Osteoporosis is a common metabolic bone disorder, yet it is underdiagnosed and undertreated in clinical settings. Osteoporosis is defined as deterioration in bone mass and microarchitecture, with increasing risk for fragility fractures [1]. Primary osteoporosis can occur in both men and women of all ages, though it often occurs in postmenopausal women. Secondary osteoporosis is the result of chronic medication use like steroids and other conditions like vitamin D deficiency and various hormonal disorders.
Osteoporosis is considered as a ‘silent disease’ since, bone loss occurs without any symptoms and is often undiagnosed until a fracture occurs. It is an issue of major public health concern as osteoporotic fractures are associated with significant morbidity and mortality. Indians are genetically predisposed for osteoporosis and have a lower average peak bone mass compared to western population. In 2013, it was estimated that 50 million people in India are either osteoporotic or osteopenic [2]. At the same time osteoporosis is a condition that can be prevented and treated if diagnosed early. Early diagnosis is essential as the beneficial effect of fracture prevention from treatment of osteoporosis is expected at least six months after initiating treatment.
The BMD scan is an essential diagnostic tool for early diagnosis of osteopenia and osteoporosis and estimation of patient’s risk of fracture. Dual-Energy X-ray Absorptiometry (DEXA) scan is considered as the gold standard. However, the commonest used modality still remains to be quantitative calcaneal ultrasound as it is cost effective, portable, easily available and lacks the deleterious effect of radiation unlike DEXA [3].
Orthopaedic surgeons are often being the first and usually the only doctor to evaluate a patient with a fragility fracture, they may be in an ideal position to initiate evaluation and early management for osteoporosis. After American Orthopaedic Association (AOA) introduced ‘Own the Bone’ programme, the idea of orthopaedic surgeons being a vital component in managing osteoporosis beyond the acute fracture management, has been given a great deal of attention [4]. Also, few studies have shown that this can lead to better management of the patients [5-7].
Even better would be if orthopaedic surgeons could do BMD screening as a routine in indicated group of patients and manage them early to prevent the fragility fractures to occur. And also there is paucity of literature regarding the prevalence of osteoporosis in India. So, we decided to do a survey on the patients who were attending orthopaedic Outpatient Department (OPD) clinics to find out the age related prevalence of osteopenia and osteoporosis and to find out the susceptible groups for early screening of BMD.
Materials and Methods
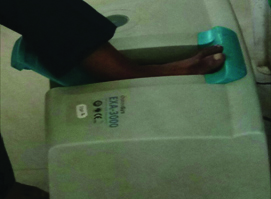
This was a multicentric cross-sectional study conducted between January 2017 to September 2017 in seven centres in the union territory of Puducherry and the state of Tamil Nadu. After Institutional Review Board clearance, all consecutive patients aged 16 years and above with various orthopaedic complaints, who were attending the orthopaedic OPD in these centres were recruited. Patients with injury to the left ankle/foot or fractures of lowerlimbs or pelvis and those with any medical comorbidities who were on chronic medications were excluded from the study. After getting written informed consents and explaining the procedure in detail, all the subjects were screened for bone mineral density using calcaneal Quantitative Ultrasound (QUS), the EXA-3000 (Osteosys) [Table/Fig-1]. The patients were seated in a chair and their left foot was kept in flush with the foot rest in the machine so that the scan was performed at the level of mid-calcaneus. Quality assurance test for the device was performed on each day of screening. The test was carried out by a single technician in all the subjects. The machine automatically converted the BMD values of the patients into T-Scores [8].
Calcaneal quantitative ultrasound machine.
A total of 956 patients were included in the study and grouped them into young adults (16-35), middle aged adults (36-55 years) and elderly (>55 years). Absolute numbers and proportions of normal, osteopenic and osteoporotic patients per age group were evaluated according to the WHO’s diagnostic categories (WHO-BMD categories): a T-score >-1 was designated as normal BMD, a T-score ≤-1.0 to >-2.5 as osteopenia, and a T-score ≤-2.5 as osteoporosis [9].
Statistical Analysis
Statistical analysis were done using SPSS version 23.0. Baseline characteristics of the study population were described using descriptive statistics. Continuous variables were described using mean and standard deviation, and compared using student t-test. Categorical data were described using frequencies and compared using chi-square test. Fisher’s exact test was used when value of any cell was less than 5. Analysis were carried out at 5% level of significance and p<0.05 (2-sided) was considered statistically significant.
