Groin Flap in Paediatric Age Group to Salvage Hand after Electric Contact Burn: Challenges and Experience
Pradeep Gupta1, Rakesh Singh Tawar2, Manohar Malviya3
1Professor, Department of Plastic Surgery, Sawai Man Singh Medical College, Jaipur, Rajasthan, India.
2Resident, Department of Plastic Surgery, Sawai Man Singh Medical College, Jaipur, Rajasthan, India.
3Resident, Department of Plastic Surgery, Sawai Man Singh Medical College, Jaipur, Rajasthan, India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Rakesh Singh Tawar, Flat Numer-202, Blue Sky Apartment, Sarojini Marg, C Scheme, Jaipur-302001, Rajasthan, India.
E-mail: Rakesh.singh.tawar@gmail.com
Introduction
Electric contact burn is characterised by multiple wounds produced by entrance and exit of the current. Hand is most commonly involved in the same and children are particularly susceptible to such accidents.
Aim
To document effectiveness and challenges associated with the use of groin flap as an initial definitive treatment of electric contact burn in paediatric age group.
Materials and Methods
From January 2015 to December 2016, 25 children up to 12 years of age, who were admitted at SMS Medical College, Jaipur, Rajasthan, India, after electric burn injury with hand defect and who were treated by pedicled groin flap at the Department of Plastic and Reconstructive Surgery, were included in the study. Details related to gender, age, type of voltage injury, sites of injury and postoperative complications were recorded. The groin flap was used in these children for coverage of hand and finger defect with exposed bone and tendon.
Results
Normal functional results were seen in all children treated with pedicled groin flap and all were able to perform activities of daily living. All the children had satisfactory aesthetic result.
Conclusion
Although, groin flap was an uncomfortable procedure due to limb position that was particularly difficult for children, it was found to be a useful method to salvage hand and it resulted in favourable functional and aesthetic outcome in each case.
Electrical injuries, Pedicled flap, Voltage injury
Introduction
Electrical injuries in children though less common than in adults, account for between 2–10% of all burns admissions worldwide [1-4]. Inserting objects into the outlets, biting cords, contacting household wires or faulty appliances are the major causes of low voltage injury in children [1,3,5]. High voltage electrical injuries have been caused by exposure to power lines through misadventure in adolescents or from lightning strikes [1-3,6]. They are the most frequent cause of amputation in burn services [7].
The hands are frequently involved in Electrical burn accidents [7]. The Optimal treatment of severe burns on hand is very important as they may result in significant functional impairment. Severe burn, especially on the dorsum of hand where the skin is thin with little underlying subcutaneous tissue, is often not amenable to skin grafting due to exposed bone and tendon. When this situation arises, flap coverage is required.
Groin flap based on the superficial circumflex iliac artery was described in 1972 by McGregor et al., [8]. Superficial circumflex iliac artery is a long course artery, which defines the groin flap as an ‘axial pattern flap’. The vessel arises from the femoral artery about 2 cm distal to the inguinal ligament. Design of the flap is an ellipse, the long axis of which is the presumed course of the artery. In the lateral part (distal portion of the flap), the elevation is very quick and easy and should not include the aponeurosis of the muscles which are attached deeply by fibrous septa. The lateral border of sartorius must be identified. The elevation can stop at this level. The aponeurosis of sartorius is incised to be included in the flap; it protects the origin of the vascular pedicle [9].
The purpose of this study was to evaluate the outcome of paediatric electric hand burn injuries that were covered by pedicled groin flap and its usefulness in the era of ever increasing use of free flaps.
