Fistula-in-ano is a granulomatous track connecting the anal canal to the perianal skin, usually the result of an anorectal abscess which has spontaneously burst or is inadequately drained [1]. Approximately 25-50% of patients with perianal abscesses may develop an anal fistula. The fistula connects an internal opening in the anal canal to an external opening in the perineum.
The search has always been on for the ideal method to surgically treat fistula-in-ano while preventing recurrence and incontinence. The common method of fistulectomy or fistulotomy is effective in treating the problem however it usually involves a large wound which takes a long time to heal and causes more morbidity. A variable part of the sphincter may be damaged depending on the level of the tract which may or may not lead to incontinence [1].
Rojanasakul A et al., developed the technique of LIFT as a method for treatment of fistula-in-ano through an intersphincteric approach [2]. The procedure is based on the principle that removal of the intersphincteric part of the tract removes the cryptoglandular tissue and thus the source of infection. Ligating the tract at the internal opening effectively closes the communication. As it avoids injury to the sphincter and the wound is smaller the morbidity is less [2]. Studies comparing LIFT and fistulotomy have shown that LIFT may be used effectively for anal fistula, however, the anal fistulae in those studies were not exclusively trans-sphincteric [3,4]. This study was planned with the aim to assess if indeed LIFT offers any advantage over standard fistulectomy or fistulotomy when treating patients with trans-sphincteric fistula-in-ano.
Materials and Methods
The prospective comparative cohort study was carried out from July 2011 to June 2015 at Lokmanya Tilak Municipal Medical College, Mumbai, Maharashtra, India, after approval by the Institutional Ethics Committee {File PS/IEC-HR/DISS/68/(11/10)}. All procedures performed in studies involving human participants were in accordance with the Ethical Standards of the Institutional and/or National Research Committee and with the 1964 Helsinki declaration and its later amendments or comparable Ethical Standards.
Patients having a documented diagnosis of a trans-sphincteric fistula tract determined to be of cryptoglandular origin (primary or recurrent), above 18 years of age and able to understand and provide informed consent were included in the study. Patients with a history or suspicion of Inflammatory Bowel Disease (Crohn’s or Ulcerative colitis), any fistula-in-ano of specific aetiology like tuberculosis, actinomycosis, nocardiasis and those associated with malignancy or a history of connective tissue disease were excluded. Sixty patients (51 males and 9 females) presenting with trans-sphincteric fistula were divided into two groups by simple randomisation and operated either by LIFT procedure or fistulotomy/fistulectomy. Informed consent was obtained from all individual participants included in the study.
Detailed history (including demographic details, presenting complaints, duration of symptoms, history of previous episodes of anorectal sepsis and past surgeries, history of any co-morbidity) was noted. Clinical findings recorded were the site and number of external opening, location of internal opening, evidence of abscess and the presence of other anal canal conditions like haemorrhoids or fissure. Findings of preoperative imaging studies such as fistulogram (conventional or MRI) were observed.
Thirty patients were treated by LIFT technique and 30 by standard fistulectomy or fistulotomy. The procedure was done under spinal anaesthesia in lithotomy position. The track was identified by probing with a fistula probe or by instilling dilute solution of methylene blue through the external opening.
All LIFT procedures were performed by the same surgeon. A curvilinear incision was taken at the intersphincteric groove over the fistula tract. The intersphincteric part of the tract was identified by careful blunt and sharp dissection. This intersphincteric part was then hooked using a small right-angled clamp. The tract was ligated close to the internal sphincter with polyglactin no. 2-0 and cut distal to ligature. The intersphincteric part of the tract was excised along with other intersphincteric tissue and sent for histopathological examination. The distal fistulous tract was then cored out or curetted from the external opening to the external sphincter. The external sphincter defect, if any, was repaired. The intersphincteric incision, as well as the distal tract, was kept open to facilitate drainage and prevent infection. Wound was irrigated using antiseptics such as hydrogen peroxide and povidone iodine. Antiseptic pack was kept and dressing given.
Fistulectomy or fistulotomy procedures were performed by different surgeons. In general, the fistula tract was laid open. Either the granulation was scraped and scooped or the tract was partially or completely excised using electrocautery leaving behind healthy perirectal fat as per surgeon’s preference. Injury to external sphincter was avoided. Haemostasis was achieved. Wound was irrigated with antiseptics such as hydrogen peroxide and povidone iodine. Antiseptic pack was kept and dressing was given. Operative time and blood loss were noted.
