Road traffic injuries are the ninth leading cause of death globally; responsible for over 1.25 million deaths each year, therefore, contributing to high mortality and socioeconomic costs [1]. It contributed to nearly 1.3 million deaths due to road injuries (2015) [2]. About 54.1 per cent of all persons killed in road accidents were in the 15-34 years age group during the year 2015 in India [3]. Mechanics of road traffic accidents are complex and are governed by an array of factors that contribute to road traffic injuries causing morbidity or mortality. The aggressive and inappropriate use of cellular mobile phones while driving may make the scenario even graver. Studies suggest that drivers using mobile phones while driving were approximately four times more likely to be involved in a crash as compared to drivers not using phones while driving [4].
This emphasizes the fact that amongst the various core competencies required for driving, psychomotor skills, alertness and visual acuity are important ones. One of the key risk factor for RTA along with the previously mentioned ones also includes use of prohibited drugs by driver while driving e.g. Anti-histaminic (anti-H1) drug (especially first generation) [5,6]. Cetirizine is a second generation anti-H1. It is an active metabolite of hydroxyzine (first generation drug) [7]. Although Cetirizine belongs to the second generation of anti-H1, its propensity to cause sedation is a matter of controversy [8]. Its use is wide spread by virtue of its quick onset of action and higher efficacy as compared to other second generation anti-H1 [8]. Numerous studies have shown these unwanted effects of Cetirizine may affect psychomotor performance during routine activity such as driving [9,10]. A report by the National Highway Traffic Safety Administration (NHTSA) branch of US Department of Transportation recently released its report in April 2015 regarding mobile and driving which mentioned that main cause of crashes with mobile use was the driver being distracted. This report has data updated till the year 2013. The report does not elaborate on the mechanisms and extent of distraction due to mobile use while driving [11]. The WHO report also emphasizes that research is also needed to understand the impacts of different forms of mobile phone use for instance, conversation and texting on driving behaviour and accidents risk more importantly in real-life settings [4]. However, there is a paucity of studies that measure the extent of distraction or effect of cellular mobile phones related changes in psychomotor skills and visual acuity.
Hence, this study was conducted to find the effect of concurrent use of cellular mobile phone on the variations in hand-eye coordination and visual acuity and compare such variations with that produced by a single oral dose of Cetirizine 10 mg.
Materials and Methods
It was single blind, single dose and interventional study; conducted in Department of Pharmacology, BJ Government medical college and Sassoon General Hospital Pune, India. The study was conducted after obtaining approval from Institutional Ethics committee (IEC Ref No.- ND-Dept 0415066-66, dated 21/04/2015). It was conducted over two months in May 2015 and June 2015.
Healthy human volunteers were selected from the teaching and non-teaching staff of the institute, who were mobile users and also regular vehicle drivers. A written informed consent form was taken from each of the participants prior to the study. For calculation of sample size, WHO report data of police crash reports in United States of year 2005 was used, where the reports of crash while driving and mobile use was 5.8% [4]. Open Epi was used to calculate the sample size with:
Two sided significance level – 95% (1-alpha)
Power – 80 % (1-beta)
Ratio of exposed to unexposed – 1
Risk/prevalence ratio – 5.8%
Sample size in each group should be 38-46 volunteers and total minimum 92
Hence, this study had screened 110 and enrolled 100 eligible healthy volunteers with random allocation of 50 volunteers in each group.
Total 100 healthy volunteers, age between 18-55 years, with vision 6/6 or corrected vision 6/6, with no pathology or injury that will interfere with fine and gross movement of the upper limb and visual acuity were enrolled. Those volunteers regularly consuming alcohol, smoking, drug abuser, having any psychiatric disorder affecting his/her psychomotor and mental abilities, who were suffering from other central nervous system disorders like epilepsy, sleep-disorders, narcolepsy and insomnia were excluded study from the study. Participants unwilling to give consent or participate were excluded. The volunteers had to pickup folded chits from a bowl. This bowl contained a total 100 chits - 50 chits written as “Group-1” and other 50 as “Group-2” – all were well folded to obscure the written material and mixed well in the bowl. Thus, the eligible volunteers were assigned into two groups (n=50) in a crude fashion, randomly.