Materials and Methods
This was a prospective therapeutic study conducted in the Department of Plastic Surgery, SMS Medical College Jaipur. All children of age group 1 to 12 years admitted in the Department from January 2015 to December 2016 for electric burn injury of hand were included in the study. Patients having associated head injury and concomitant injury to groin region were excluded from the study. Details related to gender, age, type of voltage injury and site of injury were recorded. All cases were initially managed by intravenous fluid resuscitation and dressing of the wound with silver sulfadiazine. Cardiac monitoring for electrocardiographic changes was done in all patients for 48 hours from admission. All non viable and poorly vascularized tissues were debrided and Kirschner wire fixation was used for stabilization of digits. The groin flap was used in these children for coverage of hand and finger defect with exposed bone and tendon. Marking of groin flap was done and the flap was raised according to the size of defect and insetted over the defect with ethylon 3-0 reverse cutting suture. The donor site was closed primarily in two layers. The position of limb was maintained by using adhesive bandages. Patients were admitted on an average for five days postoperatively, during which they were monitored for development of any postoperative complications like infection, flap necrosis and after discharge, patients were again reviewed on day 21 for flap adherence to the recipient bed. Detachment and insetting were done on the same day. All patients were operated in general anaesthesia. Functional outcome was assessed in all patients with respect to the ability to use hand for eating, drinking, writing, and dressing. Aesthetic satisfaction assessment was done during follow up using an ordinal scale. The study was approved by the Institutional Ethics Committee and was performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and all its later amendments. Informed consent from patient’s guardian was obtained, wherever applicable. Details of patients, investigations, operative procedures and photographs were collected.
Results
Pedicled groin flap was used in 25 paediatric patients aged between 5 to 12 years (mean = 9) with electric contact burn; out of which 21 (84%) were male and 04 (16%) were female.
[Table/Fig-1] shows the distribution of patients according to the type of voltage injury. Low voltage (<1000 volts) electric burn was seen in 20 patients. All low voltage injuries occurred indoor due to contact with the household wires.
Distribution of cases according to mode of electric injury.
| Voltage | Number of patients (percentage) |
|---|
| Low | 20 (80%) |
| High | 05 (20%) |
High voltage injury (>1000 volts) was seen in five patients due to exposure to high voltage power lines.
[Table/Fig-2] shows the various areas of hand involvement in the patients. In this study, 10 patients had injury to the dorsum of hand and eight patients had wrist injury. Right hand was more commonly involved. Associated minor injuries of other areas were managed conservatively with silver sulfadiazine dressing.
Distribution of cases according to area involved.
| Area involved | Number of patients | Percentage |
|---|
| Dorsum of hand | 10 | 40% |
| Palmer surface | 2 | 8% |
| Fingers | 1 | 4% |
| Thumb | 4 | 16% |
| Wrist | 8 | 32% |
The maximum length of flap used for resurfacing hand defect in this study was 12 cm while the minimum length was 5 cm which was used for coverage of degloved thumb.
While complete flap necrosis was not seen in any of the cases in the study, two patients had partial flap necrosis. Donor site dehiscence was seen in two patients. Another two patients had seropurulent discharge from the recipient site that was managed conservatively and did not result in adverse outcome except for delayed detachment and insetting in such patients [Table/Fig-3].
Distribution of cases according to postoperative complication.
| Complication | Number of patients | Percentage |
|---|
| Complete flap necrosis | nil | 00% |
| Partial flap necrosis | 02 | 08% |
| Donor site dehiscence | 02 | 08% |
| Recipient site infection | 02 | 08% |
The only complain was of pain that was managed by simple analgesics. Bulkiness of the flap at the recipient site was another problem faced in five cases for which thinning of the flap was done after the detachment, in one or two settings.
Functional outcome in all the patients assessed during follow up showed that all had satisfactory outcome in terms of ability to use hand for eating, drinking, writing and dressing. All parents of the children rated aesthetic outcome as satisfactory during follow-up visit.
Discussion
The groin flap is an old and reliable flap that has been used for soft tissue defects. Because of the constant landmarks and an axial blood supply, groin flap is easy to harvest [9]. In patients with electric burn of hand, the use of groin flap for coverage is an excellent choice due to the fact that the donor area is spared and relatively healthy in such patients. Moreover, free flaps are not a good option in such patients since the area may be devoid of recipient vessels for anastomosis in acutely burned hand [10].