All patients received prophylactic perioperative antibacterial medications including a ‘Fluoroquinolone’ and ‘Metronidazole’. They were also prescribed warm Seitz baths to irrigate the wound. Severity of postoperative pain was assessed using Visual Analogue Scale on the evening of surgery before administering any analgesic. Patients were discharged once pain and discomfort significantly reduced and when they were confident of managing wound at home. The duration of hospital stay was noted. After discharge patients were advised to take analgesics daily till the pain subsided significantly. Duration of use of analgesics was noted. Evaluation was done weekly till complete wound healing and time to complete wound healing was noted. Any complaint of incontinence for flatus or stools was recorded. After wound healing, patients were followed up monthly for recurrence till 12 months postoperatively.
Complete wound healing was defined as full epithelialisation of the wound [2]. Recurrence was defined as either non-healing of the wound after 12 weeks or a reappearance of symptoms at the same site.
Statistical Analysis
Statistical analysis was done by Unpaired t-test for continuous data and chi-square test for categorical data using SAS® software. A p-value of <0.05 was considered significant.
Results
Sixty patients underwent surgery for fistula-in-ano. There were 51 men and 9 women. Age ranged from 19 to 65 years (Median 35 years). Fifty-three presented with perianal discharge, 43 complained of swelling and 29 had local pain. The duration of symptoms ranged from one month to five years (Median seven months). Twenty patients reported prior surgery for perianal abscess. In all, 11 patients had recurrent fistulae. All patients had single external opening with mean distance of 4.91 cm (SD = 1.43) from the anal verge. The diagnosis of trans-sphincteric fistula in all 60 patients was mainly clinical and imaging in the form of conventional fistulography and Magnetic Resonance (MR) fistulography was only done in certain patients to confirm the type of fistula. In all patients, histopathology showed non-specific chronic inflammation as patients with specific aetiology were excluded.
LIFT procedure and fistulectomy/fistulotomy were performed on 30 patients each. The two groups were comparable in the demography and anatomy of the fistulae as shown in [Table/Fig-1].
Clinical profile of patients with trans-sphincteric fistula.
| Variables | | LIFT | Fistulectomy or fistulotomy | p-value (Pearson chi-Square test) |
|---|
| Number | | 30 | 30 | |
| Age (years) | (Mean±SD) | 34.23±9.15 | 38.8±11.31 | 0.123* |
| Gender | Male n (%) | 26 (86) | 25 (83) | 0.718 |
| Female | 4 (14) | 5 (17) |
| Pain | n (%) | 18 (60) | 11 (37) | 0.071 |
| Swelling | n (%) | 24 (80) | 19 (63) | 0.152 |
| Discharge | n (%) | 26 (87) | 27 (90) | 0.688 |
| Duration of symptoms (months) | (Median) | 8.00 | 6.50 | 0.704* |
| Previous abscess | | 12 | 8 | 0.273 |
| Previous surgery | | 4 | 7 | 0.317 |
| External opening | Anterior | 10 | 7 | 0.390 |
| Posterior | 20 | 23 | |
| Internal opening | Anterior | 12 | 9 | 0.416 |
| Posterior | 18 | 21 | |
| Distance from verge (cm) | | 4.96±1.71 | 4.85±1.07 | 0.770* |
*Unpaired t-test was used to calculate p-value
Comparison of results of the two surgical procedures are shown in [Table/Fig-2]. The patients operated by LIFT procedure had less postoperative pain and shorter hospital stay. This was most likely due to a smaller wound which led to less morbidity. [Table/Fig-3] shows the postoperative wound of a LIFT procedure with external opening 4 cm away from the anal verge. [Table/Fig-4] shows the large wound after a fistulectomy.
| Variables | LIFT | Fistulectomy or fistulotomy | p-value |
|---|
| Operating time (min) | 32.50±7.52 | 40.17±9.78 | 0.001* |
| Hospital stay (Days) | 1.64±0.79 | 2.53±0.97 | 0.003† |
| Postoperative pain on day 1 (VAS) | 4.41±1.53 | 5.67±1.45 | 0.002† |
| Need for analgesics (Days) | 2.86±3.80 | 4.57±4.34 | 0.110† |
| Patients with complete healing by 12 weeks (n) | 26 | 27 | 0.687‡ |
| Time to complete healing (Weeks) | 5.64±1.91 | 6.89±1.65 | 0.023† |
| Recurrence (n) | 5 | 3 | 0.448‡ |
| Incontinence (n) | 0 | 3 | 0.076‡ |
*Unpaired t-test; †Mann-Whitney test; ‡Pearson chi-square test
Postoperative wound after LIFT procedure with external opening 4 cm from anal verge.
