Introduction
Globally, incidence of Chronic Kidney Disease (CKD) is rapidly rising with huge burden on the life expectancy of the patients. Regular haemodialysis improves the quality of life in these patients. They get treatment at either government run or private sector hospitals. A difference in disease pattern, comorbidity, patient management and number of access failures can be observed in these set ups.
Aim
The present study was carried out to find out selection, management and disease pattern of CKD patients admitted for dialysis in government run and private hospital.
Materials and Methods
A cross-sectional study on patients (18–90 years) admitted and undergoing dialysis at government run (N=129) and private hospital (N=182) was undertaken in Karnataka, India. Parameters like comorbidity (diabetes), number of dialysis per week, number of access failures, and follow up visits were compared between these patients. Chi- squared test was used to compare the data. All tests were two-tailed and p< 0.05 was considered as significant.
Results
More number of younger patients and associated comorbidity, were seen in patients admitted in government run hospital (p<0.001), with no gender bias in selection of patients for dialysis between the two hospitals. Similarly, follow-ups with nephrologist, number of dialysis done per week and erythropoietin supplements administered were significantly more among private hospital patients (p<0.001). Number of dialysis sessions and mean haemoglobin level was less in government run hospital patients, as compared to those in private hospital. No statistical difference was seen with access failure in both these setups.
Conclusion
No bias in management of CKD patient was seen among the two sets of hospitals though available facilities seemed to vary.
Access failure, Dialysis, End stage renal disease
Introduction
[6]. CKD is a clinical condition associated with a continuous loss of renal function over time. CKD damages the kidneys and decreases their ability of functioning. Globally, chronic kidney disease is spreading very fast with huge burden on the life expectancy of the patients [1]. It is classified into five stages based on the level of urinary protein excretion and estimated glomerular filtration rate from age, race, sex, and serum creatinine concentration [2]. Diabetes and hypertension are considered as the two important risk factors for CKD. Changing lifestyle, uncontrolled hypertension, ischemic heart diseases, diabetes and lack of proper awareness are resulting in more prevalence of chronic kidney disorders [3,4]. It is not only restricted to developed countries, it is also seen in developing nations, both urban and rural population being affected [5,6].
In the western countries, with rising prevalence of CKD, financial burden on them has increased drastically. In India, it is estimated that about 7.85 million people are suffering from end stage kidney disease [7]. As the criteria used for diagnosis of CKD diagnosis differs from researcher to researcher, the prevalence of CKD has been quoted as 0.785% by Agarwal SK et al., 4.2% by Singh NP et al., and 3.02% by Varma PP et al., [8-10].
Early detection of disease and appropriate treatment can keep CKD progression to a minimal level. The most common treatment modality used to manage CKD is haemodialysis which improves the quality of life and provides a better health status to the patient. In urban areas with easy availability of advanced medical facilities, proper care to the CKD patients is available but with varied costs. The treatment costs vary from place to place and it is indeed a burden on patients’ finances. In rural scenario, without the above added advantages in screening and treatment modalities of CKD, the situation gets unreported and often not noticed. Every End Stage Renal Disease (ESRD) patient cannot get an ideally matched renal transplantation due to multiple factors. In a study in 2009, it was estimated that only 10% of the patients with ESRD can secure a renal transplantation [11].
Added to that, these CKD patients usually have comorbid complications like hypertension, hypotension, fragile bones, poor nutritional health, diabetes, aneurysms, infections etc. They are at increased risk for cardiovascular diseases. Most patients with CKD die of cardiovascular disease complications rather than progress of ESRD. Anaemia is commonly seen due to inadequate synthesis of erythropoietin by the kidneys. This worsens as the disease progresses. It is also observed that patients with diabetes may present with anaemia of CKD earlier than people without diabetes [12,13].
In Indian setting, to treat these CKD patients, government sector is doing a fair job in managing the patients with haemodialysis and subsequent management. This setting usually caters to the needs of the rural and socioeconomically poorer section of the society. There are also government run private sector hospitals providing similar services at a reasonably low cost. But major treatment and management of such cases is occurring at urban superspeciality private hospitals where patients who are financially sound, get the treatment facilities.
Hence, different set of patients get treatment at these the two different sectors; government and private. There might be difference in disease pattern, duration of illness, duration of comorbid complications, number of access failures, follow up visits advised and practiced, number of dialysis per week, erythropoietin levels required, based on their haemoglobin levels. Hence, the present study was carried out to find out the selection, management and disease pattern of CKD patients on dialysis admitted in government run and private hospital. Also, to find out the difference in selection gender wise and age-wise.
