Histomorphological Study of the Endometrium in Response to Insulin Resistance Induced by High Energy Diets in Swiss Albino Mice
Gnanagurudasan Ekambaram1, Senthil Kumar Sampath Kumar2
1 PhD Research Scholar, Department of Anatomy, Sri Ramachandra Medical College and Research Institute, Chennai, Tamil Nadu, India.
2 Professor, Department of Anatomy, Sri Ramachandra Medical College and Research Institute, Chennai, Tamil Nadu, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Senthil Kumar Sampath Kumar, Professor, Department of Anatomy, Sri Ramachandra Medical College and Research Institute, Porur, Chennai, Tamil Nadu, India.
E-mail: ssksrmc@gmail.com
Introduction
The morphology of endometrium is continuously influenced by hormones in each menstrual cycle. In addition to this, metabolic syndrome such as obesity and insulin resistance affects the morphology of endometrium through elevated estrogen and insulin levels.
Aim
To study the histomorphological effects in the endometrium due to insulin resistance through high energy diets in swiss albino mice.
Materials and Methods
Thirty six swiss albino mice were randomly divided into control, high fat diet and high fructose diet groups with 12 animals in each group. The animals were fed respective diets and the study was carried out for 12 weeks. After the study period the blood was collected from the animals in the retro orbital sinus under general anaesthesia and animals were sacrificed by the administration of ether. Serum was separated in centrifuge and stored at -20°C for the analysis of glucose and insulin levels. Uterus was removed and kept in neutral buffered formalin for tissue processing. Homeostasis Model Assessment of Insulin Resistance (HOMA–IR) was calculated to assess the insulin resistance.
Results
The glucose, insulin and HOMA–IR levels were higher in high fat and high fructose diet groups. There was complex atypical hyperplasia with glandular crowding in the endometrium of high fat diet and high fructose diet animals.
Conclusion
The present study concludes the positive role of metabolic syndromes such as insulin resistance in the development of preneoplastic lesions in the endometrium. If the condition persists for a long time it can progress into endometrial carcinoma.
Complex atypical hyperplasia, Endometrial carcinoma, Glandular proliferation, Metabolic syndrome, Obesity
Introduction
Endometrium of the uterus is a hormone dependent structure which undergoes cyclic changes throughout the reproductive period in women. Endometrium is a connective tissue layer with mucosa consisting of simple columnar epithelium, endometrial glands and stroma. In addition to this, endometrium possesses high affinity insulin receptors and thus factors which promote increase in the levels of insulin such as insulin resistance affect the endometrium and cause tissue damage. Insulin also increases the levels of insulin like peptides especially Insulin like Growth Factor-1 (IGF-1) which has actions similar to insulin in the endometrium of uterus [1,2]. Various epidemiological studies prove positive association of hyperinsulinemia and incidence of endometrial cancer. The increased incidence is seen in both pre and post-menopausal women who have type II diabetes mellitus which is due to insulin resistance [3-7]. The endometrial cancer is the most common gynaecological cancer in the developed countries which accounts for about two thirds of the global burden. The highest incidence is reported in North America with 20 per 100,000 women and in Europe it is between 11 and 14 per 100,000 women. The incidence is low in south Asian countries with less than 4 per 100,000 women [8]. In India the incidence is 4.3 per 100,000 women [9]. This could be construed in the light of westernization of lifestyle which promotes the intake of high energy diets rich in sugar and fats, sedentary lifestyle and prevalence of metabolic syndromes such as obesity.
There is a growing evidence to substantiate the fact that intake of high energy diets and sugar sweetened beverages which contain large amount of fructose as its main ingredient causes insulin resistance. Fructose is more lipogenic and causes obesity and insulin resistance than other forms of sugar. Because fructose bypasses a major rate controlling step in glycolysis and is converted into fatty acids in the liver at a faster rate [10]. The sugars in beverages are absorbed quickly and metabolized than the sugars in whole foods, because the fibre content in the whole foods slow down the metabolism of sugars [11]. The intake of sugar sweetened beverages is associated with higher incidence of type I endometrial cancer. This is due to the obesogenic tendency of sugar sweetened beverages and its potential to cause insulin resistance. Such hormonal imbalances due to dietary factors lead to higher incidence of early menarche and late menopause. All these contribute to the risk of developing endometrial cancer. Such dietary practice is prevalent in developed countries and explains why the incidence of endometrial cancer is high in these countries.