Group I- Cetirizine group (Tab. Cetirizine 10 mg orally stat)- volunteers, who only received the drug.
Group II- Cellular phone group- volunteers, who only answered the phone call while performing the test and did not receive any drug.
Apple- i phone 5C was used by all volunteers to receive the call whereas Micromax A1 20 was used by investigator for making a phone to the volunteer. The respective mobile handsets were used by all the volunteers and investigators in the study, as these smart phones were researcher’s phones and were available and used for convenience. The readings of the various tests were observed and recorded by other observers who were unaware of the volunteers’ group assignments.
After allocating to either group, baseline reading was taken for each participant from each group on each instrument which acted as the respective control as this could minimize individual variation in readings. No different group was used as control group.
Tests were repeated three hours later for both the groups so as to maintain the blinding of the procedure for the observer, Group-I after administration of Tab. Cetirizine 10 mg oral stat only (no phone call), (Film coated tablet contain Cetirizine Hydrochloride IP 10 mg, Titanium Dioxide IP, manufactured by ZEST PHARMA, batch no.T5295, MFD- 04/15, Expiry date 06/17). Group-II: This group did not receive any drug but had to perform the same tests as group-I simultaneously while picking up and answering the call on a standard cell phone which lasted till the test tasks were completed. The call was made so as to engage the subjects on phone call for approximately 8-10 minutes till the tasks were performed by them. The parameters of distraction which could affect the outcome of the study like ringtone of the mobile and sitting positions of the volunteers were maintained uniformly for all participants. Other parameters like ambient noise distraction were minimized as well as luminosity of the study room was standardized and maintained throughout the project.
The reaction time was recorded in seconds and CFFF in frequency/second. Reaction Index was calculated as follows:
Reaction Index= Reaction time (sec) X Hole diameter (mm)
Following two instruments were used in the study:
Steadiness tester: (Inco the Instrument Specialist- Instrument and Chemical Pvt.-Ltd. M2×5-962).
A standard steadiness tester was used to test the hand-eye coordination and concentration of the volunteers [12].
Instrument: The test surface of the hand steadiness tester apparatus is situated at an angle of 45° to the horizontal. The test panel consists of nine holes, spaced 1.5 cm apart, arranged in two rows. The holes were 2.5-6.5 mm with a progressive increase in 0.5 mm of diameter whereas, the first two big holes were of 12.5 and 8.0 mm respectively. A metal stylus with attached stainless steel probe of 1 mm diameter is wired such that when the probe touches the panel or rim of the hole the circuit get completed. This generates a beep signal that alerts the subject and observer. The height at which the apparatus was placed was constant. The baseline values of the subject which act as controls were noted with respect to post-intervention reaction time in seconds with the use of stopwatch.
Flicker fusion Apparatus: (Medicraft Manufacturer, Serial No. 715/FF-008).
Critical Flicker Fusion (CFF) measurement is non-invasive and of good reliability in assessing cortical arousal and a good marker of cortical alteration to physical workload, drug administration and alcohol intoxication [13].
The device consists of a rotating ring, surrounding a short cylindrical waterproof housing of 8 cm diameter containing the numeric frequency indicator. Attached to this housing is a flexible cable, on the end of which a single LED (Light Emitting Diode) red colour is enclosed in a smaller cylindrical container (to shield it from stray light and reflections). The subject to be tested was instructed to look straight at the LED light at a distance. The investigator turns the dial gradually clockwise in order to increase the flickering frequency of the light. CFFF is said to be the actual frequency at which the subject/volunteer notices a change of light from flicker to fusion. This is subjective as the subject/volunteer signals this to the investigator [13].
The volunteers underwent these tests three times on different occasions and the average of the three measurements was considered for the analysis and interpretation.