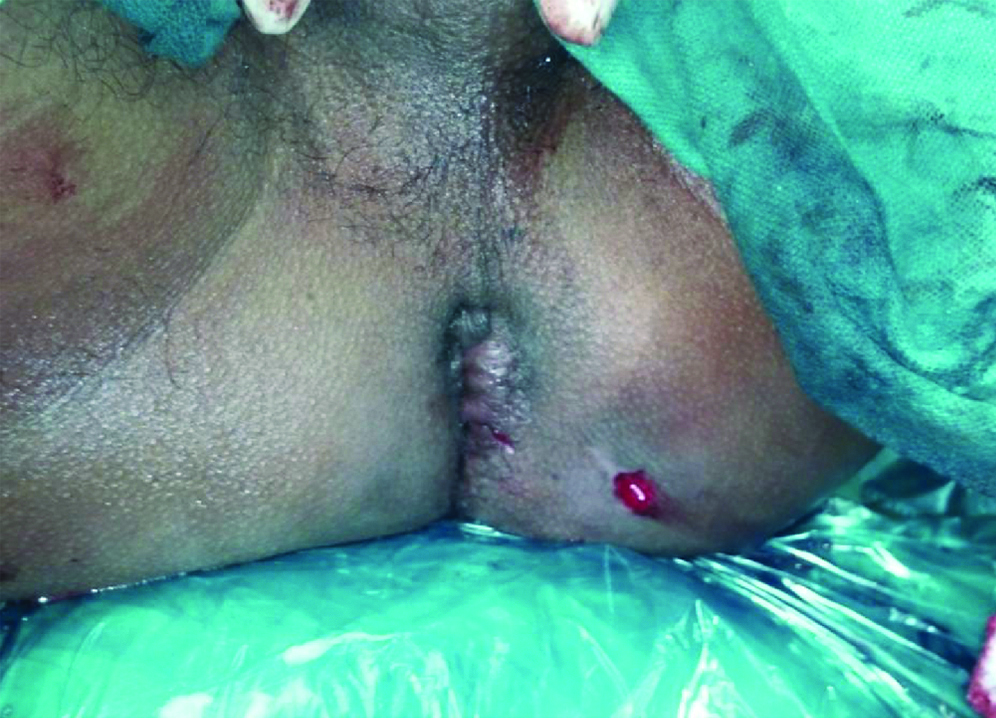
Wound after fistulectomy.
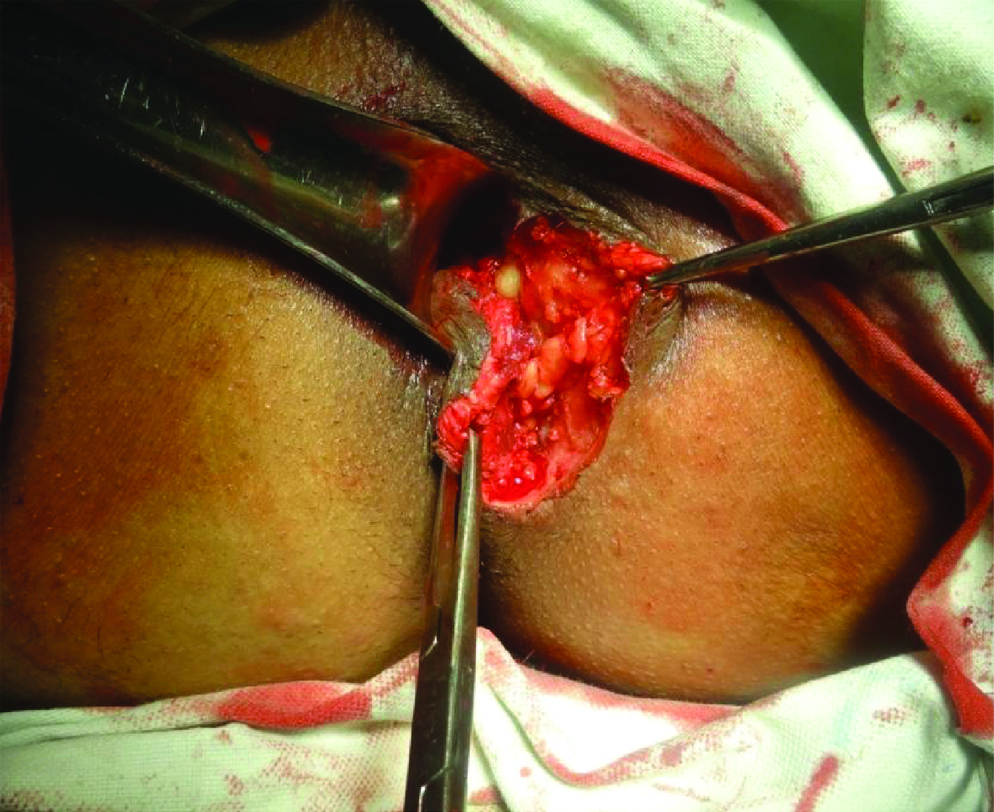
Patients were followed up for a median of 12 months (range 3 to 18 months). 5 of 30 patients (16.6%) who had LIFT performed came back with a recurrence. Median time for recurrence was 2.5 months i.e., 10 weeks. The earliest recurrence was at six weeks.