The trend in India is changing with rapid urbanization and change in the modes of diet among the urban class of people. Currently 300 million people live in cities in India and the mass migration to cities will be at an unprecedented rise in the next 20 years. The estimate predicts 300 million people to migrate to the cities for employment and livelihood according to the reports of XII Planning commission of India. Such migration would adversely affect the quality of urban lifestyle and the dietary practices in India. The intake of high fat diet and high intake of sugars in urban India are more likely to have higher BMI and incidence of diabetes mellitus, hypertension and other non- communicable diseases in India [12]. Thus, in the present study an attempt has been made to study the histomorphology of endometrium by simulating insulin resistance model through high energy diets in swiss albino mice.
Materials and Methods
A cross sectional study was done on female swiss albino mice weighing 15-25 gram in the age group of 21-30 days in Centre for Toxicology and Developmental Research and in Department of Anatomy, Sri Ramachandra University, Porur, Chennai. All the animals were properly housed in polypropylene cages (47×34×18cm) lined with sterile paddy husk renewed every 24 hours, with relative humidity (55%) in a 12 hour light/dark cycle at 25°±2°C. The animals were fed control diet, experimental diet with free access to water add libitum. The experiment was carried out in compliance with the guidelines of the Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA), New Delhi, India with the approval of Institutional Animal Ethics Committee (IAEC/XLVII/SRU/476/2016).
Experimental Groups
In the present study 36 female swiss albino mice were randomly divided into control group, high fat diet group and high fructose diet group with 12 animals in each group. All the animals were treated for the period of 12 weeks. In the control group normal pellet diet was fed with water ad libitum to the animals. In the high fat and high fructose diet group diets were formulated according to the American Institute of Nutrition (AIN – 93G) and modified for the present study to meet the recommended nutrient levels for mice [Table/Fig-1] [13]. The animals were fed experimental diets soon after the weaning period to ensure uniform consumption. The diets were prepared and fed to the animals freshly every day.
Composition of diets (g/100g).
| Ingredients | High fat diet | High fructose diet |
|---|
| Ingredients | Mayonnaise 60 | Fructose 60 |
| Casein (Fat free) | 20 | 20 |
| Methionine | 0.7 | 0.7 |
| Groundnut oil | 5 | 5 |
| Wheatbran | 10.6 | 10.6 |
| Salt mixture | 3.5 | 3.5 |
| Vitamin mixture | 0.2 | 0.2 |
Sample Collection
After the study period blood was collected from the retro orbital sinus under general anaesthesia and the animals were sacrificed by the administration of ether. The blood was centrifuged to get serum which was stored at -20°C for further analysis. The uterus was removed from the animals and washed thoroughly with tap water and fixed in neutral buffered formalin for histological tissue processing and observation. Basal insulin resistance parameters such as fasting glucose, insulin and Homeostasis Model Assessment of Insulin resistance (HOMA-IR) were analysed.
Statistical Analysis
Statistical analysis was performed by using Statistical Package for the Social Sciences (version 23.0), SPSS Inc, Chicago, Illinois, USA. Analysis was done through Kruskal wallis test, Post-Hoc test. Data are Mean±SD and the values are considered statistically significant when p-value is <0.05.
Results
The fasting glucose, insulin and HOMA–IR values were statistically highly significant between the groups in the present study [Table/Fig-2]. Comparative Post-Hoc analysis between control and other groups were shown in [Table/Fig-3].
Fasting glucose, Insulin and HOMA–IR values (Kruskal-wallis test).
| Groups | Glucose (mg/dL) | Insulin (mU/L) | HOMA-IR |
|---|
| Control | 116±12.11 | 1.49±0.09 | 0.42±0.05 |
| High fat diet | 223.17±15.54 | 3.84±0.43 | 2.13±0.38 |
| High fructose diet | 247.83±11.01 | 4.28±0.12 | 2.61±0.17 |
| Chi-square value | 22.276 | 22.354 | 22.444 |
| p-value | <0.001** | <0.001** | <0.001** |
Comparison of Fasting glucose, insulin and HOMA – IR between control and other groups (Post-Hoc test).
