back she presented with white patches on the upper back with impaired sensation. Three years later she developed ulcer on the right sole which was increasing in size and failed to respond to any antibiotics. There was no family history suggestive of Leprosy. She didn’t have any associated systemic illness like diabetes or hypertension. There was negative history of infections in the past. She had received multi bacillary multi-drug therapy consisting of Rifampicin 600 mg once a month, Dapsone 100 mg daily and Clofazamine 50 mg daily for the management of Hansen’s disease for one and a half years. On general physical examination, no abnormality was detected. On local examination, there was a single 4 cm×3 cm oval shaped punched out ulcer over the plantar surface of right foot over the metatarsal area [Table/Fig-1].
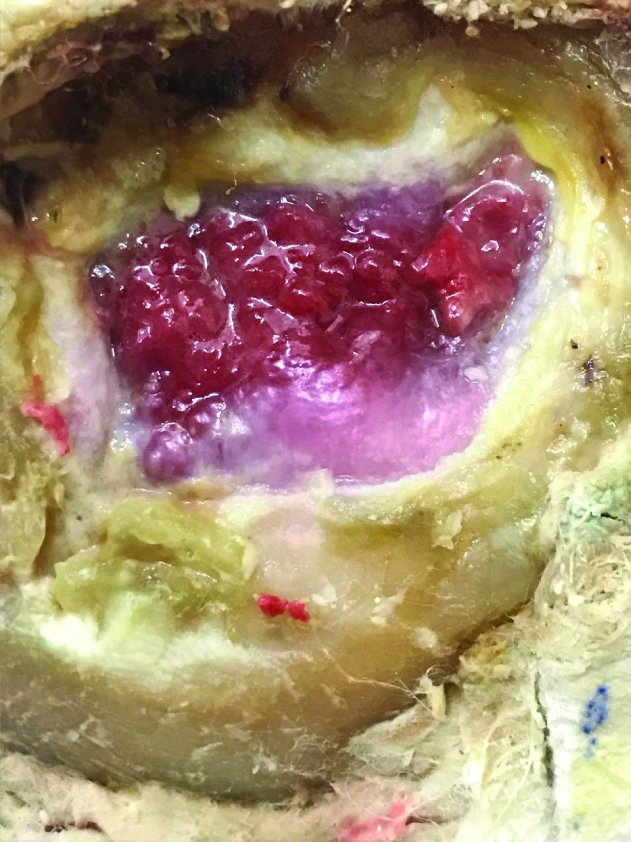
The floor was covered with red granulation tissue and mild slough was present without visible discharge from the ulcer and edges were hyperkeratotic. On palpation, there was no tenderness and no induration. The ulcer was not fixed to the underlying structures and it was one centimetre in depth, there was no bleeding on palpation. There was no lymphadenopathy. Bilateral ulnar and right posterior tibial nerves were palpable but non-tender. Peripheral nerve examination showed absence of sensation over the posterior tibial nerve distribution in the right foot. Based on the history and clinical examination, a provisional diagnosis of Hansen’s disease borderline tuberculoid with trophic ulcer on the right foot was made with a differential diagnosis of diabetic foot ulcer. The other differentials included were Syringomyelia, diabetic neuropathy, alcoholic polyneuropathy, arterial and venous ulcer and ulcer due to systemic cause mainly nutritional. The ulcer was of recent onset, hence syringomyelia was ruled out. Patient was neither diabetic nor alcoholic. Doppler study was normal hence arterial and venous causes were also ruled out. Hence, provisional diagnosis of trophic ulcer due to hansen’s disease was made. White Blood Cell (WBC) counts, haemoglobin and blood sugars were normal. Slit skin smear was done from four sites, one from ear lobe, one from supraorbital skin, one from dorsum of the hand and one from the patch and stained with Zeil Neilson stain and was negative for bacillus. She had received multiple antibiotic courses including Tab. Amoxycillin 625 mg twice daily for 10 days, Tab. Cefatoxime 200 mg twice daily for five days and Tab. Lincomycin 500 mg thrice a day for seven days. The patient was advised complete rest with Multi Cellular Rubber (MCR) footwear. The ulcer never showed any improvement to these standard treatment modalities. Hence complete rest was ensured with usage of plaster cast and she was undertaken for PRFM application.