Materials and Methods
The present cross-sectional study was done on patients admitted for dialysis in government run and private hospital, in the age group of 18–90 years. For this study, we included 129 patients from government run hospital and 182 from a private hospital in Karnataka, India, during 2015 to 2016. Ethical approval was obtained for this study from the Institute’s Ethical Review Committee. Written informed consent was taken from each participant after describing in full detail the procedure and purpose of the study. General physical examination, complete systemic examinations were done. Detailed history which included the work history, diet history, family, drug history and diabetic history as comorbidity were taken. Previous dialysis details with reference to number of access failures, follow up visits practiced, number of dialysis per week were also noted.
Inclusion criteria: Patients of CKD on dialysis were included in the study.
Exclusion criteria: Age less than 18 year and pregnant ladies were excluded from the study.
Statistical Analysis
Data were analysed for normal distribution. All these parameters among patients admitted in two different settings were analysed statistically by using the statistical software SPSS version 22 and MS Excel. Chi-squared test was used to compare the data. All tests were two-tailed and p<0.05 was considered as significant.
Results
[Table/Fig-1] shows the age group of the patients admitted to government run and private hospitals. More number of younger patients (20-39-year-old) were seen in government run hospital which was statistically significant (p<0.001).
Age group of patients admitted to different hospitals.
| Age group | Government Hospital N=129 | Private Hospital N=182 | p-value |
|---|
| 20-39 YearsN=71 | 42 (32.6%) | 29(15.9%) | <0.001 |
| 40-59 YearsN=59 | 35(27.1%) | 24(13.2%) |
| 60-69 YearsN=88 | 32(24.8%) | 56(30.8%) |
| 70 Years and aboveN=93 | 20(15.5%) | 73(40.1%) |
Chi-square test
[Table/Fig-2] shows that there exists no gender bias in selection of patients for dialysis between the two hospitals.
Gender-wise selection of patients for dialysis in government and private hospitals.
| Hospital | | No. of patients admitted | Percent | p-value |
|---|
| Government | Male | 83 | 64.3 | 0.622 |
| Female | 46 | 35.7 |
| Total | 129 | 100.0 |
| Private | Male | 122 | 67.0 |
| Female | 60 | 33.0 |
| Total | 182 | 100.0 |
Chi-square test
Age-wise comparison of diabetes as comorbidity among patients of government run and private hospital is shown in [Table/Fig-3]. Young patients in the age group of 20-39 years were seen more in government run hospital whereas patients aged 60 years and above were taking treatment in private hospital which was statistically significant for different age groups (p<0.001).
Age wise comparison of Comorbidity among patients of government and private hospitals.
| Age group | Comorbidity | Government Hospital N=129 | Private Hospital N=182 | Total | p-value |
|---|
| 20-39 YearsN=71 | Yes | 0(%) | 29(16%) | 29 | <0.001 |
| No | 42 (33%) | 0(%) | 42 |
| Total | 42 (32.6%) | 29(15.9%) | 71 | |
| 40-59 YearsN=59 | Yes | 05(4%) | 24(13%) | 29 | <0.001 |
| No | 30(23%) | 0(%) | 30 |
| Total | 35(27.1%) | 24(13.2%) | 59 | |
| 60-69 YearsN=88 | Yes | 17(13%) | 56(31%) | 73 | <0.001 |
| No | 15(12%) | 0(%) | 15 |
| Total | 32(24.8%) | 56(30.8%) | 88 | |
| 70 Years and aboveN=93 | Yes | 15(12%) | 73(40%) | 88 | <0.001 |
| No | 05(3%) | 0(%) | 05 |
| Total | 20(15.5%) | 73(40.1%) | 93 | |
Chi-square test
[Table/Fig-4] shows the disease pattern of patients on dialysis admitted to government run and private hospital. Comorbidity was seen more among government run hospital patients compared to private which was statistically significant (p<0.001). No statistically significant difference was seen in number of access failure between the two set ups.
Disease pattern of patients on dialysis admitted to government and private hospital.