Statistical Analysis
Student’s paired t-test was applied to calculate change from baseline reading to three hours in each group as regards the various parameters i.e., reaction index, reaction time, CFFF (low and high intensity), this was the intra-group (within the group) comparison. Student’s unpaired t-test was applied for intergroup comparison of the same parameters at baseline and at three hours. Graph pad prism 6.0 software was used to perform the statistical tests.
Results
The Cetirizine group (Group-I) included 24 females and 26 males whereas mobile group (Group-II) included 20 females and 30 males. The mean age of the volunteers in the Cetirizine group was 28.64 (±8.10) years and that of the volunteers in mobile group was 26.22 (±5.14) years. All the volunteers had minimum education till high school. Precisely, 32 volunteers in the Cetirizine group and 36 volunteers in the mobile group were educated minimum till graduation level. The baseline values of both the groups were comparable as regards the reaction index, reaction time and CFFF (low and high intensity) of the Cetirizine group (Group-I) and mobile group (Group -II) and no statistically significant difference existed between the two groups(p->0.05) [Table/Fig-1].
Comparison of baseline value of both the groups as regards to various parameters of alertness.
| Parameters ofalertness(Baseline- 1st reading) | CETIRIZINE(Group-I) | MOBILE(Group-II) | p-value |
|---|
| Reaction Index | 95.46±41.74 | 85.11±39.05 | 0.3625 |
| Reaction Time(in seconds) | 19.82±11.31 | 15.83+7.93 | 0.0707 |
| CFFF(low intensity)(frequency/sec) | 40.07±9.970 | 40.42±9.035 | 0.6307 |
| CFFF(high intensity)(frequency/sec) | 40.76±9.309 | 40.48±9.863 | 0.8859 |
Mean±SD, Students’ unpaired t-test applied, **p-value <0.05 as significant
Similarly, no significant difference was observed (p>0.05) when the two groups were compared regarding all the parameters (i.e., reaction index, reaction time, CFFF at both intensities) when reading was taken after three hours [Table/Fig-2].
Comparison of three hours value of both the groups as regards to various parameters of alertness.
| Parameters ofalertness(at 3 hrs-2nd reading) | CETIRIZINE(Group-I) | MOBILE(Group-II) | p-value |
|---|
| Reaction Index | 116.4±51.46 | 102.8±49.26 | 0.1809 |
| Reaction Time(in seconds) | 24.69±12.69 | 23.46±11.76 | 0.643 |
| CFFF(low intensity)(frequency/sec) | 40.16±10.98 | 41.26±9.319 | 0.5389 |
| CFFF(high intensity)(frequency/sec) | 39.59±10.42 | 41.39±9.432 | 0.3674 |
Mean±SD, Students’ unpaired t-test applied, **p-value<0.05 as significant
When the three hour reading (post-drug administration) of Cetirizine group (Group-I) was compared with the baseline reading there was a statistically significant increase in the reaction index (p=0.0017) [Table/Fig-2,3] and also increase in reaction time (p=0.001) [Table/Fig-4]. Similarly when the three hours reading (i.e., during the “on phone” session) of mobile group (Group-II) was compared with that of baseline there was a statistically significant increase in the reaction index (p=0.001) and reaction time (p=0.0011) [Table/Fig-3,4]. There was no statistically significant increase or decrease in the CFFF (low and high intensity) when such intra-group comparison of three hour reading and baseline were done for both the groups (p> 0.05) [Table/Fig-5].
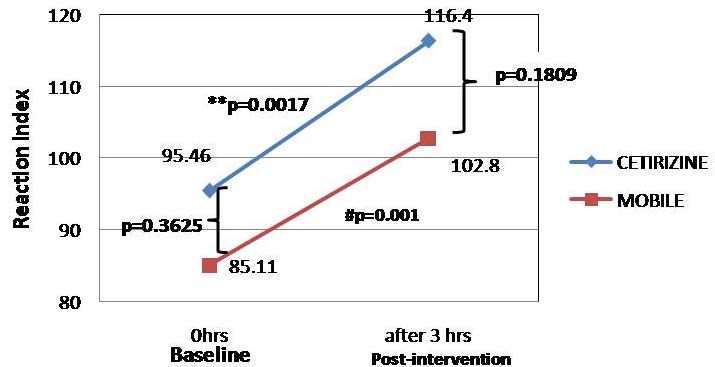
Reaction Index inter-group and intra group comparison between at baseline and at three hours reading.