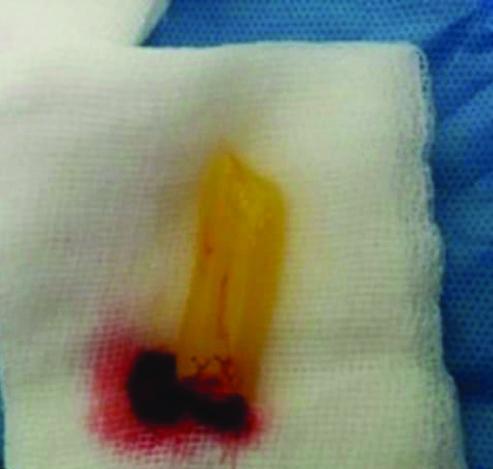
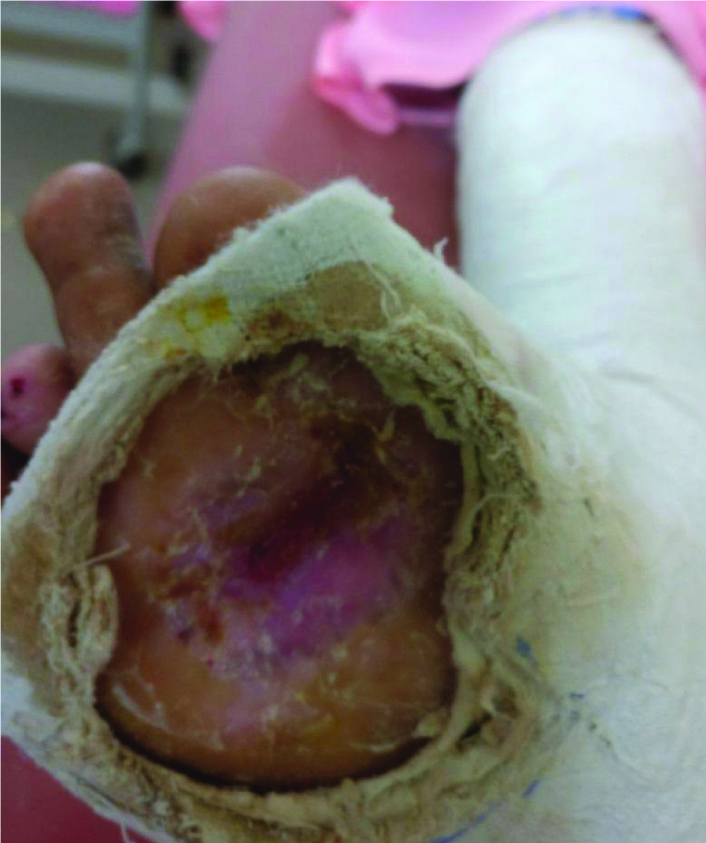
Ten millilitre of venous blood was drawn under aseptic precautions and it was added to a centrifuge tube without anticoagulant. Then it was centrifuged at 4000 rpm for 10 minutes. The fibrin layer which was obtained was transferred onto sterile gauze [Table/Fig-2] and the middle membrane was gently compressed between the two gauze pieces and applied on a healthy wound and a secondary non-absorbable dressing was applied on the top. Adequate rest was ensured after the procedure with POP cast and a window was created in the POP cast for wound dressing [Table/Fig-3]. Patient was called back after 10 days and the secondary dressing of the patient and the dried PRFM was removed from the wound bed. Procedure was repeated every third week. There was a dramatic improvement in the wound healing and wound closed completely in three sittings.
Fibrin matrix on the gauze piece.
Rest to the leg using POP cast and a window for dressing.