| Parameter | | Government Hospital N=129 | Private Hospital N=182 | p-value |
|---|
| Comorbidity | Yes | 37(28.7%) | 182(100%) | <0.001 |
| No | 92 (71.3%) | 0 |
| No. of Access failures | 0 | 84(65.1%) | 138(75.8%) | 0.068 |
| 1 | 30(22.3%) | 13(16.5%) |
| 2 | 13(10.1%) | 08(4.4%) |
| 3 | 02(1.6%) | 03(1.6%) |
| 4 | 0 | 03(1.6%) |
| Hb(%) Mean | | 10 gm/dL | 9.4 gm/dL | |
Chi-square test
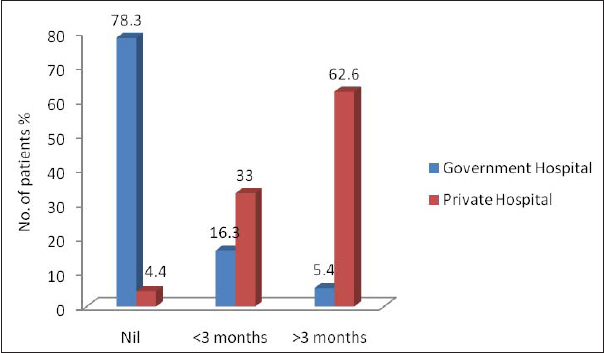
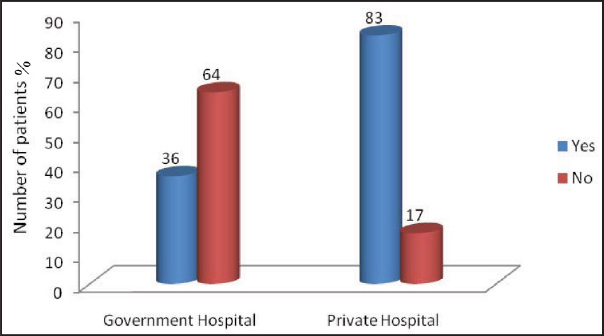
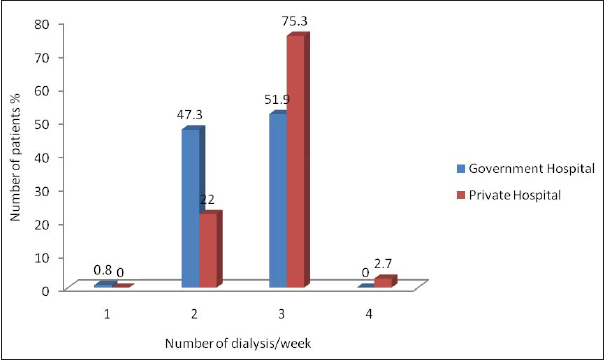
Follow-ups with nephrologist [Table/Fig-5], erythropoietin supplements administered [Table/Fig-6] and number of dialysis done per week were significantly more among private hospital patients (p<0.001) [Table/Fig-7]. Number of dialysis sessions in government run hospital was less compared with those in private. In private hospitals, it was thrice weekly in contrast with twice weekly in government run hospital [Table/Fig-7].
Follow up with nephrologist among government and private hospital.
EPO supplement of patients of government and private hospital.
Number of dialysis/week of patients of government and private hospital.
Mean haemoglobin levels of patients in government run hospital was 10 gm/dL compared with 9.4 gm/dL in private hospital.
Discussion
Chronic kidney disease is a life threatening medical, social and economic problem for patients and their families, in developing countries. Late diagnosis and failure of treatment initiation at the earliest to slow the progression of renal failure result in a predominantly young ESRD population. Financial considerations play a significant role for an appropriate treatment in such patients. In our study, we observed that relative age of patients getting admitted to government run hospital for dialysis is lesser when compared with that in private hospital. This shows that young patients are given preference in government run hospital and no such disparity existed with respect to private hospital. This is in accordance with a study conducted in government run hospitals of Africa and in most sub-Saharan countries. This also can be due to young overall population demographics in these countries [14,15]. A retrospective study of kidney disease patients who required haemodialysis done in 2013-2015 in Ethiopia showed that younger patients were treated in government run hospitals with a mean age of 36.7 years with very less pre morbid conditions [16]. In a study conducted in Australia and New Zealand by Gray NA et al., to assess dialysis modality at government and private hospitals observed that, patients were aged in private hospitals compared with government run public hospitals [17]. There exists no bias with the age group of patients getting treated in private hospitals.
Similarly, there is no bias observed in selection of patients admitted for dialysis to government run and private hospital based on their gender. Number of male patients admitted was more in both hospital set up. This is in accordance with a study conducted in Japan which mentions that differences in the socioeconomic conditions and lifestyles between genders might be due to the difference in incidence of ESRD and dialysis [18].
We found that comorbid complications were seen more among patients treated in government run hospital when compared with private hospital. A prospective randomised clinical trial in Brazilian University Hospital conducted in 2012-2013 revealed that patients admitted had comorbid complications like hypertension, diabetes, heart diseases and multi organ failures [19].
There was no statistically significant difference seen in access failure among the patients of both these hospitals i.e., 65% in government run hospital and 75% in private hospital which reveals that irrespective of the type of hospital in which patients are getting treated, nephrologists role in treating them remain the same.