Inter-group: baseline and Post-intervention values of the two groups compared p=0.3625 and p=0.1809 respectively. Intra-group: baseline Vs post-intervention- Cetirizine group **p=0.0017 and mobile group #p=0.001. (p<0.05 statistically significant)
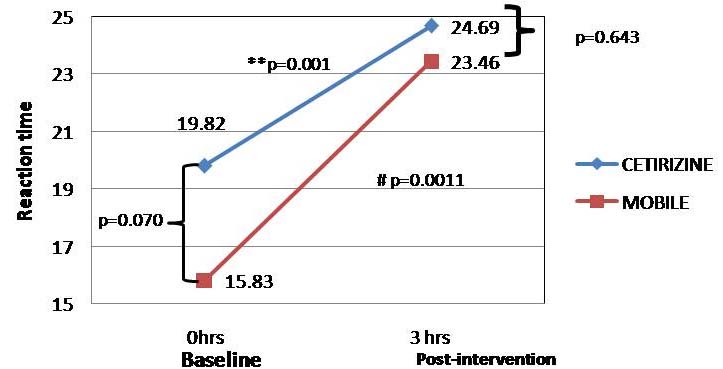
Reaction Time inter-group and intra-group comparison between at baseline and at three hours reading.
Inter-group: baseline and Post-intervention values of the two groups compared p=0.070 and p=0.643 respectively. Intra-group: baseline Vs post-intervention- Cetirizine group **p=0.001 and mobile group #p=0.0011. (p<0.05 statistically significant
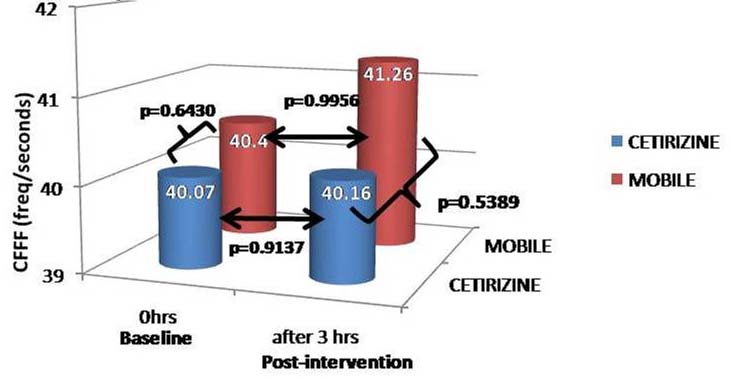
CFFF (low intensity) inter-group and intra-group comparison between at baseline and at 3 hours reading.
Inter-group: baseline and Post-intervention values of the two groups compared p=0.643 and p=0.5389 respectively. Intra-group: baseline Vs post-intervention- Cetirizine group p=0.9137 and mobile group p=0.9956. (p<0.05 statistically significant)
Discussion
Evidences show around 1% to up to 11% of drivers use cellular phones while driving and this has been increasing over the past decade [4]. Mobile phones serve as a major distraction and may contribute to crashes. A study done in naturalistic driving situations revealed that 22% of car crashes and near crashes and 71% of truck crashes (and 46% of near crashes) occurred due to such mobile distraction [11].
Although, such alarming statistics are available since past few years, yet data on mobile use by driver during accident is seldom collected; whereas, this exercise is done for drinking and driving strictly. Several studies have delved in the details of mechanics of accidents caused due to mobile use while driving. Sumer N et al., in their study have included Reaction time is an integral aspect of hazard perception skill which affects psychomotor abilities and therefore, predicts risky driving behaviour [14]. Similar findings have been reported in another study by Redelmeier et al., wherein they found 4 to 6 times increased risk of motor vehicle collision with use of cellular phones while driving [15].