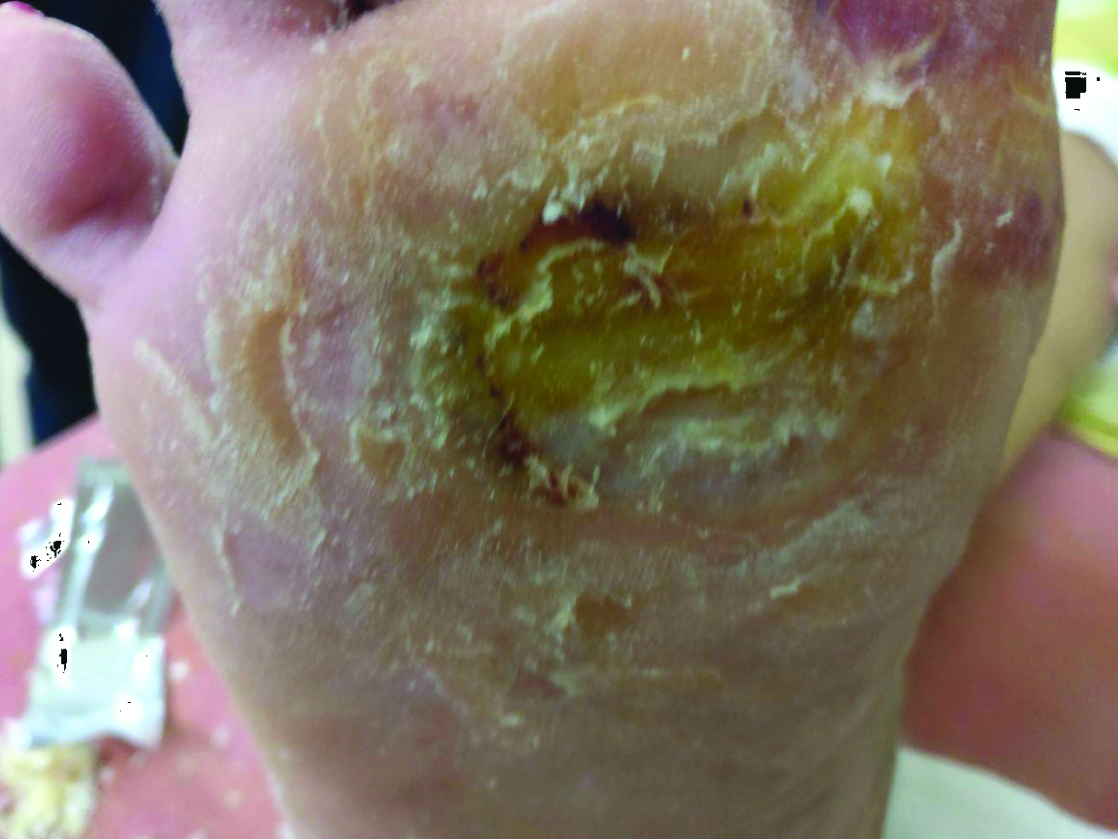
During first follow-up after three weeks there was reduction in the size of the ulcer up to 50% [Table/Fig-4]. During the second follow-up after six weeks, granulation tissue was covered with hyperkeratotic skin [Table/Fig-5]. Third follow-up at 9th week showed complete healing of the ulcer with only hyperkeratotic skin on it [Table/Fig-6].
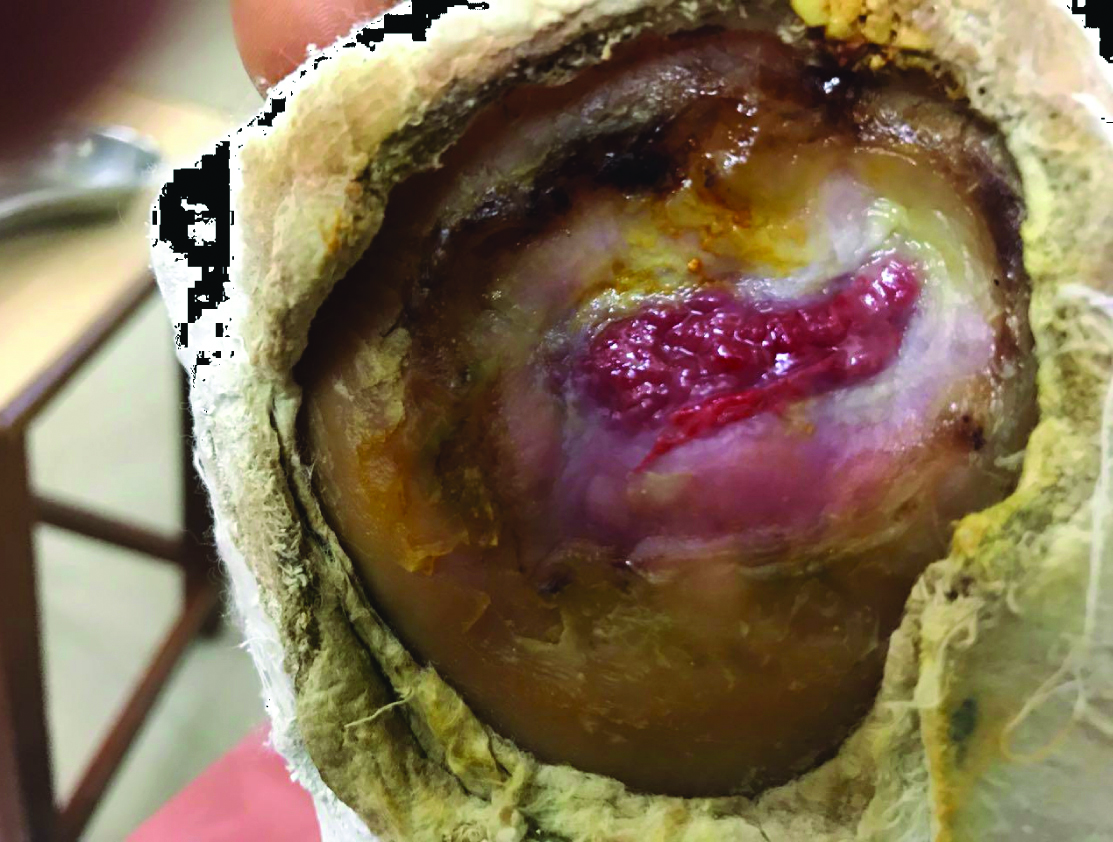
Discussion
Leprosy or Hansen’s disease is a mycobacterial infection caused by Mycobacterium Leprae and it is a major public health problem, currently affecting approximately a quarter million people worldwide, with 60% of these cases being reported from India [1]. The situation of leprosy has changed in the world significantly after the successful initiation of multi-drug therapy. The programme in India reduced the prevalence rate from 57.8/10,000 in 1983 to less than 1/10,000 by the year 2005 [2]. The disease manifests as hypopigmented patches with sensory loss and thickened nerve. Demonstration of acid fast bacilli is the key sign of leprosy. Trophic ulcer is the major complication of anaesthetic foot. This can lead to debility and deformity.