Of the 30 patients who underwent fistulectomy/fistulotomy, 3 (10%) had a recurrence within in a median follow-up time of eight weeks.
All recurrences were reported within three months of initial surgery. They were treated surgically with fistulectomy and advancement flap as required.
No patient operated by LIFT had any incontinence while three patients of fistulectomy had temporary incontinence for flatus and liquid stools for a short duration (<3 weeks) postoperatively. No patient in any group had permanent incontinence.
Discussion
The study shows that LIFT has a shorter operative time, less postoperative pain, shorter hospital stay and faster healing time than fistulectomy or fistulotomy. Though there was a higher recurrence in LIFT it was not statistically significant.
The shorter operative time for LIFT procedure is probably due to smaller incisions and precise surgical steps. Rojanasakul A et al., recorded a mean operating time of 40 minutes and an average postoperative stay of 1.25 days for patients undergoing LIFT procedure in 2007 [2]. In 2012, Ooi K et al., reported a median operating time of 39 minutes for LIFT [5].
Decreased postoperative pain noted after LIFT procedure as compared to fistulectomy or fistulotomy, would mean a decreased need for pain medication and therefore their adverse effects, and more patient comfort.
A smaller wound in the LIFT procedure leads to faster healing and lesser morbidity. Rojanasakul A et al., reported a success rate of 94.4% initially with a mean healing time of four weeks and recurrence in 5.6% without any significant impairment of continence [2]. However, no other study has duplicated these results. In 2010, Shanwani A et al., reported a success rate of 82.2% for LIFT with a median time of healing as six weeks and a failure rate of 17.8% with recurrence occurring between 3-8 months [6]. Bleier A et al., reported a recurrence rate of 43% with 10 weeks as the median time to failure [7]. Other studies showed rates of healing varying from 57% to 68% [5,7]. A long-term study has shown a primary healing rate of 87.6% after a median follow-up of 71 months [8].
Malouf AJ et al., reported a recurrence rate of 4% in patients treated by fistulotomy and fistulectomy [9]. A recurrence rate of 8% was recorded by Garcia-Aguilar J et al., in 375 patients treated by fistulotomy, seton placement and advancement flap [10]. Factors associated with recurrence have been identified in various studies as complex type of fistula, horseshoe extension, lack of identification or lateral location of the internal fistulous opening and previous fistula surgery [10].
Though LIFT seemingly has higher recurrence rate compared to fistulotomy or fistulectomy it does not bar any further procedures to treat the fistula. As Bleier JI and Moloo H, put it ‘An important point regarding the use of LIFT is the fact that it appears to burn no bridges’; even if it does not work, other approaches can still be utilised [11].
LIFT shows low incidence of incontinence in all studies conducted so far thus emphasising the sphincter saving nature of this procedure. A study by Alapach S et al., showed incontinence of 16.2% for fistulotomy which was significant compared to 2.1% incidence in the LIFT group [3].
Studies comparing LIFT to fistulotomy have shown LIFT to be an effective and safe procedure with low incidence of incontinence and faster healing time. However, intersphincteric fistulae were also included in the study groups [3,4].
Although basic principle of LIFT technique has been observed, the procedure practised in not exactly as per the original description. The intersphincteric incision was kept open instead of primary closure due to high incidence of breakdown in primarily closed perianal wounds. Yet complete healing was observed. At times, friable fistula tract disrupted during dissection prior to ligation, making identification of the tract difficult due to retraction of the ends. In such cases, tissue in the intersphincteric region representing cryptoglandular tissue was scooped or excised along with the scooping of the distal tract. In patients with very well formed tract, it could be easily cored out instead of curetting. Such wounds also healed well. Modified LIFT procedures have been termed LIFT plus and have been reported to result in similar healing rates [12,13].
Limitation
This study had a relatively small sample size. Also, fistulectomy or fistulotomy was performed by different surgeons so techniques may have a slight variations. A further study with a larger sample size can validate the findings of this study.
Conclusion
In conclusion, despite slightly higher recurrence rate, Ligation of Intersphincteric Fistula Tract procedure has certain advantages over standard fistulotomy or fistulectomy in treatment of trans-sphincteric anal fistulae. The advantages include shorter operative time, less postoperative pain, shorter hospital stay and faster wound healing which is expected to translate to early resumption of normal activities. Even if recurrence occurs it results in an intersphincteric or trans-sphincteric fistula and other treatment modalities can still be used at a later date.
*Unpaired t-test was used to calculate p-value
*Unpaired t-test; †Mann-Whitney test; ‡Pearson chi-square test