| Glucose (mg/dL) | Mean±SD | p-value |
|---|
| Normal control | 116.00±12.11 | 0.037* |
| High fat diet | 223.17±15.54 |
| Normal control | 116.00±12.11 | 0.001** |
| High fructose diet | 247.83±11.01 |
| Insulin (mU/L) | Mean±SD | p-value |
|---|
| Normal control | 1.49±0.09 | 0.066 |
| High fat diet group | 3.84±0.43 |
| Normal control | 1.49±0.09 | 0.001** |
| High fructose diet | 4.28±0.12 |
| HOMA-IR | Mean±SD | p-value |
|---|
| Normal control | 0.42±0.05 | 0.039* |
| High fat diet group | 2.13±0.38 |
| Normal control | 0.42±0.05 | 0.001** |
| High fructose diet group | 2.61±0.17 |
*p<0.05, **p<0.01
The tissues were processed and stained with Mason’s Trichrome (MT) for microscopic observation. Histological examination showed normal morphology of endometrium in the control group [Table/Fig-4]. Experimental group animals exhibited morphological changes such as papillae formation and glandular hyperplasia with crowding in high fat diet group [Table/Fig-5] and complex hyperplasia with cytological atypia and glandular proliferation in the high fructose diet group [Table/Fig-6].
Control group with normal appearance of endometrium (MT, 40X).
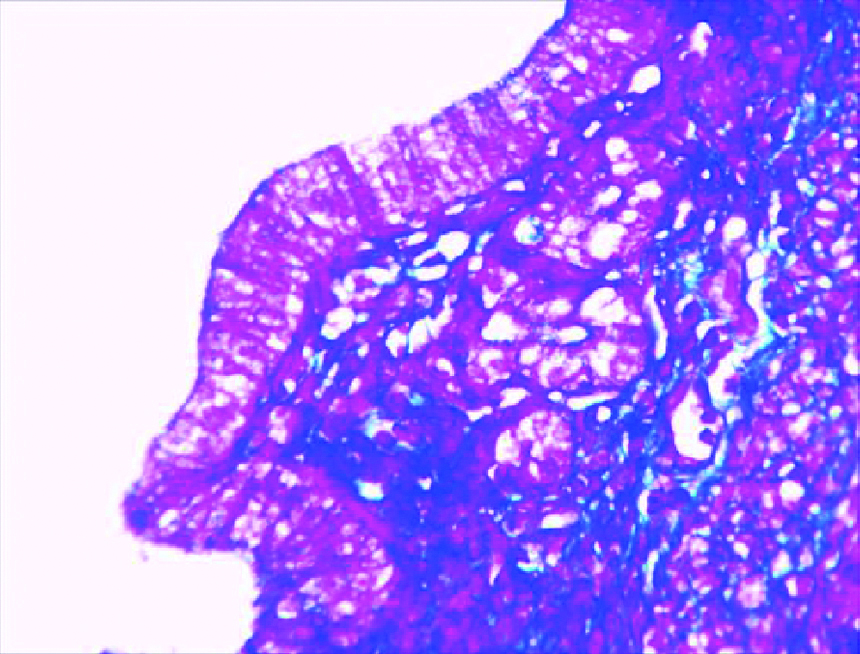
High fat diet group showing glandular hyperplasia and papillae formation in the endometrium. (MT, 40X)
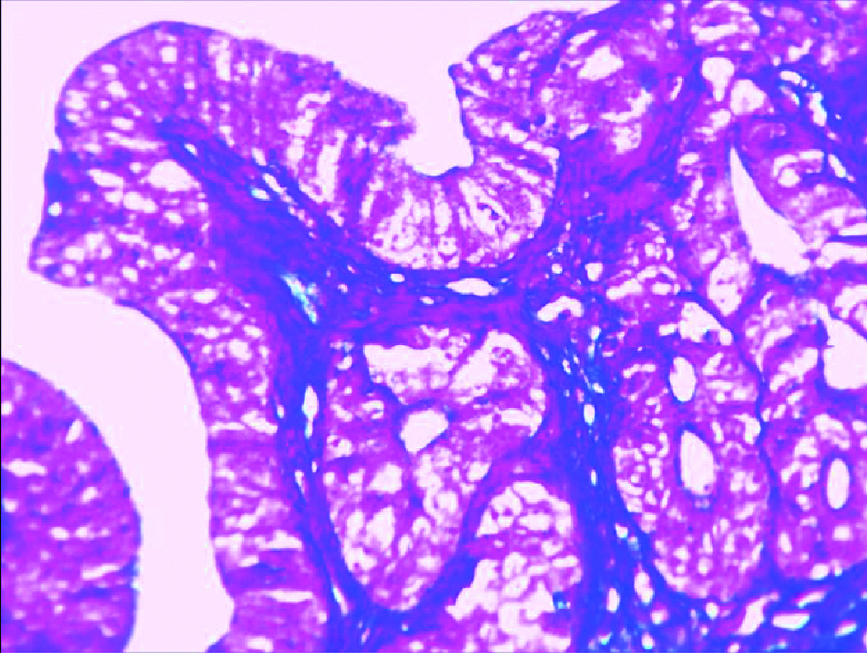
High fructose diet group showing complex hyperplasia with cytological atypia, glandular proliferation and crowding with focal stratification of epithelium. (MT 40X).