One of the major causes of debilitation in Hansen’s disease patients is chronic plantar ulcer occurring in about 10%-20% of these patients, resulting in considerable reduction in quality of life [4]. Whenever there is ulcer, the foot becomes ulcer prone and the vicious cycle continues. If it is associated with morbidity, it can lead to psychological problems and finally make the patient cripple.
Various systemic, cellular, vascular, and anatomical factors result in formation of non-healing ulcers those are refractory to normal healing processes and standard care. Some mechanism involved in the development of trophic ulcers are continuous pressure, concentrated pressure by mechanical violence, heat or cold causing burning or frostbite, repetitive mechanical stress, pressure on the infected tissue [5]. The differential diagnosis for trophic ulcers includes neurogenic like Hansen’s disease, syringomyelia, diabetic neuropathy, alcoholic polyneuropathy, arterial ulcer, venous ulcer, ulcer due to systemic causes mainly nutritional. As the hypopigmented patches on the back showed impaired sensation and skin biopsy showed features suggestive of Hansen’s disease, the cause of trophic ulcer in the present patient was considered to be Hansen’s disease. These ulcers not only lead to decreased quality of life and productivity in the patient but also increase the financial burden on the patient due to long term management [7]. The goal of management of ulcer treatment is to obtain wound closure as rapidly as possible. Conventional treatment for ulcers includes wound cleansing, tissue debridement, prevention and treatment of infection, immobilisation and local ulcer care with dressings [7,8]. However, non-healing ulcers remain unresponsive to the initial treatment and persist in spite of adequate local care.
The growth and emergence of innovative procedures like PRFM therapy have greatly revolutionised the treatment of this not uncommon but highly frustrating problem of non-healing plantar ulceration. They belong to a new generation of platelet concentrates, extracted from whole blood of the patient by centrifugation at 3000 rpm [9]. Platelets at the site of wound, releases various signalling growth factors like Platelet-Derived-Growth-Factor (PDGF), Vascular-Endothelial-Growth-Factor (VEGF), Transforming-Growth-Factor-β (TGF-β) and Fibroblast-Growth-Factor (FGF) and cytokines that help in accelerating wound healing by stimulating various components of healing process including regulation of inflammation, chemotaxis, angiogenesis, cell proliferation, synthesis and remodelling of new tissue [9-11]. It is also shown that platelets also exert antimicrobial activity thus reducing infection in wounds [12]. PRFM as a procedure was first developed by Choukroun J et al., in France for use in oral and maxillofacial surgery [13]. Nagaraju U et al., in their study said eight out of nine ulcers needed more than one application of PRFM with a mean number of three applications and ulcers closed by five sittings [9]. Sarvajnamurthy S et al., found mean duration of the healing of the chronic venous ulcers using PRP was 5.1 weeks [14].
Since then, PRFM has emerged as a safe, simple, cost-effective and feasible treatment modality with good clinical results in various fields of medicine (periodontics, eye surgeries, orthopaedics, plastic surgeries) [15,16]. However, its use in routine clinical practise is very scarce, especially in Southern India because of decreased awareness of this novel treatment modality. This case report thus substantiates the use of PRFM in non-healing plantar ulcers in patients of Hansen’s disease that are unresponsive to standard treatment procedures. The advantage of PRFM over PRP is that when incorporated into fibrin, the concentration of growth factors in the platelet concentration is three fold more. And also, these growth factors are released in a controlled manner over approximately one week [17].