Number of dialysis per week was seen more in private than the government run hospital. In private sector hospitals, decision on number of dialysis per week is based on medical conditions which are not so observed in government run hospitals [20].
Regular follow up of patients on dialysis, was observed in our study among patients of private hospital. It is oblivious that those who could afford to pay more money and those who are financially well off would be taking treatment by a nephrologist with periodic follow up in private sector hospitals when compared with government run hospitals. It is a clear fact that early referral of chronic renal failure patients to the nephrologists results in better patient management and outcome [20,21]. Patient improvement increases with the longer duration of pre-dialysis follow up by a nephrologist periodically [22,23]. It is a proven fact that specialist follow up after hospitalization for all acute conditions improves quality of life. Another study showed that regular follow up with a nephrologist within 90 days of discharge is associated with a decrease in mortality within two years of the index date, and a decrease in the need for chronic dialysis. Regular follow up with nephrologist is associated with decreased mortality, re hospitalization, and emergency room visits [24,25]. It has been observed that the number of fistula failures were low in patients followed for more than three months.
A study was conducted by Harel Z et al., in Ontario, on hospitalized adult patients with acute kidney injury who received temporary dialysis and post discharge survival of 90 days. The mortality rate was only 8.4% in those patients with regular nephrology follow up compared to 10.6% in those without follow up [26]. A total of 51% patients of government run hospital underwent dialysis thrice weekly compared with 75% in private hospitals which showed a statistical significance which could be due to patient overload and affordability.
Erythropoietin is used to treat anaemia in patients with CKD that can improve the quality of life and decrease morbidity and mortality. Erythropoietin stimulating agents are a standard feature of management for patients with ESRD. With medicare reimbursement of erythropoietin, its use has increased more so in private hospitals [27]. As per 2009 statistics, the cost of each haemodialysis in India ranged from 150 INR in government hospitals to 2000 INR in private hospitals. The monthly cost in private hospitals average 12000 INR and the yearly cost of dialysis is 1, 40000 INR. The average cost of erythropoietin per month 4000 INR to 10000 INR [28]. In 2012, total monthly cost of dialysis was 30,000 INR with cost of erythropoietin 7160 INR [29].
Limitation
This study sample was limited to only one government run and private hospital. Comorbidity details were not studied in detail. Larger sample size at different setting forms the future scope of this study.
Conclusion
In a developing country like India where a very small percentage of GDP is allocated for health, government run organizations fill up large lacunae in providing healthcare for the poor. To add up it’s the lower socioeconomically weak sections who do not have insurance coverage, nor they have sufficient information in selection of the hospital. Both private and government run hospitals provide optimum health care benefits to the patients of CKD. There exists no gender bias in the management of such patients in different set of hospitals. Infrequent follow ups among patients attending government run hospital show that they are less aware of the disease and available facility. They need to be educated towards the complications of the disease and appropriate management techniques that are provided even at government hospitals.
Chi-square test
Chi-square test
Chi-square test
Chi-square test
[1]. Jha V, Garcia-Garcia G, Iseki K, Chronic kidney disease: Global dimension and perspectivesLancet 2013 382:260-72. [Google Scholar]
[2]. Ojo A, Addressing the global burden of chronic kidney disease through clinical and translational researchTrans Am Clin Climatol Assoc 2014 125:229-46. [Google Scholar]
[3]. Snyder S, Pendergraph B, Detection and evaluation of chronic kidney diseaseAm Fam Physician 2005 72:1723-32. [Google Scholar]
[4]. Rajapurkar MM, John GT, Kirpalani AL, What do we know about chronic kidney disease in India: First report of the Indian CKD registryBMC Nephrol 2012 13:10 [Google Scholar]
[5]. Raman R, Ganesan S, Pal SS, Prevalence and risk factors for diabetic retinopathy in rural IndiaBMJ Open Diabetes Res Care 2014 2:e0000005 [Google Scholar]