This study evaluates the effect of cellular mobile phone use on hand-eye coordination and visual acuity in healthy human volunteers as compared with a single dose of 10 mg Cetirizine. In the present study, the reaction index as well as the reaction Time (in seconds) for hand-eye coordination was significantly increased in both groups (Cetirizine and cellular mobile phone) after intervention as compared to their respective baseline readings. This finding for the mobile group is in accordance with findings of another similar study by Sumer N et al., [14].
It also impressed the fact that use of Cetirizine certainly has significant impairment of psychomotor abilities. Earlier, antihistaminics were found to impair psychomotor performance and sedate substantially whereas, the second generation antihistamines are establishing their status of being free from such potential adverse effects. Despite of such claims research has shown that there is a grey area still remains which doubts the latter. Therefore, there are studies that have investigated to explore it [16].
Cetrizine tends to affect psychomotor performance, three to four hours after oral administration. A double blind cross-over placebo controlled trial was conducted in 16 healthy human volunteers in real time driving road test. It compared the impairment caused by Cetirizine 10 mg in single dose with other groups loratadine 10 mg and also alcohol. One of the important conclusion of this trial included the finding that the effects of single dose 10 mg Cetirizine on driving performance resembled those of alcohol [17].
However, the important fact that needs to be highlighted is that, the increase in reaction index and reaction time after intervention (or at three hours) in cellular mobile phone group was not significantly different, when compared with that of Cetirizine group (p< 0.64). This suggests the impairment of psychomotor skills and delay in reaction time due to mobile use are comparable to anti-H1 use which can be hazardous while performing skilled work like driving or machine operation.
There is a definite significant relationship between Visual Acuity impairment and road accidents [18]. Astonishingly there was no significant impairment in CFFF reading in both (in low or high intensity) the groups when each post-intervention reading was compared with respective baseline reading. Hence, highlighting the fact that, the Cetirizine group or the mobile did not show any statistical difference in CFFF reading after intervention as compared to baseline; thus, denoting there is no significant alteration in visual acuity due to use of either single dose Cetirizine or use of mobile while performing task. This finding is in accordance with another study conducted by David VK et al., [8].
Limitation
The present study has certain limitations only healthy human volunteers were enrolled for the study and patients were excluded. A possibility that certain pathologies viz., allergic rhinitis, disturbed sleep-wake cycle due to allergic manifestations too could contribute to somnolence. The other factor that needs consideration was that the volunteers were aware about the incoming call on given cellular mobile phone before performing the test; whereas, in real life situation unpredictable call may divert the attention more significantly. All sets of cellular phones (Non-Smartphone, Androids, Windows, Apple, etc.,) each phone is having different sensitivity to touchpad to receive the phone which may affect the level of distraction and psychomotor performance. These are the aspects that need to be studied in future.
Conclusion
On the contrary, to the common myth, Cetirizine does possess significant detrimental effects on psychomotor performance of the recipients but it does not significantly impair the visual acuity. The use of cellular mobile phone also cause detrimental effects on psychomotor skills comparable to that produced by use of Cetirizine and this is more disturbing while performing skilled tasks. The distraction caused with the use of mobile phones while talking is the main reason for the impairment of psychomotor skills while performing any task and the extent of impairment is equivalent to that produced by Cetirizine.
As use of cellular mobile phones is rampant and aggressive such impairments in psychomotor skills may translate to various forms of accidental disasters while driving or operating machinery as warned that for the anti-H1 drugs. This finding needs to be confirmed by simulated experiments in humans, which may give an insight for better understanding of mechanics of accidents with mobile use. Also, such studies of comparisons with known risk factors/drugs may be useful to create public awareness.
Mean±SD, Students’ unpaired t-test applied, **p-value <0.05 as significant
Mean±SD, Students’ unpaired t-test applied, **p-value<0.05 as significant