Results
Total of 956 patients were recruited, out of which 505 (53%) were women and 451 (47%) were men [Table/Fig-2]. The median age of the patients was 45 years (range 16-88). Median age of men was 45 years (range: 16-88) and that of women was 44 years (range:18-85). Most patients in present study included middle age adults, 49% of men and 58% of women.
Number of men and women in each age group values are given in numbers (percentages).
| Gender | Age group (in years) | Total |
|---|
| <36 | 36-55 | >55 | |
| Men | 101 (22) | 220 (49) | 130 (29) | 451 (47) |
| Women | 122 (24) | 294 (58) | 89 (18) | 505 (53) |
Median (range) T-scores were -1.1 (-5 to 3.3) in men and -1.1 (-3.7 to 3.2) in women. Difference in T-scores between men and women was not statistically significant (p=0.68). Most men (54%) and women (51%) in the middle age group were found to be osteopenic. Overall, 52% of patients affected with osteopenia were in the middle age group. The elderly age group was found to be most affected by osteoporosis, especially women (25%). In the group of young adults, most of them had normal bone mineral density. While, 39% of men and 34% women in this group were osteopenic, 1% of men and 3% women were found to be osteoporotic [Table/Fig-3,4].
Percentage of individuals with osteopenia and osteoporosis in each age group (men) values are given in numbers (percentages).
| Age group (years) | Normal BMD | Osteopenia | Osteoporosis | Total |
|---|
| <36 | 61 (60) | 39 (39) | 1 (1) | 101 (22.3) |
| 36-55 | 94 (43) | 120 (54) | 6 (3) | 220 (48.7) |
| >55 | 49 (38) | 72 (55) | 9 (7) | 130 (28.8) |
Percentage of individuals with osteopenia and osteoporosis in each age group (women) values are given in numbers (percentages).
| Age group (years) | Normal BMD | Osteopenia | Osteoporosis | Total |
|---|
| <36 | 77 (63) | 41 (34) | 4 (3) | 122 (24.1) |
| 36-55 | 124 (42) | 149 (51) | 21 (7) | 294 (58.2) |
| >55 | 25 (28) | 42 (47) | 22 (25) | 89 (17.6) |
The overall prevalence of osteopenia and osteoporosis in present study was found to be 48.4% and 6.6% in all the age groups. Women had more prevalence of osteoporosis (9.3%) while men had only 3.5%. But osteopenia was 5.3% more prevalent in men (51.2%) than women (45.9%).
Discussion
We have a unique study population, since we included even patients who were considerably younger than those included in any other studies investigating the epidemiology of osteoporosis. The youngest patient was 16-years-old and the mean patient age was 45 years. Maximum numbers of present study patients were in the age group of 35-55 years. The under-representation of elderly in the study might be due to their more frequent inpatient treatments than OPD treatments.
Osteoporosis is usually considered a disease of the elderly. According to International Society for Clinical Densitometry (ISCD) guidelines, BMD screening is routinely to be done in women aged 65 or older. The National Osteoporosis Foundation (NOF) also recommends bone density screening for all women aged 65 years or older and all men aged 70 years or older and so do some of the other studies [10-13]. Present study shows that in the elderly, 25% women had osteoporosis which is more than three times higher than the prevalence observed in men (7%) in the same age group, which is consistent with the existing studies and support the need for BMD screening in this population [14].
The corresponding rates of patients with normal BMD decreased from 60% in men and 63% in women in the youngest group to 38% and 28% in men and women respectively in the oldest age group. This is explained by the fact that peak bone mass is attained in the third decade and then gradually decreases as the age increases in both age groups, with a female preponderance, though they had similar percentage of normal BMD in the youngest age group. Low BMD is more common in elderly women than in men due to the fact that women have lower BMD to begin with, and the bone loss that occurs with ageing occurs more rapidly, especially after menopause when the protective effect of oestrogen starts to fade [15].
The main finding of the present study was the high prevalence of osteopenia in the middle-age group (51.2%). There are already few studies by Donescu OS et al., and Chen JH et al., which have shown the importance of detecting osteopenia in the middle age group [16,17]. Nayak S et al., demonstrated that screening for postmenopausal osteoporosis leads to more quality-adjusted life years compared with no screening. Their model analysis proved that the most cost effective strategy would be to start screening postmenopausal women from age of 55 years [18]. And later, study by Kling UM et al., showed all high-risk postmenopausal women and men from age of 50 years should be screened for low BMD [19].