[6]. Anupama YJ, Uma G, Prevalence of chronic kidney disease among adults in a rural community in South India: Results from the kidney disease screening (KIDS) projectIndian J Nephrol 2014 24(4):214-21. [Google Scholar]
[7]. Parker TF, Blantz R, Hostetter T, The chronic kidney disease initiativeJ Am Soc Nephrol 2004 15:708-16. [Google Scholar]
[8]. Agarwal SK, Dash SC, Irshad M, Raju S, Singh R, Pandey RM, Prevalence of chronic renal failure in adults in Delhi, IndiaNephrol Dial Transplant 2005 20:1638-42. [Google Scholar]
[9]. Singh NP, Ingle GK, Saini VK, Prevalence of low glomerular filtration rate, proteinuria and associated risk factors in North India using Cockcroft-Gault and Modification of Diet in Renal Disease equation: An observational, cross-sectional studyBMC Nephrol 2009 10:4 [Google Scholar]
[10]. Varma PP, Prevalence of chronic kidney disease in India - Where are we heading?Indian J Nephrol 2015 25(3):133-35. [Google Scholar]
[11]. Agarwal SK, Srivastava RK, Chronic kidney disease in India: Challenges and solutionsNephron Clin Pract 2009 111:c197-203. [Google Scholar]
[12]. Eiam-Ong S, Sitprija V, Co morbidities in patients with end-stage renal disease in developing countriesArtif Organs 2002 26(9):753-56. [Google Scholar]
[13]. Babitt JL, Lin HY, Mechanisms of anaemia in CKDJ Am Soc Nephrol 2012 23(10):1631-34. [Google Scholar]
[14]. Central Statistical Agency [Ethiopia] and ICF InternationalEthiopia demographic and health survey 2011 2012 Addis Ababa, Ethiopia and Calverton, Maryland, USACentral Statistical Agency and ICF International [Google Scholar]
[15]. Floege J, Johnson RJ, Feehally J, Comprehensive clinical nephrology 2010 4th edSt. LouiseElsevier Saunders [Google Scholar]
[16]. Ibrahim A, Momina M, Ahmed Kedir S, Bekele D, Clinical profile and outcome of patients with acute kidney injury requiring dialysis—an experience from a haemodialysis unit in a developing countryBMC Nephrol 2016 17:91 [Google Scholar]
[17]. Gray NA, Dent H, McDonald SP, Dialysis in public and private hospitals in QueenslandIntern Med J 2012 42(8):887-93. [Google Scholar]
[18]. Iseki K, Nakai S, Shinzato T, Nagura Y, Akiba T, Increasing gender difference in the incidence of chronic dialysis therapy in JapanTher Apher Dial 2005 9(5):407-11. [Google Scholar]
[19]. Albino BB, Balbi AL, Ponce D, Dialysis complications in AKI patients treated with extended daily dialysis: is the duration of therapy important?Bio Med Research International 2014 153626:1-9. [Google Scholar]
[20]. Caskey FJ, Wordsworth Ben T, De Charro FT, Delcroix C, Dobronravov VY, colsEarly referral and planned initiation of dialysis: what impact on quality of life?Nephrol Dial Transplant 2003 18:1330-38. [Google Scholar]
[21]. Winkelmayer WC, Owen W, Levin R, Avorn J, A propensity analysis of late versus early nephrologist referral and mortality on dialysisJ Am Soc Nephrol 2003 14:486-92. [Google Scholar]
[22]. Stack AG, Impact of timing of nephrology referral and pre-ESRD care on mortality risk among new ESRD patients in the United StatesAm J Kidney Dis 2003 41:310-18. [Google Scholar]
[23]. Jungers P, Massy ZA, Nguyen-Khoa T, Longer duration of predialysisnephrological care is associated with improved long-term survival of dialysis patientsNephrol Dial Transplant 2001 16:2357-64. [Google Scholar]
[24]. Hernandez AF, Greiner MA, Fonarow GC, Relationship between early physician follow-up and 30-day readmission among Medicare beneficiaries hospitalized for heart failureJAMA 2010 303:1716-22. [Google Scholar]
[25]. Sharma G, Kuo YF, Freeman JL, Zhang DD, Goodwin JS, Outpatient follow-up visit and 30-day emergency department visit and readmission in patients hospitalized for chronic obstructive pulmonary diseaseArch Intern Med 2010 170:1664-70. [Google Scholar]
[26]. Harel Z, Wald R, Bargman JM, Nephrologist follow-up improves all-cause mortality of severe acute kidney injury survivorsKidney Int 2013 83(5):901-08. [Google Scholar]
[27]. Swaminathan S, Mor V, Mehrotra R, Trivedi A, Medicare’s payment strategy for end-stage renal disease now embraces bundled payment and pay-for-performance to cut costsHealth affairs (Project Hope) 2012 31(9):2051-58. [Google Scholar]
[28]. Khanna U, The economics of dialysis in IndiaIndian J Nephrol 2009 19(1):1-4. [Google Scholar]
[29]. Jeloka TK, Upase S, Chitikeshi S, Monthly cost of three exchanges a day peritoneal dialysis is same as of thrice a week haemodialysis in self-paying Indian patientsIndian J Nephrol 2012 22(1):39-41. [Google Scholar]