Mucosal Tears Following Biopsy in Eosinophilic Oesophagitis
William G Simpson1
1 Department of Rural Health Gastroenterology, Oklahoma State University, College of Osteopathic Medicine, Tahlequah, Oklahoma, USA.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. William G Simpson, 205 Harris Circle, Suite 201, Tahlequah, Oklahoma, USA.
E-mail: wsimpson@nhsok.org
Dysphagia, Fibrosis, Gastrointestinal endoscopy
Dear Editor,
Previously thought to be a paediatric disease, eosinophilic oesophagitis is being diagnosed in adults with increasing frequency. These individuals frequently present with dysphagia to solids and food bolus impaction is common. Two patients were evaluated endoscopically for dysphagia. A 66-year-old male had Los Angeles grade A ulcerative oesophagitis as well as numerous concentric rings throughout the oesophagus, longitudinal furrows and distinct strictures in the mid- and distal oesophagus. Biopsy of the mucosa using large capacity forceps (jumbo) (Boston Scientific Radial Jaw 4, 2.8 mm cup) was met with tenting of the mucosa requiring noticeably increased force to obtain the specimen resulting in zipper-like mucosal tears [Table/Fig-1]. A second patient, a 34-year-old male, demonstrated no gross reflux oesophagitis but diffuse concentric rings, longitudinal furrowing and a distal stricture [Table/Fig-2]. Biopsies from the body of the oesophagus with jumbo forceps resulted in similar mucosal tears after force was required to obtain the specimen. In both instances, the mucosa appeared to peel away from the underlying tissue leaving an oblong to linear defect much larger than the size of the forceps cups. Balloon dilation of the strictures did not result in mucosal tearing. Histopathologic examination of both sets of biopsies confirmed Eosinophilic Oesophagitis (EoE) demonstrating chronic oesophagitis with a marked infiltration of the mucosa with eosinophils (>30 per high power field) and eosinophilic microabscesses [Table/Fig-3] [1]. Neither patient was symptomatic in the recovery area. There was no clinical evidence of transmural perforation. These individuals reflect the mucosal fragility commonly seen in patients with EoE [1,2]. Dilation of strictures often produces distinct mucosal tears and can result in transmural perforation.
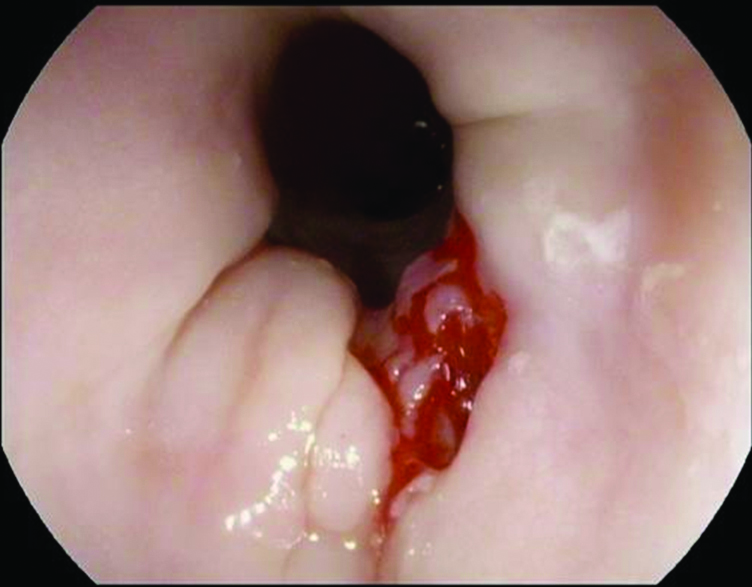
Linear oesophageal mucosal tear following biopsy with large capacity (jumbo) forceps.
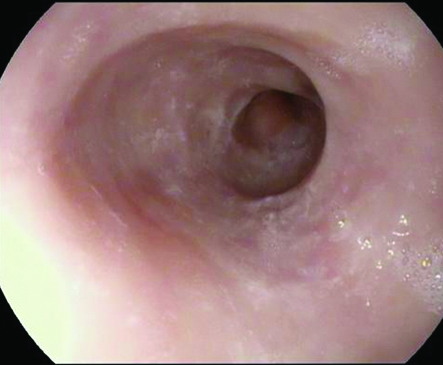
Endoscopic view of the mid- and distal oesophagus of the second patient revealing concentric mucosal rings, linear furrows, and a distal stricture.
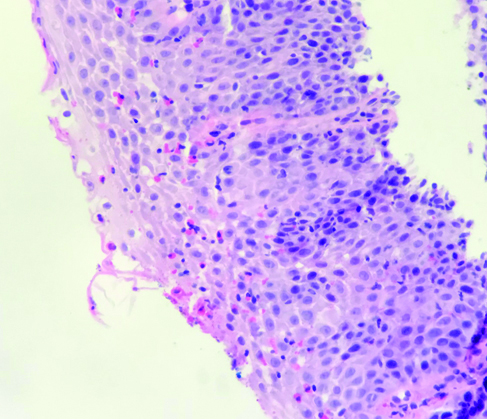
Photomicrograph of biopsy (from the first patient) obtained with jumbo forceps demonstrating chronic oesophagitis with >30 eosinophils per high power field (H&E, original magnification 40X).
Such fragility has not previously been reported with mucosal biopsy employing jumbo forceps but suggest caution is warranted. The force required to obtain the biopsies, when contrasted with patients without EoE, further support the growing perception of EoE as a chronic inflammatory disorder resulting in progressive fibrosis [3]. The biopsy of patients with suspected EoE should be approached with care similar to that afforded dilation.
[1]. Dellon ES, Gonsalves N, Hiran I, Furuta GT, Liacouras CA, Katzka DA, ACG Guideline: Evidence based approach to the diagnosis and management of esophageal eosinophilia and eosinophilic esophagitis (EoE)Am. J. Gastroenterol 2013 108:679-92.10.1038/ajg.2013.7123567357 [Google Scholar] [CrossRef] [PubMed]
[2]. Cohen MS, Kaufman AB, Palazzo JP, Nevin D, Dimarino AJ Jr, Cohen S, An audit of endoscopic complications in adult eosinophilic esophagitisClin Gastroenterol Hepatol 2007 5(10):1149-53.10.1016/j.cgh.2007.05.01717683993 [Google Scholar] [CrossRef] [PubMed]
[3]. Koutlas NT, Dellon ES, Progression from and inflammatory to a fibrostenotic phenotype in eosinophilic esophagitisCase Rep Gastroenterol 2017 11(2):382-88.10.1159/00047739129033756 [Google Scholar] [CrossRef] [PubMed]