Not many studies have separately studied prevalence of osteopenia in middle age group until recently. Boschitsch EP et al., carried out an age related prevalence study at the menopause and osteoporosis outpatient clinic Klimax in Vienna. It showed 31.1% women between 40-55 years age group had osteopenia and 4.5% had osteoporosis. There was high prevalence of fractures in middle aged women, with many fractures occurring in women with non-osteoporotic BMD, confirming the significance of early detection of osteopenia in this age group [20]. Another study by Chen JH et al., from Taiwan showed only 8% of women between 40-55 years had osteopenia [17]. Present study shows 54% of osteopenia in the men and 51% in women in the age group of 35-55 years, which is much higher than both the above studies which were conducted in different population. But present study is concurrent with few of the studies done in Indian population. A similar study in 1188 orthopaedic outpatients by Qureshi A et al., showed a prevalence of 45.6% and 44.8% osteopenia and 8.6% and 5.8% osteoporosis in men and women respectively, in the age group of 40-59 years [21]. One cross-sectional study done in patients from southern India with various conditions of musculoskeletal pain in the age group above 50 years of age, demonstrated osteoporosis in 50% and osteopenia in 36% [22].
Another cross sectional study by Agarwal MT and Verma AK in Indian women, using calcaneal QUS showed that 48.6% of the study patients in the age group of 35-54 years had osteopenia and 11% had osteoporosis [23]. In a hospital based study among urban women above age of 25 years utilising calcaneal QUS by Sharma S et al., 20.25% and 36.79% detected to have osteoporosis and osteopenia respectively [24]. While retrospective study in Indian women of 40-60 years age group by Acharya S et al., using DEXA scan documented 18.41% osteoporotic and 47% osteopenics [25]. Das BG et al., studied a total of 1206 women using calcaneal QUS and recorded osteopenia in 65.9% and osteoporosis in 11.2% in age group of 31-45 years and osteopenia in 41% and osteoporosis in 32.1% in the age group of more than 45 years [8].
The increased prevalence of osteopenia in present study and the other Indian studies, compared to other study populations could be explained by genetic susceptibility of Indian population for osteoporosis, high risk of hypovitaminosis D in Indians due to higher 25(OH)-d-24-hydroxylase enzyme and dark pigmentation of their skin which reduces the effect of sunlight exposure. The other factors are their changing life style (alcohol consumption, smoking, and lack of physical exercise), inadequate calcium intake, lack of diagnostic facilities in rural set ups and unawareness of osteoporosis among the general population. Vitamin D deficiency is an important risk factor for the development of osteoporosis in any age group [26,27]. Hypovitaminosis D adversely affects calcium metabolism, osteoblastic activity, matrix ossification, bone remodelling, and hence bone mineral density. Indian diets are mostly vegetarian, and the consumption of dairy products is minimal in the lower socioeconomic population. So, it is recommended to consume diets rich in calcium, encourage physical excercise and adequate sun light exposure for adequate bone health.
Also according to Canadian guidelines, BMD test is not necessary in every case to estimate fracture risk especially the very high risk patients, and elderly patients who have a typical osteoporotic proximal femur or vertebral fracture, who can be considered for osteoporotic treatment without a BMD evaluation [28]. So, the aim of BMD screening should be to prevent the fragility fractures and for that it might be necessary to evaluate BMD even in middle age patients for early detection of osteoporosis as well as osteopenia instead of waiting till 65 years as per previous recommendations [10,11,12,13]. It is supported by the results from the National Osteoporosis Risk Assessment (NORA) which showed that osteoporosis was associated with a fragility fracture risk approximately four times that in normal BMD while osteopenia was associated with a 1.8-fold higher rate. Further, the same study also showed that the risk of fracture is not years later in the future, but rather exists at the time of diagnosis [29].
The present study, confirms that the prevalence of osteopenia and osteoporosis in middle aged women is so far under-recognised. Present results along with the other studies discussed above, point to a need to shift from the preoccupation with BMD as a disease of elderly to decrease the morbidity and mortality in the affected patients.
Limitation
We did not consider diagnosis of the patients as a variable. There is a scope for further studies looking into this matter, whether any particular diagnosis made in an orthopaedic outpatient set up has a preponderance to osteopenia or osteoporosis.
Conclusion
Routine BMD screening is recommended in elderly population, especially in women. The need for early detection of osteopenia and osteoporosis is underestimated. In present study, we found a high prevalence of osteopenia and osteoporosis even in the age group of 35-55 years, in both men and women. This finding is concurrent with some of the recent studies on osteoporosis and hence we recommend that BMD screening should be made as a routine investigation even in the middle aged orthopaedic outpatients.