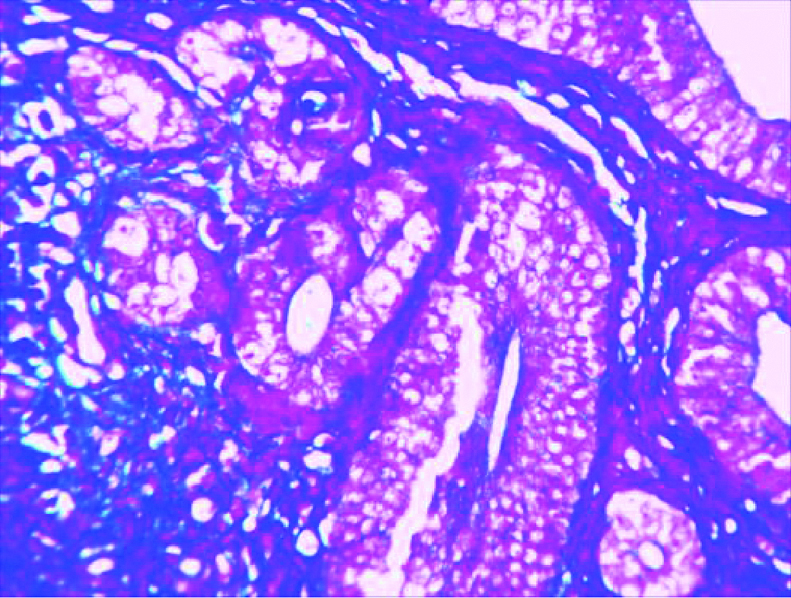
Discussion
Insulin resistance is a state in which there is a consistent increase of insulin in the circulation. This explains why diabetes is an independent risk factor for endometrial cancer with the risk of 2.0 [14]. In the present study there is a positive role of insulin resistance in the development of tissue damage in the endometrium through high energy diets. Insulin acts at two levels. In the endometrium increase in insulin reduces the level of Insulin like growth factor binding protein 1(IGFBP1) which consequently increases the action of IGF 1 and causes endometrial proliferation. In the ovary hyperinsulinemia due to insulin resistance causes ovarian hyperandrogenism which causes anovulation in which absence of progesterone increases the activity of oestrogen on the endometrium. This is especially seen in premenopausal women whereas in postmenopausal women excess adipose tissue deposit provides substrate for the peripheral conversion of oestrogens [15]. In addition to this, consumption of high energy diets leads to obesity which increases the levels of oestrogen and affects the endometrium. Diet contributes for 30% of cancers in western countries and second only to tobacco as a preventable cause of cancer. This has been known since 1970s in which people who consume diets rich in animal fat, sugar developed cancers of colorectum, breast, and prostate, endometrium in many western countries than the people in developing countries who consume diets rich in starch and have low intake of animal fat and sugar [16]. Among the dietary sugars fructose is found to be implicated in the development of insulin resistance than other forms of sugar [10,17]. In the earlier days fructose was considered to be an ideal sweetener due to its low glycaemic index and fructose does not stimulate insulin secretion and it is not under the regulatory control of insulin [18]. High intake of fructose leads to deposition of large amount of visceral adipose tissue than glucose which promotes deposition of subcutaneous adipose tissue [19]. Experimental administration of high doses of fructose directly into the brain through intracerebroventricular route leads to high consumption of food which could predispose to insulin resistance and obesity that can cause pathological changes in the endometrium [20]. The reason for the tissue damage in endometrium due to insulin resistance is that endometrial cancer cell lines have high affinity for insulin receptors [21]. Insulin with its mitogenic and antiapoptotic potential adversely affects the endometrium. The consequent increase of IGF-1 in insulin resistance is another major factor in the progression of neoplastic changes in the endometrium because IGF-1 is more mitogenic than insulin [22].