Conclusion
Autologous platelet-rich fibrin matrix for the treatment of hard-to-heal chronic plantar ulcer in Hansen’s disease is a feasible, safe, simple and inexpensive method with no complications. Further prospective studies are now needed to substantiate its use in regular clinical practice.
[1]. WHO Expert Committee on Leprosy elimination, Geneva, World Health. Organization, 2017 [Google Scholar]
[2]. Rao PN, Suneetha S, Current situation of Leprosy in India and its future implicationsIndian Dermatol Online J 2018 9(2):83-89.10.4103/idoj.IDOJ_282_1729644191 [Google Scholar] [CrossRef] [PubMed]
[3]. Murthy PK, Clinical manifestations, diagnosis and classification of LeprosyJ Indian Med Assoc 2004 102(12):678-79. [Google Scholar]
[4]. Srinivasan H, Dharmendra , Deformities in leprosy (general consideration)Leprosy in India. Mumbai, India 1978 1:197-204. [Google Scholar]
[5]. Riaz N, Sehgal VN, Leprosy: Trophic skin ulcersSkinmed 2017 15(1):45-51. [Google Scholar]
[6]. Puri V, Venkateshwaran N, Khare N, Trophic ulcers-Practical management guidelinesIndian J Plast Surg 2012 45(2):340-51.10.4103/0970-0358.10131723162234 [Google Scholar] [CrossRef] [PubMed]
[7]. Suthar M, Gupta S, Bukhari S, Ponemone V, Treatment of chronic non-healing ulcers using autologous platelet rich plasma: a case seriesJ Biomed Sci 2017 24:16doi:10.1186/s12929-017-0324-110.1186/s12929-017-0324-128241824 [Google Scholar] [CrossRef] [PubMed]
[8]. Greer N, Foman NA, MacDonald R, Dorrian J, Fitzgerald P, Rutks I, Advanced wound care therapies for nonhealing diabetic, venous, and arterial ulcers: a systematic reviewAnn Intern Med 2013 159(8):532-42.10.7326/0003-4819-159-8-201310150-0000624126647 [Google Scholar] [CrossRef] [PubMed]
[9]. Nagaraju U, Sundar PK, Agarwal P, Raju BP, Kumar M, Autologous platelet-rich fibrin matrix in non-healing trophic ulcers in patients with Hansen’s diseaseJ Cutan Aesthet Surg 2017 10:03-07.10.4103/JCAS.JCAS_17_1628529413 [Google Scholar] [CrossRef] [PubMed]
[10]. O’Connell SM, Hessler K, Dardik H, Cascade ® autologous system platelet-rich fibrin matrix in the treatment of chronic leg ulcersAdv Wound Care (New Rochelle) 2012 1:52-55.10.1089/wound.2011.029024527280 [Google Scholar] [CrossRef] [PubMed]
[11]. Steenvoorde P, van Doorn LP, Naves C, Oskam J, Use of autologous platelet-rich fibrin on hard-to-heal woundsJ Wound Care 2008 17:60-63.10.12968/jowc.2008.17.2.2817918389830 [Google Scholar] [CrossRef] [PubMed]
[12]. Lacci KM, Dardik A, Platelet-rich plasma: support for its use in wound healingThe Yale J Biol Med 2010 83(1):01-09. [Google Scholar]
[13]. Choukroun J, Adda F, Schoeffler C, Vervelle A, An opportunity in perio-implantology (in French): The PRFImplantodontie 2001 42:55-62. [Google Scholar]
[14]. Sarvajnamurthy S, Suryanarayan S, Budamakuntala L, Suresh DH, Autologous platelet rich plasma in chronic venous ulcers: Study of 17 casesJ Cutan Aesthet Surg 2013 6:97-99.10.4103/0974-2077.11267124023432 [Google Scholar] [CrossRef] [PubMed]
[15]. Agrawal AA, Evolution, current status and advances in application of platelet concentrate in periodontics and implantologyWorld J Clin Cases 2017 5(5):159-71.10.12998/wjcc.v5.i5.15928560233 [Google Scholar] [CrossRef] [PubMed]
[16]. Sclafani AP, Safety, efficacy, and utility of platelet-rich fibrin matrix in facial plastic surgeryArch F Surg 2011 13(4):247-51.10.1001/archfacial.2011.321339469 [Google Scholar] [CrossRef] [PubMed]
[17]. Yazawa M, Ogata H, Nakajima T, Mori T, Watanabe N, Handa M, Basic studies on the clinical applications of platelet-rich plasmaCell Transplant 2003 12(5):509-18.10.3727/00000000310874707312953925 [Google Scholar] [CrossRef] [PubMed]