Male preponderance noted in the study is similar to other studies of paediatric burn [1,2,5,11]. Maximum cases were of low voltage injury indicating that most children were exposed to electric injuries in their house by the indoor appliances and wires that can be prevented by providing a safer and vigilant environment to children at home [1,3] [Table/Fig-2]. Similar results were found by other authors [1,2,12]. Wallace BH et al., in their study concluded that majority of paediatric electric burns were due to low voltage household electric appliances specially in young patients [5]. Similar results were seen in the study of Katherine LT et al., in which mean age was 7.6 years and 30% patients required surgical management [13], while in the study of Lui P et al., 61% children with burn were managed surgically and they concluded that electric burn causes significant morbidity in children [11].
In this study, groin flap was used as a method of reconstruction in the ‘difficult to manage’ paediatric cases of electric contact burn of hand. The main challenge was maintenance of limb position in children till the time of detachment for which explanation of the importance of positioning of limb for flap attachment and reassurance to the family members was required for cooperation [Table/Fig-4,5]. Elastic adhesive bandages were used for holding the limb in position. Infection and flap necrosis are the usual known complications encountered in groin flap. In this study, seropurulent discharge was found in two cases which were easily managed by regular dressing and antibiotics. Complete flap necrosis was not seen in any patient though partial necrosis occurred in two cases for which timely debridement and advancement of flap was done. The donor site was closed primarily in all cases, which required flexion at hip and knee joint in four patients. Donor site dehiscence occurred in two patients which was managed by secondary closure at the time of flap detachment and insetting. The results of our study are comparable to other studies conducted by authors for the use of groin flap for closure of hand defect in adult patients, though there is scarcity of reports in paediatric age group [14-16].
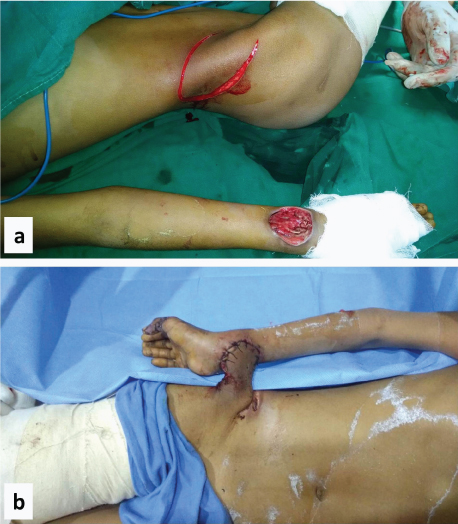
Eleven-year-old male child with right sided electric burn wrist defect covered by groin flap: a) Preoperative picture of electric burn defect over right wrist with groin flap marking; b) postoperative picture of defect after insetting of flap.
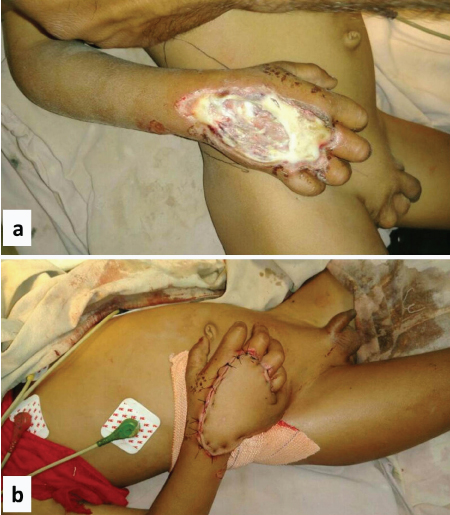
Seven-year-old male child with electric contact burn defect on dorsum of right hand; a) Pre-operative picture showing exposed tendon and bone (Post burn day 07)
b) Groin flap inset is performed on the defect and the hand is kept in comfortable position.
Extensive electrical burn may create a wide zone of injury making local flaps unreliable. Free tissue transfer may not be possible due to the inability of a sick patient to tolerate a multi hour surgical procedure, or due to the non availability of microsurgical expertise or equipment. In these circumstances, pedicled flaps derived from uninjured distant tissue provide an alternative method for hand soft tissue coverage.