Among the surrogate markers to assess insulin resistance, in the present study the most popular HOMA-IR was used. HOMA-IR is a reliable method and can be used as a surrogate marker for insulin resistance in experimental research in rodents. It is a mathematical method derived from the product of glucose and insulin and divided by a constant [23]. HOMA-IR value above or equal to 2 has high diagnostic value in insulin resistance [24]. In the present study high fat and high fructose group animals exhibited HOMA–IR of >2 which shows successful simulation of insulin resistance in the experimental group.
Atypical hyperplasia of endometrium can progress into adenocarcinoma and if atypical hyperplasia a precursor lesion is associated with adenocarcinoma it is oestrogen induced [25]. In the present study similar atypical hyperplasia of endometrium was observed in the animals in experimental diet groups due to insulin resistance and obesity which can progress into carcinoma of the endometrium.
Limitation
Animal experimental research is beneficial in the understanding of positive correlation of insulin resistance and its effect on the endometrium because it simulates the development of human model of diet induced metabolic syndrome. Since the present study is conducted in a limited sample size, larger number of animals with a relatively longer duration of experimentation is therefore necessary.
Conclusion
The present study proves the direct correlation of metabolic syndrome such as insulin resistance and its effect on the endometrium of uterus. The present study implicates the role of high energy diets in the development of morphological lesions in the endometrium.
*p<0.05, **p<0.01
[1]. Talavera F, Reynolds RK, Roberts JA, Menon KM, Insulin-like growth factor I receptors in normal and neoplastic human endometriumCancer Res 1990 50:3019-24. [Google Scholar]
[2]. Werner H, Leroith D, The role of the insulin-like growth factor system in human cancerAdv Cancer Res 1996 68:183-223.10.1016/S0065-230X(08)60354-1 [Google Scholar] [CrossRef]
[3]. O’Mara BA, Byers T, Schoenfeld E, Diabetes mellitus and cancer risk: a multisite case-control studyJ Chron Dis 1985 38:435-41.10.1016/0021-9681(85)90139-0 [Google Scholar] [CrossRef]
[4]. Adami HO, McLaughlin J, Ekbom A, Berne C, Silverman D, Hacker D, Cancer risk in patients with diabetes mellitusCancer Causes Control 1991 2:307-14.10.1007/BF000516701932543 [Google Scholar] [CrossRef] [PubMed]
[5]. Weiderpass E, Gridley G, Persson I, Nyren O, Ekbom A, Adami HO, Risk of endometrial and breast cancer in patients with diabetes mellitusInt J Cancer 1997 71:360-63.10.1002/(SICI)1097-0215(19970502)71:3<360::AID-IJC9>3.0.CO;2-W [Google Scholar] [CrossRef]
[6]. Shoff SM, Newcomb PA, Diabetes, body size and risk of endometrial cancerAm J Epidemiol 1998 148:234-40.10.1093/oxfordjournals.aje.a0096309690359 [Google Scholar] [CrossRef] [PubMed]
[7]. La VC, Negri E, Franceschi S, D’Avanzo B, Boyle P, A case control study of diabetes mellitus and cancer riskBr J Cancer 1994 70:950-53.10.1038/bjc.1994.4277947103 [Google Scholar] [CrossRef] [PubMed]
[8]. Sankaranarayanan R, Ferlay J, worldwide burden of gynaecological cancer. The size of the problemBest Pract Res Clin Obstet and Gynaecol 2006 20(2):207-25.10.1016/j.bpobgyn.2005.10.00716359925 [Google Scholar] [CrossRef] [PubMed]
[9]. Balasubramaniam G, Sushama S, Rasika B, Mahantshetty U, Hospital-based study of endometrial cancer survival in Mumbai, IndiaAsian Pac J Cancer Prev 2013 14(2):977-80.10.7314/APJCP.2013.14.2.97723621271 [Google Scholar] [CrossRef] [PubMed]
[10]. Inoue-Choi M, Robien K, Mariani A, Cerhan JR, Anderson KE, Sugar-sweetened beverage intake and the risk of type I and tye II endometrial cancer among postmenopausal womenCancer Epidemiol Biomarkers Prev 2013 22(12):2384-94.10.1158/1055-9965.EPI-13-063624273064 [Google Scholar] [CrossRef] [PubMed]
[11]. Oettle GJ, Emmet PM, Heaton KW, Glucose and insulin responses to manufactured and whole food snacksAm J Clin Nutr 1987 45:86-91.10.1093/ajcn/45.1.863541564 [Google Scholar] [CrossRef] [PubMed]
[12]. Green R, Milner J, Joy EJ, Agrawal S, Dangour AD, Dietary patterns in India. A systematic reviewBr J Nutr 2016 116:142-48.10.1017/S000711451600159827146890 [Google Scholar] [CrossRef] [PubMed]
[13]. Reeves PG, Nielson FH, Fahey GC Jr, AIN-93 Purified diets for laboratory Rodents: Final report of the American Institute of Nutrition Ad Hoc Writing Committee on the reformulation of the AIN-76A Rodent dietJ Nutr 1993 123:1939-51.10.1093/jn/123.11.19398229312 [Google Scholar] [CrossRef] [PubMed]
[14]. Soliman PT, Wu D, Tortolera-Luna G, Schmeler KM, Slomovitz BM, Bray MS, Association between adiponectin, insulin resistance, and endometrial cancerCancer 2006 106(11):2376-81.10.1002/cncr.2186616639730 [Google Scholar] [CrossRef] [PubMed]
[15]. Amant F, Moerman P, Neven P, Timmerman D, Van Limbergen E, Vergote I, Endometrial cancerThe Lancet 2005 366(9484):491-505.10.1016/S0140-6736(05)67063-8 [Google Scholar] [CrossRef]
[16]. Key TJ, Allen NE, Spencer EA, Travis RC, The effect of diet on risk of cancerThe Lancet 2002 360:861-68.10.1016/S0140-6736(02)09958-0 [Google Scholar] [CrossRef]
[17]. Dekker MJ, Su Q, Baker C, Rutledge AC, Adeli K, Fructose: a highly lipogenic nutrient implicated in insulin resistance, hepatic steatosis and the metabolic syndromeAm J of Physiol Endocrinol and Metab 2010 299:E685-94.10.1152/ajpendo.00283.201020823452 [Google Scholar] [CrossRef] [PubMed]
[18]. Vos MB, Lavine JE, Dietary fructose in nonalcoholic fatty liver diseaseHepatol 2009 57(6):2525-31.10.1002/hep.2629923390127 [Google Scholar] [CrossRef] [PubMed]
[19]. Stanhope KL, Schwarz JM, Keim NL, Griffen SC, Bremer AA, James L, Consuming fructose-sweetened, not glucose-sweetened beverages increases visceral adiposity and lipids and decreases insulin sensitivity in overweight/obese humansThe J of Clin Invest 2009 119(5):1322-34.10.1172/JCI3738519381015 [Google Scholar] [CrossRef] [PubMed]
[20]. Miller CC, Martina RJ, Whitney ML, Edwards GL, Intracerebroventricular injection of fructose stimulates feeding in ratsNutrit Neurosci 2002 5:359-62.10.1080/102841502100003383912385599 [Google Scholar] [CrossRef] [PubMed]
[21]. Nagamani M, Stuart CA, Specific binding and growth promoting activity of insulin in endometrial cancer cells in cultureAm J Obstet Gynaecol 1998 179:06-12.10.1016/S0002-9378(98)70244-32 [Google Scholar] [CrossRef]
[22]. Yu H, Rohan T, Role of insulin-like growth factor family in cancer development and progressionJ Natl Cancer Inst 2000 92:1472-89.10.1093/jnci/92.18.147210995803 [Google Scholar] [CrossRef] [PubMed]
[23]. Antunes CL, Elkfury JL, Jornada MN, Foletto KC, Bertoluci MC, Validation of HOMA-IR in a model of insulin resistance induced by high fat diet in wistar ratsArch Endocrinol Metab 2016 60(2):138-42.10.1590/2359-399700000016927191048 [Google Scholar] [CrossRef] [PubMed]
[24]. Salgado ALFA, Carvalho L, Oliveira AC, Santos VN, Vieira JG, Parise ER, Insulin resistance index (HOMA-IR) in the differentiation of patients with non-alcoholic fatty liver disease and healthy individualsArq Gastroenterol 2010 47(2):165-69.10.1590/S0004-28032010000200009 [Google Scholar] [CrossRef]
[25]. Newbold RR, Bullock CB, McLachlan JA, Uterine adenocarcinoma in mice following developmental treatment with oestrogens. A model for hormonal carcinogenesisCancer Res 1990 50:7677-81. [Google Scholar]