Limitation
A short postoperative follow up period is a limitation of this study as the longer follow-up would confirm or refute the results over time.
Poor vascularity in the recipient area, post burn, precluded the use of free flap for coverage in our study. The authors recommend further studies in paediatric patients for comparison of pedicled groin flap with free flap whenever available.
Conclusion
Groin flap is an excellent option available in armanterium of plastic surgeon when there is a doubt of donor site vascularity for free flap. Despite of long hospital stay, uncomfortable position and number of operations, results obtained from groin flap are assured and satisfactory. The pedicled groin flap is thus a safe and effective method to salvage hand function of children.
[1]. Celik A, Ergun O, Ozok G, Paediatric electrical injuries: A review of 38 consecutive patientsJ. Paediatr. Surg 2004 39(8):1233-37. [Google Scholar]
[2]. Zubair M, Besner GE, Paediatric electrical burns: Management strategiesBurns 1997 23(5):413-20. [Google Scholar]
[3]. Robinson M, Seward PN, Electrical and lightning injuries in childrenPaediatr Emerg Care 1986 2:186-90. [Google Scholar]
[4]. Fordyce TA, Kelsh M, Lu ET, Sahl JD, Yager JW, Thermal burns and electrical injuries among electric utility workers 1995–2004Burns 2007 33(2):209-20. [Google Scholar]
[5]. Wallace BH, Cone JB, Vanderpool RD, Bond PJ, Russell JB, Caldwell FT, JrRetrospective evaluation of admission criteria for paediatric electrical injuriesBurns 1995 21(8):590-93. [Google Scholar]
[6]. George EN, Schur K, Muller M, Mills S, Brown Tl, Management of high voltage electrical injury in childrenBurns 2005 31(4):439-44. [Google Scholar]
[7]. Bajaj SP, Sarabahi S, Electrical burnsPrinciples and practice of burn care. 21 2010 IndiaJaypee:276-85. [Google Scholar]
[8]. McGregor IA, Jackson IT, The groin flapBr J Plast Surg 1972 25(1):3-16. [Google Scholar]
[9]. Koshima I, Mardini S, Wei FC, Wei FC, Mardini S, Groin flap and superficial circumflex iliac artery perforator flapFlaps and reconstructive surgery 2009 27Elsevier Inc:358-66. [Google Scholar]
[10]. Hettiaratchy S, Papini R, ABC of burns: Initial management of a major burn: II-assessment and resuscitationBMJ 2004 329(7457):101-03. [Google Scholar]
[11]. Lui P, Tildsley J, Fritsche M, Kimble RM, Electrical burns in childrenJ Burns and Surg wound care [Serial online] 2003 2(1):8 [Google Scholar]
[12]. Rai J, Jeschke MG, Barrow RE, Herndon DN, Electrical injuries: A 30-year reviewJ Trauma Inj Infect Crit Care 1999 46(5):933-36. [Google Scholar]
[13]. Katherine LT, Andrew JA, Electrical burn injuries in childrenJournal of Paediatrics and Child Health 2008 44:727 [Google Scholar]
[14]. Choi JY, Chung KC, The combined use of a pedicled superficial inferior epigastric artery flap and a groin flap for reconstruction of a dorsal and volar hand blast injuryHand (NY) 2008 3(4):375-80. [Google Scholar]
[15]. Brooks TM, Jarman AT, Olson JL, A bilobed groin flap for coverage of traumatic injury to both the volar and dorsal hand surfacesCan J Plast Surg 2007 Spring15(1):49-51. [Google Scholar]
[16]. Ole G, Nicolai K, Adrien D, Tobies H, Heinz HH, Lars S, The effectiveness of pedicled groin flaps in the treatment of hand defects: Results of 49 patientsThe Journal of hand surgery 2012 37(10):2088-94. [Google Scholar]